Part 3: Managing buildings and clinical equipment to maintain health services
3.1
In this Part, we set out the results of our analysis of the specific information about building and clinical equipment asset management we collected as part of our 2013/14 audits of DHBs. For each of these two classes of assets as a whole, we discuss:
- their age and condition;
- their levels of service for, and the performance;
- the management information systems used; and
- performance information reporting.
3.2
We also present the results of the self-assessments that all DHBs carried out at the request of the Ministry and the Treasury in 2014 and of Architecture, Engineering, Construction, Operations, and Management's (AECOM's) review of nine of these self-assessments.
3.3
The results of our work on asset management practices showed that:
- Levels of service for assets tend not to be well defined, which means that reporting of asset performance is generally weak.
- Many DHBs have asset management information systems with advanced functionality but often do not use this functionality.
- DHBs generally do not systematically collect, maintain, analyse, and use asset information – such as about age, condition, and performance, particularly for clinical equipment.
- More than half of the DHBs do not regularly reconcile their asset management and financial information.
- There is limited reporting to governors and senior managers about asset performance and condition.
- Based on AECOM's review, up to two-thirds of DHBs might not have substantively updated their asset management plans since 2009, when asset management requirements were introduced.
3.4
This raises questions about how well DHBs are positioned to support future service delivery and financial decision-making.
3.5
Our results are reinforced by the DHBs' self-assessments. These self-assessments suggest that DHBs could improve many aspects of their asset management with moderate effort. The weakest aspects of current practice, and the aspects with the largest gaps between current practice and target maturity, are those assessing how well asset management is integrated and embedded into the DHB's overall processes and practices.
What do we know about the condition and remaining useful lives of existing buildings and clinical equipment?
3.6
Effective asset management means knowing the condition of assets, their likely remaining useful lives, and the potential for critical assets to fail. Knowing and planning for asset management needs can make a significant difference to the financial operations and likely future costs of a DHB.
3.7
Most DHBs gather information about the condition of their assets, especially critical assets. However, there are wide variations in how formally and regularly they assess and report this information. Only 12 DHBs have formal approaches to recording asset condition in an asset management information system (AMIS).
3.8
Asset revaluations are important for asset management because they necessarily include reassessing the best estimate of an asset's remaining useful life. Regularly reassessing the remaining useful lives of assets helps to forecast and plan asset replacements and renewals. Assessments of the remaining useful life of an asset can change over time, and assets can be impaired (such as those of the Canterbury DHB because of the Canterbury earthquakes) or become obsolete.
3.9
Even where information is available, DHBs do not always use it well – for example, to update asset management forecasts and expectations. The practice of regularly updating asset management plans did not seem to be well embedded in DHBs. Many asset management plans have not been substantively reviewed since 2009.
3.10
Overall, DHBs appear to have better asset management information for buildings than for clinical equipment. DHBs carry out regular revaluations (at least every five years) to determine the fair value of their building assets. Thirteen DHBs have buildings that are less than halfway through their useful lives.
3.11
Clinical equipment is valued on the basis of historical cost. DHB asset and financial management practitioners told us that the useful lives of many clinical equipment assets would not be reassessed from the initial expected life that was assigned when the assets were acquired, even though actual lives might have exceeded initial expected lives.
3.12
Figure 4 shows that buildings make up most of DHBs' assets.
Figure 4
Health asset classes by value, 2008-2018
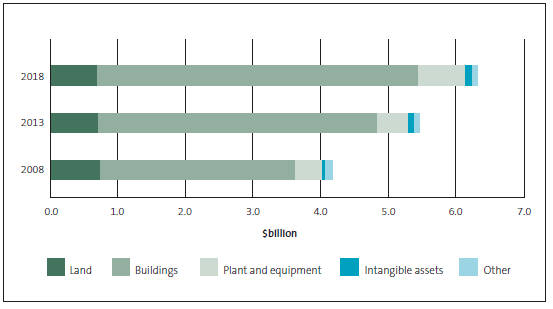
Source: The Treasury, 2014 Investment Statement, page 59. The 2018 values are forecast.
3.13
Our auditors estimated that buildings that are currently valued at $24 million have remained in use past the end of their theoretical useful lives. Figure 4 shows that this represents a small proportion of the total value of DHBs' building assets.
