Part 2: Audit results for 2012/13
2.1
In this Part, we discuss the 2012/13 audit results and our areas of interest, including:
- our audit reports;
- observations and matters arising from the 2012/13 audits; and
- our assessment of the management environment, systems, and controls for DHBs and other significant health sector entities.
2.2
We discuss DHBs' service performance reporting, including our qualified audit opinions on performance information, in Part 3. We discuss DHBs' financial results and performance in Part 4.
Overview of our audit reports
2.3
There are legislative requirements for government departments, Crown entities (including DHBs), and other public entities to report on their service performance, and for the Auditor-General to audit that reporting. Our audit reports include our opinion on the entity's financial statements and on its performance information.
2.4
We set out details about our standard and non-standard audit reports, and timeliness of reporting, in our report, Central Government: Results of the 2012/13 audits, Volume 2. In this Part, we provide an overview of audit reports for major health sector entities. Non-standard audit reports include:
- modified audit opinions7 on the financial statements or performance information; or
- unmodified opinions that include a paragraph emphasising a matter (an emphasis-of-matter paragraph) or otherwise drawing the reader's attention to a particular matter (an other-matter paragraph).
2.5
We summarise our audit reports for significant public entities in the health sector in Figure 3, including a brief explanation of why we issued the non-standard audit reports.
Figure 3
Summary of 2012/13 audit reports
| 2012/13 audit reports | Public entities in the health sector |
|---|---|
| Standard audit reports | We issued standard audit reports for:
|
| Non-standard audit reports These include modified and unmodified audit opinions. |
Modified opinions We issued modified audit opinions for all 20 DHBs, which included:
We also qualified our opinion on particular performance information reported by Lakes DHB and by Wairarapa DHB. We issued an unqualified opinion on the Ministry of Health's financial statements and a qualified opinion on its service performance information. We explain our qualified opinion about service performance information in Part 3. We qualified our opinion on the Auckland District Health Board Charitable Trust's financial statements because the Trust had limited control over donations and we could not confirm that all donations were properly recorded. Unmodified opinions with an "emphasis of matter" paragraph We drew attention to the uncertainty about the delivery of office functions in the future of the 16 health regulatory authorities and the two secretariats. We drew attention to the uncertainty about Allied Laundry Services Limited's ability to continue as a going concern because of the national restructuring of laundry services being led by Health Benefits Limited. We drew attention to the appropriate preparation of Manukau Health Trust's financial statements on a disestablishment basis. The Trust is expected to be wound up before the next balance date. |
Observations and matters arising from the 2012/13 audits
2.6
A significant matter arising from our 2012/13 audit work was the qualified opinions relating to service performance reporting by DHBs. This is a sector-wide issue that affected the audits of all DHBs and the Ministry. We discuss it further in Part 3.
2.7
DHBs continued to operate in a constrained financial environment, with lower increases in funding and a focus on making efficiencies and cost savings. This included the continued focus on developing and implementing regional and shared services initiatives for the DHB sector, including those led by HBL. We considered these and other important matters, such as procurement and DHBs' asset management, in our audit work.
Information systems and controls
2.8
As part of the annual audit, we consider information systems and technology (IT) controls that affect the reliability of the financial statements and service performance reporting. The work includes assessing general information technology controls, business application controls, and data analysis. Matters that auditors focus on include:
- assessing risks related to an entity's activities, such as its IT governance and strategic planning, IT processes and organisation, and how performance is monitored and evaluated; and
- testing operational effectiveness of management controls, such as data and operations management, problem and incident management, systems acquisition and project management, and security (network and applications).
2.9
Balancing IT business requirements with the availability of resources is a continuing challenge for DHBs. We are interested in DHBs' information service risks, particularly the ongoing regionalisation of IT operations, information security, business continuity, emerging technologies, and effective IT governance.
Effects of regionalisation on the IT environment
2.10
Regionalisation, collaboration, and shared services continued to be themes within DHBs' IT environment during 2012/13. There are also ongoing and significant IT developments, such as increased sharing of information between health providers and developing patient portals (for patients to access their health information, book appointments, or communicate directly with their general practitioner).
2.11
There are several risks associated with regionalisation that the DHBs need to mitigate, such as conflicts between regional and local priorities, a single point of failure for the regionalised systems, and a lack of standardised operational procedures.
2.12
DHBs need to ensure that their planning is robust, to properly align local priorities with those in regional and national IT plans. We expect the governance of regional activities to be defined and documented in regional information systems plans.
2.13
The roll-out of the HBL-led national Finance, Procurement and Supply Chain (FPSC) system for all DHBs started in April 2014 with the implementation of the finance system in Hutt Valley DHB (see paragraphs 2.30-2.33). This is part of a significant period of change for DHBs and the wider heath sector, and there will be an increased inherent risk of a breakdown in controls in the transition period, or possibly a move to an ineffective control environment under the FPSC. Effective governance is critical, including that boards monitor change and risk management processes during the change period. Those risks include the possible loss of key personnel or institutional knowledge, as well as any effect on the control environment.
