Part 4: How Infection Control is Organised and Managed
- Introduction
- Roles and Responsibilities for Infection Control
- Planning Infection Control Activities
- Financial Management of Infection Control
- Staffing Infection Control
- Assurance about the Quality of Infection Control Systems and Practices
Introduction
4.1
Hospital managers are responsible for ensuring the safety of patients and staff. Protecting them from infection is an important element of this responsibility. In this part we examine the following components of providing an effective infection control service:
- assigning roles and responsibilities for infection control throughout the hospital, with clear lines of accountability and delegation;
- planning infection control activities through work plans or programmes;
- ensuring good financial management of infection control activities;
- ensuring that infection control activities are appropriately staffed; and
- obtaining assurance about the quality of infection control systems and practices.
Roles and Responsibilities for Infection Control
4.2
In each DHB hospital service43:
- Policy and operational infection control responsibilities should be clearly assigned.
- All managers should be alert to the infection control implications of their work.
- There should be a well-established infection control team.
Survey Responses on Responsibilities for Managing Infection Control
4.3
In our survey we asked whether:
- each hospital service had an infection control team and how long it had been operating; and
- executive, clinical, and risk managers had infection control responsibilities.
4.4
All hospital services had an infection control team, with only one having been operating for less than five years.44
4.5
In all hospital services, infection control policy was a responsibility of the infection control committee (see paragraphs 5.6-5.14 on pages 102-105) and the infection control team, supported by hospital managers and/or the risk manager.45 However, not all relevant hospital managers had infection control responsibilities. Notably, in seven hospital services, the Medical Director (and in three the Director of Nursing) had no responsibility for infection control policy, despite being the hospital service’s clinical leader.46
4.6
Responsibility for operational infection control rested with the infection control team, along with the infection control committee and the General Manager.47 Only nine hospital services identified their risk manager as having any infection control responsibility. Risk managers need to be aware of recurring and significant safety matters (such as infection) in order to be able to report to the District Health Board (DHB) and the Ministry of Health on the management of non-financial risks.
Conclusions
4.7
Infection control responsibilities were appropriately allocated to a range of clinical staff and managers, although some hospital services did not give responsibilities to all relevant managers.
4.8
In those hospital services where the Medical Director and/or the Director of Nursing had some responsibility for infection control, the policies, procedures, and practices to prevent and control infection were more likely to receive full clinical support.
4.9
Assigning some responsibility for infection control to risk managers should ensure they are in a position to take a comprehensive view of this aspect of patient safety, in the context of risk management and quality assurance throughout the hospital.
| Recommendation 11 |
|---|
| Hospital services should ensure that all relevant hospital managers are assigned infection control responsibilities – including clinical leaders and managers with responsibility for risk management and quality assurance. |
Planning Infection Control Activities
4.10
Infection control activities are wide ranging (see Parts Six, Seven, and Eight on pages 127-180). Reflecting the breadth of activity, an infection control programme should outline:
- what infection control issues the hospital service is facing (drawing on the results of the past year’s activities);
- how the infection control team proposes to perform its functions; and
- the infection control team’s strategies and priorities.
Survey Responses on the Content and Implementation of Infection Control Programmes
4.11
We asked about the content of infection control plans or programmes, and how often progress against them was assessed.
4.12
Figure 6 (on the next page) illustrates the content of hospital services’ infection control programmes in terms of seven sets of information that we expected the programmes to address. Most included five of the seven. The other two – the infection control team’s input to setting standards and its input to audits of clinical support services – featured in just under half of the programmes.