3.14
Clinical equipment is included in plant and equipment. Figure 4 shows that, in 2013, plant and equipment made up less than $500 million of DHBs' total assets. Our auditors estimated that more than $300 million of clinical equipment has remained in use past the end of its theoretical useful life. Figure 5 shows the through-life10 of buildings and clinical equipment by DHBs.
Figure 5
Through-life of buildings and clinical equipment, by district health board
| District Health Board | Through-life of buildings (%) | Through-life of clinical equipment (%) |
|---|---|---|
| Northern Region | ||
| Auckland | 34 | 73 |
| Counties Manukau | 11 | 79 |
| Northland | 38 | 83 |
| Waitemata | 42 | 69 |
| Midland Region | ||
| Bay of Plenty | 41 | 64 |
| Lakes | 35 | 66 |
| Tairāwhiti | 40 | 53 |
| Taranaki | 68 | 76 |
| Waikato | 7 | 66 |
| Central Region | ||
| Capital and Coast | 42 | 68 |
| Hawke's Bay | 66 | 53 |
| Hutt Valley | 41 | 66 |
| MidCentral | 53 | 66 |
| Wairarapa | 24 | 67 |
| Whanganui | 40 | 69 |
| South Island Region | ||
| Canterbury | 69 | 76 |
| Nelson Marlborough | 42 | 68 |
| South Canterbury | 58 | 76 |
| Southern | 64 | 65 |
| West Coast | 84 | 72 |
Note: Through-life of buildings is calculated as 100% less the age profile of depreciated replacement cost divided by replacement cost. The replacement cost may apply to different years as the revaluation process takes place at least every three years. [More complicated than previously.]
3.15
Overall, clinical equipment appears to be a long way through its useful life. No DHB has clinical equipment that is less than halfway through its useful life, and several DHBs have clinical equipment more than 75% through its useful life.
3.16
These results do not mean that DHBs are not investing in clinical equipment on an ongoing basis. Nor does it mean, given the changes outlined in Part 1 about the effect of technology on health assets that existing clinical assets should be replaced on a like for like basis. However, as an asset class, the average age of clinical equipment appears to be increasing. This means that DHBs will need to plan how to keep delivering services for many clinical equipment assets reaching the end of their useful lives in the medium term. It might also mean that DHBs are not regularly reassessing the useful lives of clinical equipment and so might be depreciating clinical equipment assets too quickly.
3.17
In commenting on the draft of the report, some DHBs noted that the lack of up-to-date information about the useful life of their assets did not mean that they lacked a good knowledge of the condition of their assets. They observed that assets will often be suitable and safe for use beyond their initial useful life.
3.18
We agree with this observation. We consider that it reinforces the need to maintain good information about the actual performance and lives of assets. This allows DHBs to make practical and realistic plans for renewing and replacing those assets. It also allows them to plan for and manage the associated funding implications.
3.19
Our concern is that, at present, it is not clear that all DHBs are maintaining this information. DHBs need to improve their information about, and understanding of, these assets to manage the performance, maintenance, and eventual renewal or replacement of the assets.
3.20
Given the nature and range of clinical equipment assets, it might not be as cost-effective or useful to reassess their useful lives as it is for buildings. However, we consider that DHBs should reassess the useful lives of high-value and critical individual assets or of networks of assets.
| Recommendation 1 |
| We recommend that each DHB understand, respond to, and manage demand for its assets and the related risks. |
| Recommendation 2 |
| We recommend that each DHB know how well its mix of assets meets its service delivery needs now, and in the future. |
How is asset performance measured?
3.21
Asset performance relates to the ability of the asset to provide the agreed levels of service or service standards. In other words, is the asset "fit for purpose"?
3.22
Measuring asset performance involves three elements:
- agreeing on and defining the service required from using the asset;
- regularly comparing the actual performance of the asset with the defined service standards; and
- reporting this performance to the people responsible for decision-making.
3.23
DHBs should know what measures and targets about the performance of their critical assets are important to them, then monitor and report that performance regularly. As well as having asset management teams that monitor the performance of assets, DHBs do other kinds of monitoring – for example, clinical departments check that equipment meets clinical standards and have warrants of fitness that they are operating safely.
3.24
DHB asset and financial management practitioners and advisors told us that, although quite specific and demanding specifications are set when assets are purchased or commissioned, this rigour is often not maintained in monitoring the ongoing performance of assets.
