Part 1: Background
- What Is Infection Control?
- Rationale for Our Audit
- Risks of Hospital-acquired Infection
- Extent of Hospital-acquired Infection
- Costs of Dealing with Hospital-acquired Infection
- How Can Infection Control Help?
- The Infection Control Standard
- How We Carried Out Our Audit
What Is Infection Control?
1.1
Infection control refers to a range of practices and procedures designed to minimise the risk of spreading infections, especially in hospitals and health care facilities.
1.2
A hospital-acquired infection is an infection that:
- a patient acquires while in hospital (though it may only become apparent after discharge); and
- was neither present nor incubating at the time of the patient’s admission to hospital.
Rationale for Our Audit
1.3
The purpose of our audit was to describe and assess systems for managing hospital-acquired infection in public hospitals. We undertook the audit for four main reasons:
- hospital-acquired infections pose a serious risk to the safety of patients and hospital staff;
- the cost of dealing with hospital-acquired infection is high;
- a significant proportion of hospital-acquired infections can be avoided through effective infection control practices; and
- a review of the management of hospital-acquired infection is timely.
1.4
By October 2004, providers of health care services10– including public hospitals – will have to demonstrate that they meet the Infection Control Standard (see paragraph 1.28 on page 30) in order to be certified under the Health and Disability Services (Safety) Act 2001. We assessed the current position and what work is needed to ensure that hospitals can comply with the Standard by 2004.
1.5
DHBs (see map of DHB boundaries at Figure 1 on page 33) are relatively new bodies, and are continuing to come to terms with their responsibilities. Ensuring the safety of hospital services is a key DHB responsibility, and we saw value in bringing the importance of effective infection control practices to the attention of Board members.
Risks of Hospital-acquired Infection
Hospital-acquired infections pose a serious risk to the safety of patients.
1.6
Hospital-acquired infections are recognised both nationally and internationally as a serious problem. In common with other parts of the world, they are an important concern in New Zealand public hospitals.11 The Ministry’s document An Integrated Approach to Infectious Disease: Priorities for Action 2002-200612 identified hospital-acquired infections (and in particular those caused by organisms that are resistant to commonly used antibiotics) as one of the six highest priority categories of infectious disease.13
1.7
Hospital-acquired infections occur most often in the patient’s urinary tract, lungs, surgical wounds, and bloodstream:
- Urinary tract infections are the most common but least likely to cause significant additional problems or a prolonged stay in hospital.
- Pneumonia, wound infections, and bloodstream infections can have serious consequences, resulting in prolonged hospital stays, ongoing complications and (occasionally) death. Antibiotics used to treat such infections may themselves cause complications or have toxic side effects.
1.8
Where a patient with a hospital-acquired infection dies, it is often from a cause other than infection. Nevertheless, hospital-acquired infections can result in permanent disability or death. In the United States, estimates suggest that hospital-acquired infection is primarily implicated in 1% of all deaths – making it the 11th most common cause of death, and a contributory factor in many more.14 Equivalent data is not available for New Zealand.
1.9
Unless contained, infections can spread throughout a hospital and into the community – as occurred in 2001 when the organism Methicillin-resistant Staphylococcus aureus (MRSA)15 spread from public hospitals to aged care facilities in the North Island. Publicity about outbreaks of hospital-acquired infection reduces the public’s confidence in the safety of our hospitals.
Hospital staff are also vulnerable.
1.10
Hospital staff and people visiting the hospital can also acquire an infection in the hospital, particularly if they are directly exposed to an organism and are susceptible to the disease.
1.11
Hospitals need to manage the risk to staff in order to meet their responsibilities as good employers. Moreover, even if only a small number of staff become sick with a hospital-acquired infection, their absence from work can have major financial and operational consequences for the hospital.
Certain types of patients are more likely to acquire an infection while in hospital.
1.12
Three patient groups are most likely to acquire an infection while in hospital:
- elderly people – whose immune systems deteriorate with age;
- the very young – who have immature immune systems; and
- patients undergoing therapies that suppress their immune systems, e.g. chemotherapy.
1.13
Patients are also more likely to acquire an infection if they:
- have a prolonged stay in hospital;
- had a severe underlying condition before admission that makes them particularly susceptible to infection;
- are attached to medical devices (such as ventilators); or
- have undergone invasive procedures – such as surgery or insertion of tubes into the blood circulation system, bladder or lungs.
The bigger the hospital, the greater the risks associated with hospital-acquired infection.
1.14
Bigger hospitals tend to treat very sick patients who have lower immunity to infections – for example, cancer patients and patients with kidney disease. These hospitals carry out complex procedures that put patients at greater risk of acquiring an infection in hospital.