Figure 6
What Did the 2000-01 Infection Control Programme Contain?48
| Did the Infection Control Programme Contain: | Yes | No |
|---|---|---|
| A list of policies requiring implementation or update? | 18 | 3 |
| Details of categories of staff requiring training or education? | 17 | 4 |
| Details of surveillance activities to be carried out? | 21 | 0 |
| Details of aspects of hospital hygiene to be monitored? | 18 | 3 |
| Plan/timetable for audit of infection control activities? | 19 | 2 |
| Details of infection control team’s input into setting standards? | 10 | 11 |
| Details of infection control team’s input to audits of clinical and support services? | 10 | 11 |
4.13
One particularly comprehensive infection control programme identified the following key areas of emphasis for infection control in the coming year:
- reviewing infection control policies;
- considering compliance and auditing requirements to meet the Standard;
- finalising a programme for safe re-use of medical devices;
- providing ongoing education and awareness training for people working in the hospital service;
- contributing to the design of new health care facilities; and
- enhancing access to corporate information for surveillance and analysis.
4.14
Many infection control activities follow cycles, and need to be planned to make it possible to interpret data and trends over time. However, only seven hospital services had a documented long-term strategy for infection control beyond 12 months.49
4.15
Most respondents reported that they assessed the progress of their infection control programmes at least annually.50
Conclusions
4.16
Most infection control programmes covered those areas we expected them to address, but we were concerned that fewer than half of the programmes specified how the infection control team should contribute to setting standards in clinical and support services, or identified planned audits of the services. Parts Five and Six on pages 99-150 look at why these matters are important.
4.17
Long-term planning (more than a year) is important in the context of meeting the Infection Control Standard by October 2004, but few hospital services were undertaking long-term planning of infection control.
| Recommendation 12 |
|---|
| Hospital services should make long-term plans for infection control in the context of meeting the Infection Control Standard by October 2004. |
Financial Management of Infection Control
4.18
We asked about funding and budgeting for infection control, and monitoring of expenditure.
Survey Responses on Funding and Budgeting for Infection Control
4.19
An infection control programme can be funded discretely or as one component of a larger budget. Different approaches have their benefits and drawbacks in terms of priorities for resource use, transparency, independence, and capability.
4.20
We asked:
- how the infection control programme was funded;
- what was budgeted for and spent in the 2000-01 financial year and what was budgeted for in 2001-02; and
- whether infection control budgets had changed between 1999-2000 and 2000-01 and between 2000-01 and 2001-02.
4.21
Twelve hospital services had a separate infection control budget and were able to provide a breakdown of their infection control team’s costs.51 Based on that data and the staff resources reported by all the survey respondents, we estimate that some $2.7 million is spent directly on infection control programmes by public hospital services each year.
4.22
Infection control personnel are commonly engaged in a range of activities, and infection control work can compete with clinical and other duties. Establishing a discrete budget for infection control is one means of ensuring that resources are not eroded by competing priorities – or at least indicates to managers when priority choices have to be made. Nine respondents told us that a separate budget helped them to manage infection control activities.52 Conversely, one of the respondents without a separate budget commented that having no discrete budget made it more difficult to make a case for additional resources.
| "… Because everything gets lumped in together it can be difficult to make a case for extra funds. Discrete budget would help … " |
4.23
More than three-quarters of hospital services reported that their infection control budget had remained the same or increased in the past two years.53 Four said it had declined in 2000-01 and three said it had declined in 2001-02.
4.24
Publication of the Standard – see paragraph 2.27 on page 46 – appeared to have had little effect on the amount of resources allocated to infection control. However, four hospital services had allocated more resources to meet the Standard.54
| [Effect of the Infection Control Standard] "...Infection control has a higher focus and priority, education for practitioners and staff has been increased, and resources to undertake duties have been improved … " |
Survey Responses on Monitoring of Infection Control Expenditure
4.25
We would expect hospital General Managers (or their equivalent – for example, where responsibilities are delegated in a large DHB) to exercise a degree of oversight on resources applied to and money spent on infection control. However, the General Managers of only seven hospital services reported that they received regular reports from the infection control team on expenditure in managing hospital-acquired infection.55 Five of these teams reported this information at least every six months. Eleven were not reporting infection control expenditure.