3.25
Only half of the DHBs have systems for recording asset performance information about buildings, and 11 have systems for recording information about clinical equipment.
3.26
We looked at whether DHBs measured performance in what we considered would likely be important dimensions for health-related assets. The dimensions we reviewed were:
- capacity or utilisation;
- safety;
- legislative or regulatory compliance;
- risk of asset failure or outages; and
- cost efficiency.
3.27
Figure 6 sets out the five dimensions of asset management that DHBs most commonly measure. It shows that "not applicable" responses have the least variation. This reflects that not all DHBs have systems for recording asset performance. Asset managers of DHBs without systems for measuring and monitoring assets tend to rely on clinical departments to alert them to asset performance concerns or issues.
3.28
On average, the DHBs that use systems to record asset performance measure seven performance dimensions (for both building and clinical assets). The two most commonly measured dimensions are safety and legislative or regulatory compliance.
Figure 6
Asset performance dimensions that district health boards most commonly measure
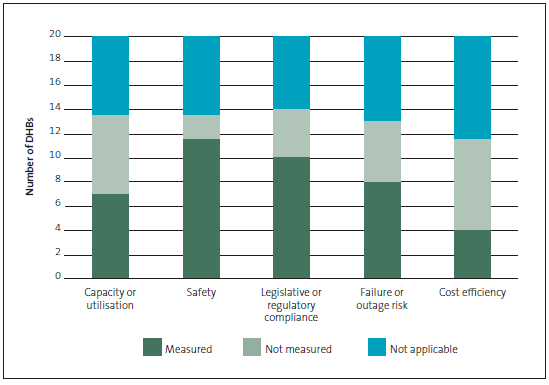
Note: Some sections in Figure 6 are not whole numbers because the numbers are an average of DHBs' performance in respect of buildings and their performance in respect of clinical assets.
3.29
We looked at DHBs' annual reports since 2010 to see what sort of performance measures and targets they include that would give readers an understanding of the services and results related to assets. Although we found limited information of this nature, some DHBs include information about operating theatre use.
3.30
Operating theatres are one of the most service-intensive and expensive assets in a typical major hospital. One DHB estimated that it costs an average of $1,121 each hour to operate a theatre, excluding the cost of surgical personnel.
3.31
In the past, the Ministry required DHBs to report operating theatre use in their annual reports, but it no longer does so. Some DHBs have continued reporting operating theatre use, but others have not. In 2013, 14 DHBs reported operating theatre use.
3.32
We looked at publicly available information, primarily DHB annual reports from 2010 to 2014, to see what they said about the measurement of, monitoring of, and results achieved in operating theatre use.
3.33
Where results were reported, the rates for operating theatre use between 2010 and 2014 look impressive:
- The average operating theatre use was 85% of the time, and the rates ranged from 72% to 99%.
- The rates were usually very close to the "base" or budgeted use and generally increased during the period.
3.34
There are catches. The principal issue is that the rates are for "resourced" use of the theatre (in other words, staff resource is assigned to the theatre). It does not include theatre sessions not allocated because of planned leave or maintenance. There also appeared to be some differences in how DHBs assessed "use".
3.35
One of the important aspects of measuring performance is the trend over time, so we are surprised that the Ministry did not maintain its expectation that DHBs report the measure.
3.36
Figure 7 describes another initiative described in the annual reports we reviewed, the Productive Operating Theatre.
Figure 7
Case study 1: The Productive Operating Theatre
| The Productive Operating Theatre (TPOT) had its genesis in a series of improvement programmes from the National Health Service in the United Kingdom. One New Zealand DHB described it as "one of a series of programmes aimed to improve patient satisfaction and outcomes, staff work satisfaction, and efficiency in theatres. The key result areas include reduction in cost of consumables, stable nursing and support workforce, reduced turnaround times, and improved on-time starting and finishing of theatre sessions." For DHBs that have introduced TPOT programmes, the information reported indicates that there have been significant benefits to the efficient running of operating theatres. The DHB annual reports mentioned some of the initiatives:
However, to sustain improvements, it is necessary to measure theatre use on an ongoing basis and to maintain and extend the TPOT initiatives. We realise that health professionals have many demands on their time. Nevertheless, this seems to us to be an initiative worthy of increased effort. It provides the multiple benefits of using expensive operating theatres better, better and more satisfying work practices, and more operations for patients. |
3.37
Since the Crown Entities Act 2004 was amended in 2013, the Ministry's annual planning guidance has advised DHBs to include information about asset performance (availability, use, functionality, and condition) and management of assets in annual plans.