1.15
At the same time, there is a rationale for having big hospitals – for example, to bring together specialist expertise and sophisticated equipment that often requires expert operators. The job of infection control is to manage the risk of hospital-acquired infection in an environment where very sick patients are receiving complex and invasive treatments.
Outbreaks of hospital-acquired infection are often associated with antibiotic-resistant organisms.
1.16
Most hospital-acquired infections are treated with antibiotics. Widespread prescribing of antibiotics can give rise to organisms that are resistant to one or more types of antibiotic. Antibiotic resistance reduces the options available to treat infections, thereby further increasing the importance of preventing infection in the first place.
Extent of Hospital-acquired Infection
An infection can be passed on in many different ways.
1.17
Organisms capable of causing infection are present everywhere on or in people and animals, and in the environment. A large number of infections are caused by organisms normally present on or in the patient’s own body.
1.18
An infection occurs when organisms capable of causing diseases have the means to invade a susceptible host. Sources of these organisms in hospitals include:
- infected patients and staff;
- people who are carrying organisms but are not infected themselves;
- moist, unclean areas in the hospital environment;
- dry objects and surfaces if they have been recently contaminated by being in contact with a colonised or infected person;
- endoscopes or other medical devices (if not properly processed for re-use); and
- the environment in or near the hospital – e.g. infections caused by exposure to fungal spores from materials around building sites.
1.19
Almost any type of organism can cause infection, but bacteria are the most common cause in hospitals. In hospitals, patients and health care workers are in close contact, making it easier for infections to spread.
Estimates suggest that about one in 10 hospital patients admitted to hospital will acquire an infection while in hospital.
1.20
Overseas studies16, and a New Zealand study17 drawing on multi-year data from one DHB area, suggest that about 10% of patients admitted to hospital will acquire an infection as a result of their hospital stay. Some hospital-acquired infections will not be recorded by hospitals when the infection appears after the patient has been discharged. For this reason, the true rate may be higher.
1.21
Incidence data relating to hospital-acquired bloodstream infections in New Zealand public hospitals has been collected since the mid-1990s, and a study published in 1998 found the rate acceptable for a developed country with a comprehensive health service.18 Almost 80% of bloodstream infections occurred in the six DHBs having the largest hospitals and offering the most complex services. The study recommended that a nationally co-ordinated programme be initiated to monitor and compare bloodstream infection rates for comparable medical and surgical services in high-risk hospital units.
Costs of Dealing with Hospital-acquired Infection
The cost of dealing with hospital-acquired infection is high.
1.22
Hospitals bear most of the direct financial costs of dealing with hospital-acquired infection. No authoritative studies have been carried out to establish the full costs of dealing with hospital-acquired infection in New Zealand. However:
- A recent study19 based on data collected from the hospitals in the area of the Auckland District Health Board estimated that it would cost about $137 million a year to treat hospital-acquired infection in medical and surgical patients in the country’s public hospitals. The total true cost is likely to be higher, as this figure does not include the costs of managing infections acquired by patients in maternity, neonatal intensive care, and paediatric services.
- The cost of treating hospital-acquired infection in adult medical and surgical patients in two Auckland DHB hospitals was assessed at almost $19 million a year.
- Even in smaller hospitals, the costs of treating hospital-acquired infection – or containing a threatened outbreak – can be high. One hospital estimated that it spends $261,000 annually on dealing with surgical site infections.
- In another hospital, the estimated cost of swabs, protective clothing, and medication associated with treating and containing MRSA approached $30,000. Controlling an outbreak of the infection was likely to add around $50,000 to this cost.
| "… There are countless studies from overseas that we regularly reference showing the high cost of infection control inactivity and of the cost-benefits of controlling outbreaks …" |
1.23
Treating hospital-acquired infection consumes scarce hospital resources by prolonging hospital stays, requiring additional investigations and treatment, and taking up extra staff time. Costs to the patient include time off work, rehabilitation and medical costs.
Hospital-acquired infections create extra costs in the community.
1.24
Many hospital-acquired infections become evident after a patient is discharged. Most such infections are not serious, but they nevertheless create extra costs in the community. These costs include:
- the need for family or friends to care for the patient;
- community-based nursing services;
- GP visits; and
- time off work.
1.25
As a further indicator of the amount and cost of infection acquired in our hospitals, we asked the medical misadventure unit of the Accident Compensation Corporation (ACC) for information on the claims it accepted that relate to hospital-acquired infection.