4.26
Limited reporting on expenditure is likely to reflect the fact that:
- not all hospital services have a separate budget for infection control;
- expenditure on infection control activities is low compared with expenditure on other hospital activities;
- the costs of controlling individual outbreaks (which can be considerable) are often not known, being hidden in other hospital budgets; and
- for some infection control services there is no obligation to report formally on their activities.
Conclusions
4.27
In hospital services without a separate budget for infection control, it is more difficult for managers to oversee and manage the resources dedicated to infection control. The money spent on infection control does not have a high profile with senior managers in many hospital services.
| Recommendation 13 |
|---|
| Hospital services should consider establishing separate infection control budgets, having regard to the benefits and drawbacks in terms of priorities for resource use, transparency, independence, and capability. |
| Recommendation 14 |
|---|
| Hospital General Managers (or their equivalent) should monitor resources applied to infection control. |
Staffing Infection Control
4.28
The number of staff – including clerical staff – required to support an effective infection control programme will depend on the size and type of hospital, the services it delivers, and the population it serves. Infection control staff need to be able to carry out a wide variety of tasks, including:
- drawing up policies and procedures for infection control;
- providing advice, and monitoring and auditing the application of the policies and procedures;
- undertaking surveillance to detect hospital-acquired infections; and
- training other staff and raising their awareness of infection control issues within the hospital service.
4.29
Infection control teams are normally made up of hospital nursing and medical staff with the necessary training and skills. Skills and expertise not available within the hospital should be contracted in.
4.30
Our survey included questions about:
- the people and time dedicated to infection control;
- problems relating to resourcing of infection control;
- qualifications and training of infection control staff; and
- clerical support for infection control.
Survey Responses on People and Time Dedicated to Infection Control
4.31
We asked about:
- numbers of infection control practitioners and doctors with infection control responsibilities56; and
- whether there had been difficulties in recruiting infection control practitioners and/or doctors over the past two years and, if so, why.
4.32
We also asked infection control practitioners and doctors to:
- estimate the proportion of time they spent on different infection control activities;
- specify an ideal proportion of time they would wish to spend on these activities; and
- estimate how infection control practitioner and doctor time was divided between infection control work within and outside the DHB hospital service.
4.33
In more than two-thirds of hospital services, the number of infection control practitioners (in terms of full-time equivalent staff) had either increased or stayed the same in the previous two years.57 Respondents reported a similar profile for infection control doctors over the same period.58
4.34
The ratio of occupied beds59 per infection control practitioner in each hospital service ranged from 114:1 to 365:1 (see Figure 7).
Figure 7
Ratio of Occupied Beds per Infection Control Practitioner at 1 July 200160
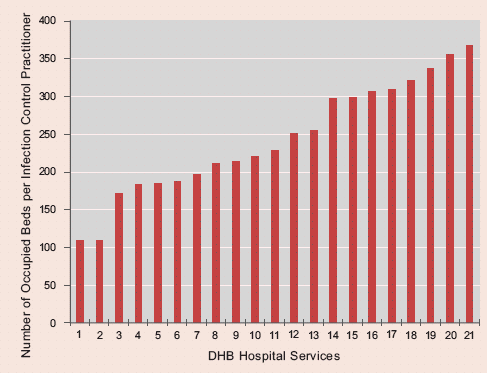
4.35
We expected the larger hospital services with tertiary61 hospitals to have the highest ratio of infection control practitioners because these hospitals tend to:
- have high demand for beds and high throughput of patients; and
- carry out the most complicated operations and medical procedures for the most vulnerable categories of patient.
4.36
However, this expected pattern was not reflected in the survey results. We return to this matter in paragraphs 4.52-4.56 on page 91.
4.37
Employing infection control practitioners and infection control doctors can provide continuity and an infection control presence in the hospital. In most hospital services these staff are employees rather than contractors:
- in 17 hospital services, all infection control practitioners were employees62;
- in 15 hospital services (not all of which were included in the 17) all infection control doctors were employees; and
- the other six services assigned some responsibility to consultant doctors contracted to provide infection control expertise.63
4.38
In one small hospital service, both the infection control practitioner and the infection control doctor were contracted in. However, an infection control presence in the hospital was maintained by the employment of a nurse with infection control responsibilities.