How is asset management information captured and integrated with financial information?
3.38
For entities with complex networks of assets, a formal AMIS is an important tool for dealing with the amount of information and analysis needed to support those assets.
3.39
Asset managers use an AMIS to help determine whether to maintain, renew, or replace (through new capital investment) assets. An AMIS can help justify the level and funding of asset-related spending.
3.40
The basic features of an AMIS provide essential information about assets. The features include the asset register, financial information, maintenance work recording, condition assessments, a record of which assets are critical, and a record of customer service requests. Advanced functions can include maintenance planning, asset performance, deterioration modelling, life-cycle cost optimisation, work management, risk management, and inventory control.
3.41
Figure 8 shows the Information Systems Maturity Index, which describes the range of AMIS functionality from minimum to advanced.
Figure 8
Information Systems Maturity Index
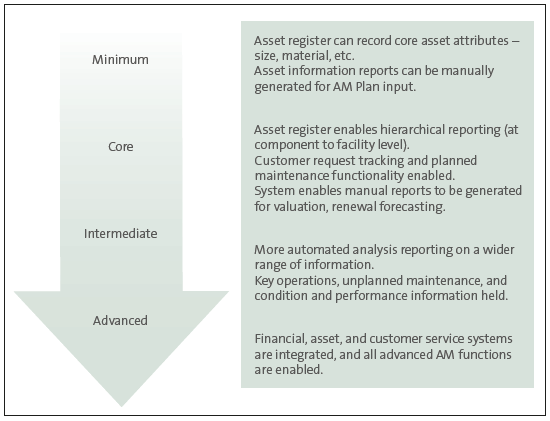
Source: NAMS (2011), International Infrastructure Management Manual, page 4/28.
3.42
Nearly two-thirds of DHBs use an external proprietary AMIS with extensive functionality for their clinical equipment and buildings assets. Only two DHBs do not use a formal AMIS.
3.43
Most DHBs use the core functions of their AMIS (most commonly, the asset register, basic financial information, and maintenance work recording), but a third did not use all the available functionality. For instance, recording performance information is a function available in most of the various proprietary AMIS that DHBs use. However, only about half of the DHBs use a formal system to record asset performance.
3.44
The ability to easily integrate and reconcile the AMIS with the DHB's financial management information system (FMIS) is also important for managing DHB assets and for planning and managing capital expenditure. Easily integrating and reconciling asset and financial information can help DHBs to optimise their decisions about the best mix and timing of asset maintenance, renewal, and replacement options based on the benefits, costs, and the DHB's needs and risks.
3.45
Most DHBs have separate information systems for managing their assets and for managing their finances. Nine perform regular reconciliations of their AMIS and FMIS. Others do not reconcile their AMIS and FMIS, using their FMIS for asset information even though their AMIS has more sophisticated functionality.
Who gets information about the condition and performance of assets?
3.46
Almost three-quarters of DHBs report asset condition on some basis, generally "by exception as issues arise" to the asset manager. By comparison, reporting asset performance is patchy. Only five DHBs (which use formal systems for performance) record and report building and clinical asset performance regularly. Information on asset performance monitoring is often generated by the asset/facilities team or a third-party contractor responding to the service requests of the day-to-day clinical users of equipment and facilities.
3.47
The Board of a DHB or a subcommittee tends to receive reporting of only high-level asset management matters or on a "by exception" basis about major issues (such as asset failures).
3.48
The extent of reporting based on "response to service request" and "by exception as issues arise" suggests that DHBs could take a more managed and integrated approach to asset performance, use, condition, and future-needs forecasting.
3.49
DHB asset management practitioners told us that the limited visibility of asset performance and condition can sometimes mean that senior levels of DHB governance and management might not appreciate how important asset management is to efficient service delivery.
3.50
Many different professional staff and services need to be co-ordinated to make effective use of both staff and assets. One asset manager told us that dealing with asset information about clinical equipment in particular is difficult because there tends to be no clear point of accountability and responsibility for that information.