1.26
ACC reviewed claims for the 10 years to February 2002 and found that 4.4% (or 697) of accepted claims for medical misadventure involved a hospital-acquired infection. Wound infections accounted for more than half of those claims, while the most severe form of hospital-acquired infection – bloodstream infection – accounted for 7% of the 697 claims. The costs of the accepted claims over the 10 years ranged from $40 for a medical consultation to $57,000 compensation over a year. Eleven of 342 claims from families for compensation for the death of a family member related to hospital-acquired infection.
How Can Infection Control Help?
A fair proportion of hospital-acquired infections can be avoided through effective infection control practices.
1.27
Infection control is essential to the safety of the hospital environment and to public health. Studies suggest that up to around 30% of hospital-acquired infections could be avoided by use of rigorous infection control practices. One study20 conducted in the United States during the 1970s estimated that an intensive infection surveillance and control programme was associated with a reduction in hospital-acquired infection. Even though this study is now about 30 years old, its findings are still likely to be credible and relevant in today’s environment.
The Infection Control Standard
The Infection Control Standard is designed to promote safe, high-quality delivery of health and disability services.
1.28
The Health and Disability Services (Safety) Act 2001 requires all licensed public (and private) hospitals to comply with the Health and Disability Sector Standards21 by 2004. The New Zealand Infection Control Standard22 (the Standard) was published in 2000. It was prepared by an expert technical committee drawn from the health and disability sector, in preparation for implementation of the standards-based certification regime required by the Act (see paragraphs 2.15-2.20 on pages 42-44).
1.29
The Standard addresses the basic principles and systems of effective infection control. We used the Standard in drawing up our expectations of good practice and in designing a survey questionnaire for our audit. The Standard provides guidance in seven areas:
- governance – with emphasis on a managed environment to reduce the risk of infection to patients, residents of health care facilities, staff, and visitors;
- the composition, responsibilities, and resourcing of the infection control team;
- policies and procedures to prevent and control hospital-acquired infection;
- education for hospital staff and patients;
- surveillance in accordance with agreed objectives, priorities, and methods specified in the infection control programme23;
- policies and procedures to promote the prudent prescribing of antibiotics and other anti-microbial agents; and
- an infection control programme explicitly linked to the organisation’s quality and risk management programme.
How We Carried Out Our Audit
1.30
In February 2000, the National Audit Office (NAO) in the United Kingdom published a report24 on the management and control of hospital-acquired infection. The report highlighted the importance of infection control as a dimension of public health care and hospital safety. It drew conclusions about the quality of strategic management, surveillance, and measures for prevention, detection, and control in England. We identified benefits in taking a similar approach to examining infection control arrangements within the New Zealand public hospital environment.
1.31
We gathered information about infection control arrangements in public hospitals through an extensive survey questionnaire25 that we sent to all 21 DHBs. The questionnaire drew on:
- the issues explored by the NAO in its study of the management of hospital-acquired infection;
- the requirements of the Standard (see paragraph 1.29), research, and international best practice;
- the advice of two practitioners (see paragraph 1.37) and the Ministry; and
- the views of managers and practitioners when we piloted the questionnaire in two hospitals.
1.32
All 21 DHBs completed the questionnaire and returned it by April 2002, in good time for us to undertake our analysis. Many DHBs’ responses included valuable additional comments, and, in some cases, relevant supporting documents, to illustrate their infection control arrangements or practices.
1.33
When we had undertaken a preliminary analysis of the survey responses, we visited four DHBs with tertiary hospitals – Auckland, Capital and Coast (Wellington), Canterbury, and Otago – to gather further information about their infection control practices. We also examined all DHBs’ planning documents, their six-month reports to June 2001, and their annual reports to June 2002.
1.34
We consulted the Ministry in planning this audit, seeking its views on the design and content of our questionnaire. In the course of the audit, we gathered further information on the role of Ministry staff in drawing up policy and standards for infection control, and on their use of the information they received from DHBs on hospital-acquired bloodstream infections.
1.35
We consulted two other public entities on their responsibilities relating to infection control and hospital-acquired infections:
- the Institute of Environmental Science and Research Limited (ESR), a Crown Research Institute specialising in environmental and public health, and forensic science; and
- the Accident Compensation Corporation.
1.36
We also invited the views of professional bodies and groups with an interest in infection control matters.26
1.37
Our audit team included an infection control practitioner27 from a DHB who worked full-time on the audit. Two medical practitioners attended meetings of our internal steering committee for the audit, and provided advice and comments on our plans and the draft report:
- Dr Timothy Blackmore, Infectious Diseases Specialist, Capital and Coast DHB, and
- Dr David Holland, Microbiologist and Infectious Diseases Specialist, Auckland Hospital.