4.39
The survey responses indicated that infection control practitioners spent most of their time working within DHB hospitals.64 Eight infection control teams reported65 that they performed an infection control role of some kind in the community. This role commonly involved providing advice, education, and other support to health care providers in the community and other agencies. Such services are valuable, but place additional demands on infection control practitioners, leaving less time available for work in the hospital.
| "… Education and support is given to private hospitals for older persons and to residential care facilities. This extension is viewed as support for our community and is about prevention …" |
4.40
In all hospital services, infection control doctors reported spending a relatively small proportion of their time on infection control tasks.66 One service with a tertiary hospital reported that the infection control doctor spent 19.5 hours a week on infection control matters. Most infection control doctors in other hospital services spent considerably less time than this on infection control.
4.41
We compared the proportion of time that infection control practitioners and doctors spent on different infection control activities with the proportion they felt they should ideally spend. This comparison revealed no major discrepancies.67 However, most practitioners and doctors had been unable to undertake all their planned hours of continuing education for the period January 2001 to January 2002.68
| "… Education and policies/procedures [are] very important to verbally back/educate infection control practitioners and procedures. Surveillance [is] extremely important to identify and report relevant infections to improve practice, etc. Audits are also important to validate infection control practices are being performed and where improvements can be made… " |
4.42
Figure 8 below shows the results of our analysis of how hospital services’ infection control practitioners spent their time.69
Figure 8
What Proportion of Time (%) Do Infection Control Practitioners Spend on Different Infection Control Activities?
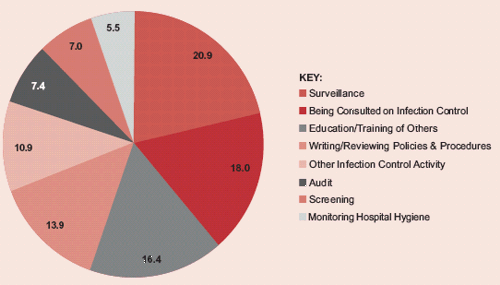
4.43
On average, in 2000-01, in all the hospital services:
- the three largest proportions of time were spent on surveillance (20.9%), responding to consultation by other staff (18.0%), and educating and training other staff (16.4%); and
- only 5.5% and 7.4% of time respectively was spent on monitoring hospital hygiene and audit – which means that only a relatively small amount of time was being spent on checking that infection control policies and procedures were actually being applied.
4.44
There were wide differences between hospital services in the proportion of time spent on some infection control activities. The widest variation was in the amount of time spent on surveillance – one hospital service reported 60% of practitioner time spent on surveillance, while some others reported much less. (Part Seven on pages 151-172 examines the need for surveillance and the factors that might be expected to influence the amount of time that infection control practitioners spend on this activity.)
4.45
Time spent on monitoring hospital hygiene and on audit also varied markedly. One hospital service reported that its infection control practitioners spent 20% of their time on these two activities, while another reported that they spent no time on them. Part Six on pages 127-150 examines these activities.
4.46
The equivalent results for the proportion of medical time spent on infection control activities70 were difficult to interpret. Six hospital services did not provide a response because the medical input was small and/or contracted in, and they felt unable to accurately assess the proportion of time spent on the various activities. A few responses suggested that most of the medical time would be spent giving advice.
4.47
Our analysis of the results of the 15 hospital services that provided useful data showed that, on average, more than 40% of doctor time71 was spent on responding to requests for infection control advice. Audit took up an average of only 6% of doctor time. As for infection control practitioners, there was a wide range of responses – from no time spent on audit in six hospital services to between 2% and 24% in the rest.