Information security
2.14
Work during our annual audits has shown that more than half of the DHBs need to improve their IT security controls. The most common problems were weak password settings, failures to promptly terminate system access (for example, removing access for staff who no longer work for the DHB), the management of user log-on accounts, and a lack of periodic reviews of users' access rights.
2.15
The main reason we were given for why DHBs were not implementing robust password settings was the potential negative effect on the delivery of health services (that is, password log-on procedures could cause a delay in accessing a clinical system). Several DHBs also told us that they were delaying making improvements as they awaited the implementation of regional and national IT systems and operations, such as the FPSC. It is important for DHBs that delay making IT security improvements to manage associated risks in the meantime.
Business continuity and disaster recovery
2.16
Business continuity and disaster recovery are essential to ensure that vital health services and systems are still working in the event of a disaster. More than half of the DHBs lacked formally documented and tested disaster recovery and business continuity plans. Improvements might be addressed through regional plans and regional operations but, in the meantime, DHBs bear the risk of the absence of formal plans.
Main technology risks for the sector
2.17
In our feedback to entities in the DHB sector, we highlighted that the main technology risks were to do with:
- aligning local DHB plans with regional and national IT plans to avoid duplication of effort and resources;
- IT governance – DHBs (management and boards) need to ensure that they have an adequate understanding of the main information systems risks through, for example, regular oversight by boards of significant strategic projects;
- business continuity and IT disaster recovery – business continuity must be DHB-wide, and IT disaster recovery is an important component of continuity planning and ensuring that critical systems are working within the required period (regional IT plans provide an opportunity to ensure that continuity provisions are highlighted); and
- information security, which is challenging for the sector (DHBs need to ensure that security policies and initiatives are in place, and that they are implemented).
Shared services for district health boards
2.18
Collaborative regional and national initiatives to improve efficiency and save costs in the DHB sector continued to evolve during 2012/13. In this context, the DHB sector includes the 20 DHBs, the regional shared services agencies (healthAlliance, HealthShare Limited, and Central Region's Technical Advisory Services Limited) and the national agencies – HBL and the Pharmaceutical Management Agency (Pharmac) – leading initiatives for shared services and sector procurement.
2.19
The shared services agencies have an increasing role in providing services to DHBs and, in some instances, have been taking on expanded roles and functions. The following sections set out our main findings and risks for the sector.
Health Benefits Limited
2.20
HBL is a Crown company and was set up on 30 July 2010. Its purpose is to facilitate and lead initiatives that reduce administrative, support, and procurement costs for DHBs. It had an initial target of delivering gross sector savings of over $700 million.
2.21
HBL is dealing with a substantial change agenda for the sector in a range of programme areas.8 It is important that HBL has robust programme and risk management and regular, timely reporting to the board and to the sector, to enable it to meet its objectives effectively and efficiently.
2.22
We note that HBL's programme management arrangements are evolving as the programmes progress beyond the initiation phases of the project life cycle. Although some of these changes have arisen as a result of the State Services Commission's Gateway review of the FPSC in December 2012, the changes also reflect a growing maturity of what is a relatively young organisation. The recent establishment of a project management office by HBL will assist with ensuring consistency throughout HBL in terms of programme management requirements, practices, and documentation.
Reporting sector savings
2.23
In our 2013 report on the health sector,9 we described HBL's savings methodology and recommended that HBL continue to improve the transparency of its measurement and reporting of savings.
2.24
HBL reported cumulative (gross) sector savings of $213.5 million to 30 June 2013 and has forecast reaching $764.9 million by 30 June 2016.
2.25
Overall, HBL has improved its reporting of savings, including disclosing the definitions used for the various categories of savings reported. HBL is also providing a better breakdown of the benefits achieved in these savings categories.
2.26
HBL has also revisited its savings methodology, in partnership with the DHBs. HBL will, in 2013/14, report benefits under the categories "budget-impacting" and "non-budget-impacting":
- Budget-impacting savings are those that have a clearly defined effect on the DHB "bottom line" (that is, in the Statement of Comprehensive income, including any depreciation effect).
- Non-budget impacting benefits are those that do not meet the definition of "budgetary". They can include increases in costs that are avoided, benefits carried forward from previous years (budgetary or non-budgetary), and qualitative improvements (such as reduced complexity or reduced clinician time in administration).
2.27
Our 2012/13 audit of HBL also reviewed the assurance processes put in place by HBL to satisfy itself as to the validity of DHB-reported benefits. That review confirmed that the work performed by HBL to date was not yet sufficiently documented or detailed enough for us to rely on. It is important that HBL has confidence in the quality of the savings data in its annual report. We believe that some level of sample verification by HBL would be appropriate, both to satisfy the board that its information is valid and also to identify any common issues that could beneficially be communicated to all DHBs.
2.28
We also recommended that HBL improve its systems for reviewing the savings data that DHBs provide to it. It is important that DHBs ensure that they have appropriate documentation to support their reporting of savings to HBL, which will also support HBL's reporting of savings.
2.29
We will check whether the reporting of savings is adequate and reflects the new benefit definitions referred to above. We are also considering what future work we might do to assess the effectiveness or benefit realisation of sector shared services or procurement initiatives, such as those led by HBL.