1.38
We also consulted a medical microbiologist and hospital epidemiologist on the scope of our audit.
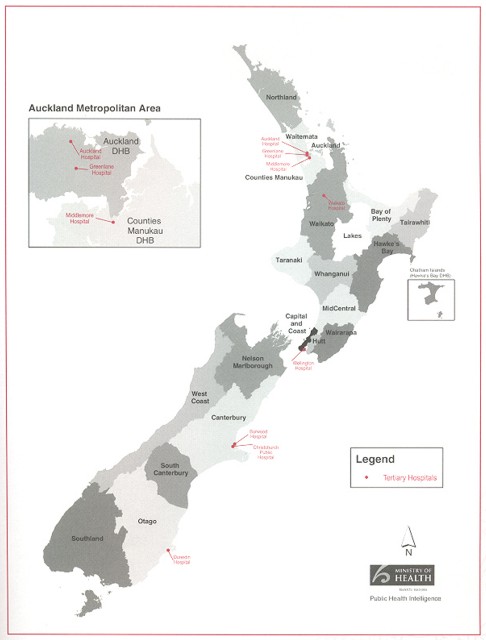
Figure 1
District Health Board Boundaries and Tertiary Hospitals
10: The term health care services means services that are hospital care, residential disability care, rest home care, or specified health or disability services.
11: As shown, for example, by the further analysis of material collected for the study conducted by Davis et al: Adverse Events in New Zealand Public Hospitals: Principal Findings from a National Survey; Occasional Paper No 3, published by the Ministry of Health, December 2001; ISBN 0-478-26265-5 (Booklet), 0-478-26268-X (Internet); available on www.moh.govt.nz.
12: Ministry of Health, November 2001, ISBN 0-478-26230-2 (Book), 0-478-26231-0 (Internet); available on www.moh.govt.nz.
13: The other five highest priority infectious diseases are: vaccine-preventable diseases, infectious respiratory diseases, blood-borne infections, sexually transmitted infections, and food-borne enteric (intestinal) diseases.
14: Haley RW: Managing Hospital Infection Control for Cost-effectiveness: A strategy for reducing infectious complications; American Hospital Publishing, Chicago, USA; 1986.
15: MRSA is resistant to methicillin, oxacillin, and other antibiotics. It can spread easily in hospitals and other health care settings. We describe the nature and impact of MRSA in more detail in Figure 15 on page 154.
16: Pittet D: Nosocomial bloodstream infections; chapter in Prevention and control of nosocomial infections edited by Wenzel R.P; published by Williams & Wilkins, Philadelphia. 1993 (2nd edition); ISBN 0-683-08921-8. Plowman R, Graves N, et al: The Socio-economic Burden of Hospital Acquired Infection; published by the Public Health Laboratory Service, London, 1999.
17: Graves N, et al: The Prevalence and Estimates of the Cumulative Incidence of Hospital-Acquired Infections Among Patients Admitted to Auckland District Health Board Hospitals in New Zealand; published in Infection Control and Hospital Epidemiology (an official journal of the Society for Healthcare Epidemiology of America), Vol. 24, No. 1, January 2003.
18: Jones M, et al: Hospital-acquired bloodstream infections in New Zealand; published in the New Zealand Medical Journal, February 1998.
19: Graves N, Nicolls T, Morris A: Modeling the Costs of Hospital-acquired Infections in New Zealand; published in Infection Control and Hospital Epidemiology (an official journal of the Society for Healthcare Epidemiology of America), Vol. 24, No. 3, March 2003.
20: Haley R, Culver D, White J, et al: The efficacy of infection surveillance and control programmes in preventing nosocomial infections in US hospitals; published in American Journal of Epidemiology Vol. 121, 1985.
21: A series of generic standards that are applicable to a wide range of specialities, age groups, and health and disability settings.
22: Standards New Zealand: NZS 8142:2000 Infection Control.
23: Ibid. Table B1 – surveillance guide.
24: Report by the Comptroller and Auditor General: The Management and Control of Hospital Acquired Infection in Acute NHS Trusts in England; The Stationery Office, London; 17 February 2000; available on www.nao.gov.uk.
25: The blank survey form is [was] available on www.oag.govt.nz under “Publications”.
26: The New Zealand Nurses Organisation (NZNO), the NZNO Division of Infection Control Nurses, the New Zealand Medical Council, and the Royal Australasian College of Surgeons.
27: An infection control practitioner is usually a registered nurse with appropriate training and skills in infection control.
page top