4.48
Few respondents to our survey reported problems recruiting doctors or infection control practitioners over the previous two years.72 However, a small number referred to reluctance among doctors to work in infection control, which some see as a low profile role.73 Some staff raised the same issue with us during our visits.
| Recommendation 15 |
|---|
| Hospital services should review the way in which infection control staff spend their time, to ensure that key activities – such as surveillance, monitoring hospital hygiene, and audit – receive the appropriate attention. |
Survey Responses on Access to Information Technology
4.49
We asked whether infection control teams used computerised systems for recording and analysis to help manage their activities. Ten infection control teams had their own computerised systems.74 Standard forms are commonly used75, with data often entered manually into a computer.76 As outlined in paragraphs 7.37-7.41 on pages 162-163, access by infection control teams to hospital information systems is generally satisfactory.
Survey Responses on the Key Issues Relating to Resourcing of Infection Control
4.50
We identified, from our preliminary work, the main problems that hospital services might experience in resourcing infection control. The two factors most often selected in the survey responses both related to available staff time rather than material resources. Respondents reported that:
- doctors had too little time available for infection control77; and
- infection control staff were unable to keep up to date with developments in infection control78.
4.51
Three of the six hospital services with tertiary hospitals expressed concern about the amount of doctor time available for infection control work. Four of the six were concerned about lack of time for ongoing education of infection control staff. These comments indicated that infection control staff might be facing work pressures.
4.52
In addition, two of the six hospital services with tertiary hospitals reported that they needed more infection control practitioners.79
4.53
Many hospital services take account of bed numbers when assessing the number and type of staff required for infection control. However, few systematically consider how intensively the beds are used – i.e. the numbers of patients moving through the hospital as inpatients, day patients, and outpatients. Intensity of bed use, and a number of other factors, have a bearing on the risk of hospital-acquired infection, and therefore need to be considered in making decisions about infection control staffing. The other factors include:
- the complexity of medical and surgical procedures and associated technology; and
- patients’ state of health and to what extent their treatment makes them more vulnerable to infection.
4.54
The absence of any clear relationship between staffing of infection control and the type of hospital service (see Figure 7 and paragraph 4.35) suggests that assessments of staff requirements may not be taking sufficient account of how factors relating to the type of services provided affect the risk of hospital-acquired infection.
4.55
Measuring the benefits of expenditure on infection control is difficult. Evidence of positive outcomes is needed to support a reliable assessment. Nevertheless, some international research has shown that expenditure on infection control activities can produce substantial savings.80
4.56
One hospital that we visited had produced a business case seeking additional infection control staff. It estimated that almost $4 million could be saved each year through an expenditure of $170,000. Based on a conservative estimate of hospital-acquired infection rates, the hospital estimated that it would save (in bed occupancy costs) at least 15 times what it would spend on additional infection control resources. The business case was accepted.
| Recommendation 16 |
|---|
| In consultation with the Ministry, DHBs and hospital services should design a model to help determine the appropriate level of resources applied to infection control. The model should take account of all relevant factors – such as bed numbers, bed occupancy, complexity of medical and surgical procedures and associated technology, and patient mix. |
Survey Responses on Qualifications and Training of Infection Control Staff
4.57
Infection control staff need a wide knowledge of health care and medical disciplines, as well as microbiology and infectious diseases. Refresher training and continuing education are important to ensure that infection control staff are kept up-to-date with new developments.
4.58
We asked about the specialty of doctors with infection control responsibilities and the qualifications of infection control practitioners. We also asked whether infection control staff had the means to keep up-to-date with developments in the theory and practice of infection control.
4.59
Fourteen hospital services employed or contracted the services of individual doctors with a relevant clinical background to carry out infection control activities. In most cases they were infectious disease physicians or clinical microbiologists.81 In the remaining cases, the infection control services were supported by doctors with an interest in infection control and/or by doctors engaged through DHB and private laboratory contracts.
4.60
Of the 52 infection control practitioners represented in the survey, all had some form of nursing or midwifery registration.82 Almost all had undertaken or were undertaking some recognised infection control education.
4.61
Infection control practitioners had, on average, about six years’ experience, but the extent of experience differed markedly between hospital services. For example, one had no infection control practitioners with more than one year’s experience, while around a quarter of the infection control practitioners had 12 years’ experience or more.