3.51
DHBs should work to integrate assets with other information (such as financial or service performance information), and asset, financial, and clinical managers should share information for longer-term forecasting and service planning, as well as for day-to-day service delivery.
| Recommendation 3 |
| We recommend that each DHB has reliable information about its assets and their condition that supports its planning for-long term service delivery. |
How do district health boards assess their own current asset management practice?
3.52
The Treasury and the Ministry have been working to improve the asset management practice maturity of DHBs. In 2014, all DHBs assessed their "current practices" and "appropriate practice" targets against 17 aspects of asset management maturity.11 The Ministry selected nine DHBs' self-assessments for expert review by AECOM.12
3.53
The current practice state of each aspect and the target maturity state was assessed and scored out of 100. The scores were put in bands as follows:
- aware: 0-20;
- minimum: 25-40;
- core: 45-60;
- intermediate: 65-80; and
- advanced: 85-100.
3.54
There were variations between self-assessments and the expert-reviewed assessments prepared by AECOM. For instance, the average gap between the current practice and target maturity for all DHBs for all aspects was 29.5, or a two-band gap between practice and target maturity. However, the gaps between practice and target maturity were greater for DHBs reviewed by AECOM than for those that assessed themselves.
3.55
Figure 9 shows the strongest and weakest aspects of current asset management practice and the aspects with the smallest and largest gaps between current practice and the target maturity state.
Figure 9
District health board self-assessments of asset management maturity for current practices and the target maturity state
| Current practice score | Current practice to target maturity | ||
|---|---|---|---|
| Strongest aspects (> 60: Intermediate) | Weakest aspects (< 50: Core) | Smallest gap (< 20) | Largest gap (> 30) |
| Service delivery models | Financial and funding strategies | Decision-making | Improvement planning |
| Asset register data | Asset management policy and strategy | Asset management plans | Levels of service and performance management |
| Decision-making | Quality management | Demand forecasting | Asset management policy and strategy |
| Demand forecasting | Asset management plans | Capital investment strategies | Asset management teams |
| Asset management teams | Operational planning and reporting | ||
| Improvement planning | Information systems | ||
3.56
The Ministry and the Treasury identified several common issues, challenges, and trends from AECOM's report. These include:
- Although staff were committed and well intentioned, there was a general lack of knowledge about comprehensive asset management principles.
- AECOM was not convinced that there was a good level of understanding of the longer-term expenditure profile or planning to accommodate the increased expenditure needs as assets deteriorate.
- Although future population and demographic changes and forecast health service needs were generally understood, optimising the location of service provision was less well understood and the implications for facilities and equipment tended to be short term and reactive.
- DHBs used a large variety of IT systems, but there was little integration between systems and manual reconciliation of asset information.
- Maintenance planning for facilities was generally reactive.
3.57
AECOM also reported that all DHBs expressed a desire for the Ministry to play a greater role in facilitating asset management and best practice information-sharing, providing guidelines and tools, and setting clear directional expectations.
3.58
The assessments identify many similar areas to those we have expressed concern about in this report. DHB self-assessments suggest that they could improve many aspects with moderate effort. However, three aspects appear on both the list of weakest aspects and of largest gaps. These aspects relate to how well asset management is integrated and embedded into the processes and practices of DHB management. We set out how AECOM describes intermediate and advanced practice for these aspects in Figure 10.
Figure 10
Characteristics of intermediate and advanced asset management for the aspects of weakest current practice and largest gap to target maturity for district health boards
| Intermediate | Advanced | |
|---|---|---|
| Asset management policy and strategy | Expectations of each business activity are supported by action plans, resources, responsibilities, and time frames. Asset management policy and strategy is reviewed and adopted by the Executive Team each year. | Asset management policy and strategy is fully integrated into the organisation's business processes and subject to defined audit, review, and updating procedures. |
| Asset management teams | All staff in the organisation understand their role in relation to asset management, it is defined in their job descriptions, and they receive training aligned to their roles. A person on the Executive Team has responsibility for delivering the asset management policy and strategy. | There is strong leadership of the asset management functions throughout the organisation. There is a formal asset management capability management programme. The cost-effectiveness of the asset management structure has been formally reviewed. |
| Improvement planning | There is formal monitoring and reporting on the improvement programme to the Executive Team. Project briefs have been developed for all key improvement actions. Resources have been allocated to the improvement actions. | There is evidence that agreed improvement plans have delivered the expected business benefits. |
3.59
Decision-making appears in Figure 9 on both the strongest aspect and the smallest gap list. AECOM describes the maturity bands as:
- Intermediate: Formal decision-making and prioritisation techniques are applied to all operational and capital asset programmes within each main budget category/business unit. Formal decision-making techniques are applied to major projects and programmes. Critical assumptions and estimates are tested for sensitivity to results.