4.62
Newly employed infection control staff should have access to information that explains the role of the infection control team, hospital policies and procedures, and relationships with other parts of the organisation. One hospital service had produced a comprehensive orientation handbook for infection control practitioners, which provided helpful information and guidance in an accessible format.
4.63
Infection control practitioners had good access to material such as journals and infection control texts, providing them with the means to keep abreast of developments in infection control theory and practice.83
Survey Responses on Clerical Support
4.64
Infection control typically involves large amounts of data entry and communication. To do this work cost-effectively, infection control practitioners need clerical support.
4.65
We asked infection control teams how much clerical support was provided for infection control practitioners and doctors. We also asked whether the clerical support was adequate.
| "… We don’t have enough time to do all the infection control activity we think is needed so having to spend time on clerical work (not our specialty) is frustrating and inefficient … " |
4.66
Most infection control teams were not allocated any dedicated clerical support.84 Only three of the 20 infection control teams that responded considered the level of support to be adequate for both infection control practitioners and doctors.85 Responses included comments that86:
- clerical support had to be negotiated as necessary, with the result that infection control work could be given low priority; and
- clerical tasks – such as data entry, photocopying, mail outs, and typing – consumed the time of infection control practitioners at the expense of core activities such as surveillance.
4.67
A comment by the infection control team at one large hospital is an illustration of what was commonly seen as a resourcing problem:
There is one secretary to provide services for the Director of Microbiology, second microbiologist, 35 technical staff, a scientific officer, the vaccination clinic as well as infection control.
Conclusions
4.68
Overall, our findings painted a picture of a fairly stable and appropriately experienced infection control workforce. Clerical support for infection control is not adequate, and infection control staff were spending time on clerical work. This is not a good use of their skills and experience.
4.69
Some of the data from our survey (for example, the widely variable staff/bed ratio and the relatively little time spent in some hospital services on auditing compliance with infection control procedures) and the views from our survey respondents and people we met during visits, suggest that the human resources applied to infection control may not be sufficient in some hospital services.
4.70
Health and cost benefits may be gained from hospital services periodically reviewing their requirements for infection control resources, and increasing the resources where such additional expenditure is shown to be cost-effective.
| Recommendation 17 |
|---|
| Hospital managers should consider assigning additional clerical support to infection control practitioners, thereby leaving the practitioners free to carry out the wide range of tasks that require their infection control expertise. |
| Recommendation 18 |
|---|
| Hospital services should periodically review whether their infection control resources are adequate, and look for ways of increasing resources where such additional expenditure is shown to be costeffective. |
Assurance about the Quality of Infection Control Systems and Practices
4.71
Two related processes provide important assurance to hospital managers about the quality of infection control systems and practices:
- undertaking voluntary accreditation to demonstrate adherence to specific standards of good practice; and
- meeting the Standard in order to gain certification under the Health and Disability Services (Safety) Act 2001.
Survey Responses on Voluntary Accreditation
4.72
Voluntary accreditation provides independent assurance that a health service meets a recognised set of clinical and managerial standards. The Ministry has encouraged all DHBs to seek accreditation of their hospital services to help prepare for certification (paragraphs 2.21-2.23 on pages 44-45). We therefore expected all to have achieved accreditation, or to be actively taking part in an accreditation scheme. We asked whether hospital services had taken part in any accreditation scheme, and whether the scheme covered infection control.
4.73
Most hospital services were taking part in a voluntary accreditation scheme.87 In 18 hospital services the accreditation had included aspects of infection control.88 In more than half of hospital services, some or all hospitals within the service had achieved accreditation.89
4.74
Hospital services commented positively on the impacts of the accreditation surveys, noting that they reinforced good practice and identified areas for improvement – prompting the introduction of targeted action plans and ongoing reviews.
| [How accreditation helps patients] "...Patients are given relevant information regarding their infection … " |
Survey Responses on Compliance with the Infection Control Standard
4.75
Hospitals will need to demonstrate that they meet the Standard in order to be certified. An accompanying workbook90 provides an audit tool for organisations to evaluate their practices and procedures against the outcomes required by the Standard.
4.76
We asked whether:
- the Standard was used to provide guidance when infection control arrangements were being considered;
- the hospital service also used the infection control audit tool; and
- publication of the Standard and audit tool led to changes in infection control resources.
4.77
In all but one of the responses, hospital managers reported that they always used the Standard for guidance when considering infection control arrangements.91 Only eight infection control teams responded that they were using the audit tool.92
4.78
The audit tool represents a valuable source of guidance, and infection control teams using it reported that the audit tool93:
- helped them to review infection control policy;
- could be used for internal audits of infection control and for accreditation; and
- recommended surveillance requirements that prompted a review of workload and resources and led to changes in the composition of the infection control team.
Conclusions
4.79
Most hospital services have sought voluntary accreditation in preparing for certification by October 2004 and they have found the accreditation process helpful in improving practice.
4.80
The Standard is proving to be a valuable resource for hospitals in planning and implementing infection control.
4.81
There was only limited application of the infection control audit tool. It is possible that some hospital staff may not be aware of the audit tool and its value as a source of guidance.
| Recommendation 19 |
|---|
| Hospital managers and staff should make use of the infection control audit tool (published by Standards New Zealand as a companion document to the Infection Control Standard). |
43: The term hospital service refers to that part of the DHB delivering services in a hospital setting within the DHB.
44: F2: Q4.
45: F2: Q2, A.
46: F2: Q2, A.
47: F2: Q2, B.
48: F3.3: Q2.
49: F3.3: Q7.
50: F3.3: Q3.
51: F3.4: Q2.
52: F3.4: Q7a.
53: F3.4: Q10, A, B – respondents made estimates where precise figures were not available.
54: F3.4: Q18 & Q20.
55: F2: Q5, a.
56: These doctors are generally microbiologists and/or infectious disease specialists who are responsible for a range of services in the hospital, including infection control. We refer to them as “infection control doctors”, but infection control is only one of a number of activities in which they are involved. An infection control practitioner is usually a registered nurse with appropriate training and skills in infection control.
57: F3.2: Q8, a.
58: F3.2: Q8, b – five respondents did not complete this question.
59: Bed occupancy is a measure of the amount of time that hospital beds contain patients – as opposed to lying vacant until the next patient that needs the bed is admitted.
60: F3.2: Q4; F1: Q4, a.
61: We use the term tertiary to refer to those DHB hospitals providing very specialised care and performing the most complex procedures. These services are predominantly delivered by the DHBs based in major cities.
62: F2: Q7a.
63: F2: Q8a.
64: F3.2: Q4.
65: F2: Q9.
66: F3.2: Q7.
67: F3.2: Q2, A, B & D; Q5, A, B & D.
68: F3.2: Q20.
69: F3.2: Q2, A.
70: F3.2: Q5.
71: Full-time equivalent – none of the doctors worked full time on infection control.
72: F3.2: Q10 & Q13.
73: F3.2: Q16.
74: F3.1: Q32.
75: Examples supplied by survey respondents.
76: F3.1: Q34.
77: F3.4: Q21, b.
78: F3.4: Q21, e.
79: F3.4: Q21, a.
80: For example, Haley RW – see footnote 14 on page 24.
81: F2: Q8b; F3.2: Q7.
82: F3.2: Q4.
83: F3.2: Q21, Q22 & Q23.
84: F3.2: Q19a.
85: F3.2: Q19b & Q19d.
86: F3.2: Q19e.
87: F3.1: Q15a.
88: F3.1: Q16.
89: Information obtained from www.qualityhealth.org.nz.
90: SNZ HB 8142:2001 Infection Control Audit Workbook – known as the audit tool.
91: F2: Q26.
92: F3.4, Q19a.
93: F2: Q28 – from respondents’ notes to this question about the audit tool’s effect on resources.
page top