- Advanced: As for Intermediate, plus the decision-making framework enables projects and programmes to be optimised throughout the business. Formal risk-based sensitivity analysis is carried out.
3.60
Good asset management practice emphasises that best results are achieved when all the aspects are collectively operating at a strong enough level for the nature of the assets involved and the service delivery challenges facing the organisation. This raises questions about how effective the contribution of good decision-making about assets can be if asset management is not well integrated and embedded into the processes of each DHB.
3.61
Figure 11 describes the practices of Auckland DHB that resulted in it achieving good overall results in AECOM's review of asset management maturity assessments.
Figure 11
Case study 2: Auckland District Health Board's asset management practices
| This case study discusses Auckland DHB's asset management practices and provides some reflections about how it has strengthened its asset management in recent years. Auckland DHB says that the support for, and expectations from, the Ministry for capital expenditure information were a useful prompt to improve its asset management. In response, Auckland DHB decided to develop its internal asset management capability. It brought the preparation of the DHB asset management plan and capital expenditure forecasting in-house (rather than relying on external providers). A formal asset management working group made up of members from the Facilities, Clinical Equipment, Information, and Finance functions was involved in Auckland DHB's asset management maturity self-assessments. Co-ordinated capital and asset management planning was put in place to ensure a whole-of-DHB perspective for all asset classes (buildings, clinical equipment, IT/IM, and other assets) and between service groups, to look after existing assets and their replacement, as well as planning for new assets to meet growth. Affordability of capital in terms of both operational cost impact and financing requirements, is assessed centrally within the DHB to ensure that financial sustainability is not compromised. Auckland DHB attributes its strong asset management to good capability within the Facilities team, engagement of the Facilities team with key staff within services, and a management structure that reinforces integration and engagement. This management structure is based on single-point accountability at service-group level. Clinical leaders are appointed as directors responsible for each directorate, supported by general managers, finance personnel, and human resources personnel. Directors are responsible for managing assets within their portfolios, planning for their replacement, and identifying any capacity increases required. A Capital Asset Management and Planning Committee, made up of all the directorate leaders, takes responsibility for investment decision-making, prioritising capital expenditure, and monitoring asset management improvement initiatives throughout the DHB. Particular aspects of Auckland DHB's asset management planning that AECOM assessed as strengths in its expert review are described below. Demand forecasting: Demand drivers are identified, analysed, and documented. Health services needs are assessed and effects on assets and facilities are identified and projected through models, including a bed model based on the Ministry's demand model, a theatre model based on a contracted analysis, and space modelling. Further modelling work is required to inform factors such as service demand, capacity, and models of care changes to inform facility and capital requirements. Auckland DHB has recently begun developing a Clinical Services Plan to better inform its future capacity requirements and the scope and timing of capital investments. Decision-making: Auckland DHB developed a comprehensive Investment Manual jointly with Waitemata DHB to provide a (national and regional) system view of capital planning and funding for the DHB sector as well as detailed district capital processes and business case development guidelines. The manual defines thresholds for analytical rigour and approval, and an options analysis framework. The Capital Asset Management and Planning Committee prioritises major projects by using a risk framework tied to service outcomes. Although the prioritisation process tends to be short term and driven by financial affordability, improvement to medium- to long-term plans is intended. Maintenance planning: Detailed maintenance and equipment certification programmes are in place, as are disaster response/recovery plans for facilities. Operating and maintenance plans have been prepared for all systems and are routinely required as part of the technical information on completed capital works. A vehicle maintenance contract is in place. Forensic root cause analysis is carried out on all significant plant failures and renewals planning factors in maintenance activity and costs, although the optimal blend of reactive versus planned or prescriptive versus performance maintenance is not specifically assessed. Capital investment strategies: Capital projects are identified and prioritised using a prioritisation tool. The Capital Investment Manual describes approval thresholds and the degree of justification required. Limitations include the lack of a clinical services plan and a level-of-service framework to systematically identify what the project needs to deliver. The Asset Management Plan is used for forecasting capital expenditure, limited by available cash. Capital expenditure bids and intentions are submitted by all services and informed by various sources. Information systems: A mix of systems is used, although these have limited inter-connectivity. Auckland DHB uses a proprietary AMIS for building and plant assets and for about 18,500 items of clinical equipment. Information is not held centrally for a large number of assets, where maintenance is provided by contractors (for example, radiology and laboratories). Service delivery models: Auckland DHB has found in the past that a fully contracted-out service delivery model to one maintenance service provider does not provide good value for money. It uses a blend of internal and external maintenance contracts. The Facilities team carries out routine clinical equipment servicing and facility repairs and maintenance. Larger or more specialised works are contracted out, generally using open market procurement. Standard contracts and formal tendering process are in accordance with central government guidance. |
Getting traction on asset management improvement initiatives
3.62
Although there has been an emphasis on improving asset management since 2009 and practice within individual DHBs has been strengthened, our audit work suggests that initiatives during the last decade have improved DHBs' overall asset management to only a limited extent.
3.63
In our audit work on DHBs' management of buildings and clinical equipment, we found that many DHBs had last updated their asset management plans in 2009.
3.64
Participants in our workshop considered that initiatives now under way might help achieve change. One such initiative is the Health Asset Management Improvement Group, which was formed in 2015 to support DHBs in improving their asset management maturity.
3.65
Some participants also pointed to the Ministry's Health Strategy Update work and new requirements set out in Cabinet Office Circular CO 15/5 Investment Management and Asset Performance in the State Services as increasing focus on asset management.
3.66
The participants noted that initiatives to improve asset management will need to:
- develop consistent health-asset metadata for all DHBs and others involved in DHBs' asset management planning and decision-making to use;
- build more robust cases for funding changes based on good information;
- use information to co-ordinate and communicate the overall plan, picture, and consequences;
- look at spatial planning needs to understand and manage future demand and the resulting asset needs; and
- clarify national and regional planning intentions and funding envelopes to allow district responses to develop.
3.67
In 2015, the Ministry updated its Operational Policy Framework to incorporate the Treasury's capital assessment guidance and the Cabinet's Capital Asset Management policy. Under these changes, DHBs are now required to do formal asset management planning. This means that they must prepare an asset management plan that shows planned asset replacement and the expected financing arrangements, including the use of cash generated from operations. Asset management plans must address:
- strategic asset management;
- strategic asset financing;
- facilities and major equipment; and
- Information Services Strategic Plan.13
3.68
Asset management plans must be maintained as a "live document" and kept up to date. Components of the asset management plan will be required as part of Annual Plans, Regional Service Plans, and business case development. There are currently no expectations to provide the asset management plans to the Ministry.
3.69
We consider that these requirements are an important opportunity for DHBs to improve their asset management information and planning. We expect each DHB, the Ministry, the Capital Investment Committee, and regional capital committees to use them to improve DHBs' asset management.
| Recommendation 4 |
| We recommend that the Ministry of Health and the Treasury provide support to help DHBs to improve their asset management practices, including making more effort to identify, share, and implement the lessons from the leaders of DHB asset management. |
10: The through-life is the proportion of the expected total useful life of an asset that has already been consumed.
11: The 17 aspects of asset management maturity the self-assessments covered were asset management policy and strategy, levels of service and performance management, demand forecasting, asset register data, asset condition assessment, risk management, decision-making, operational planning and reporting, maintenance planning, capital investment strategies, financial and funding strategies, asset management teams, asset management plans, information systems, service delivery models, quality management, and improvement planning.
12: AECOM selected Northland, Auckland, Counties Manukau, Waikato, Wairarapa, Capital and Coast, Nelson Marlborough, West Coast, and Southern DHBs for review.
13: See Cabinet Office Circular CO 15(5), Investment Management and Asset Performance in the State Services, http://www.dpmc.govt.nz/cabinet/circulars/co15/5, and the Treasury's information about investment management (and asset management) at http://www.treasury.govt.nz/statesector/investmentmanagement.