National Finance, Procurement and Supply Chain
2.30
During 2012/13, HBL has continued to make progress with national systems and services for the FPSC.
2.31
Last year, we reported that the first two DHBs were expected to move to the new system by December 2013 and the rest of the DHBs by December 2014. The FPSC is now expected to be gradually released to the DHBs over two to three years, starting in April 2014. We encourage HBL to communicate regularly to DHBs on progress and changes to the timetable for implementation.
2.32
There can be good reasons to delay implementing new systems to make sure that the systems and sector are ready for implementation. However, the extended timetable also heightens the need to manage associated risks in an extended period of uncertainty. These can include the loss of key staff, declining staff morale, potential system breakdowns or loss of controls, and a greater risk of fraud. We encourage the sector to keep these risks under review before and during the transition phase.
2.33
Hutt Valley DHB has been the first to move to the new system, followed by Capital and Coast and Wairarapa DHBs. Implementing the FPSC will also be divided into functional phases, such as rolling out the finance system first (this includes the general ledger, accounts payable, and accounts receivable, but does not include payroll), followed by the procurement and supply chain functions.
healthAlliance N.Z. Limited
2.34
healthAlliance has been selected as the future provider of the FPSC shared services to all 20 DHBs.
2.35
healthAlliance was established in 2000 as a joint venture to provide support functions (including procurement, supply chain, finance, information technology, and payroll processing) to Counties Manukau and Waitemata DHBs. In 2011, its scope and ownership was changed to be jointly owned by, and provide shared services to, all four northern DHBs and HBL.
2.36
As the FPSC service is rolled out, healthAlliance will assume responsibility for providing financial transaction processing, financial accounting, and reporting services to successive groups of DHBs. It will also assume responsibility for purchasing and receiving goods and for payments to suppliers. A subsidiary company, healthAlliance (FPSC) Limited, was established in September 2013 to carry out these functions.
2.37
healthAlliance (the parent company) will continue to provide support services to the four northern DHBs until they receive the national FPSC service. Operating in regional and national environments will add complexity and challenges for the healthAlliance Group (the parent and its new subsidiary) because it will be operating in two different environments for an extended period of time.
2.38
This is expected to put a strain on resources. A disruption to service continuity could therefore become a risk for DHBs in the Northern Region. It is important that the DHBs keep this risk under review.
2.39
The expanded role is significant for healthAlliance, and its risk profile has changed and continues to change.
2.40
Capability and capacity are significant risks for the healthAlliance Group, as is the increased risk of control breakdowns, fraud, and loss of productivity. In our audit, we highlighted the need for healthAlliance to ensure that it has the processes, systems, controls, and resources required for its changing and expanding role.
2.41
Effective project management and risk management through the transition is critical. It is also important that healthAlliance works closely with HBL and DHBs to make sure that roles and responsibilities are clear, in particular to avoid overlaps and gaps.
2.42
Although DHBs will be relying on the controls within the shared service centre, the responsibility for effective internal control remains with each DHB's board. It will be important for DHBs, and other entities that receive shared services, to understand and obtain assurance that controls at the shared services centre are appropriate and operating as intended.
2.43
Evolving shared services also present challenges and opportunities for how we audit DHBs and other agencies in a shared services environment. We will continue looking at how we can increase our audit efficiency and improve our effectiveness as these changes develop.
Procurement in the health sector
2.44
More than three-quarters ($10.9 billion in 2012/13) of Vote Health was used to fund services that each DHB provided directly to its population (for example, hospital services) or indirectly through other providers, including non-governmental organisations, PHOs, or another DHB.
2.45
Procurement in the health sector involves billions of dollars and is a major activity for many entities. This includes DHBs' purchasing of services from third-party health service providers (such as rest homes, Māori health providers, and PHOs), worth more than $5.7 billion, collective procurement in DHB regions by shared services agencies, and centralised procurement for all DHBs by Pharmac and HBL. In 2013/14, the Ministry will also directly purchase about $2.8 billion worth of health and disability services.
2.46
We have an ongoing interest in whether procurement policies, practices, and systems are current, effective, and fit for purpose. We are also interested in the changing procurement environment of the DHB sector and the achievement of the intended benefits from new initiatives.
2.47
Procurement services provided through the FPSC will cover only some of the DHBs' procurement, such as hospital supplies. DHBs will still carry out significant procurement activity, including purchasing health services from third parties.
2.48
Our auditors continue to make recommendations to DHBs where improvements are needed to procurement policies or practices. It is important that DHBs ensure that they have up-to-date and good-practice procurement policies and practices to cover their own procurement activities, and which also address procurement in a shared services environment.
Ministry contracting and procurement
2.49
The Ministry contracts with a large number of organisations, including health providers within and outside the public sector, to provide health-related services, worth about $2.8 billion annually.
2.50
In previous audits, we have recommended that the Ministry improve the consistent application of, and compliance with, its procurement policies. To help address this in 2011/12, the Ministry engaged an external reviewer to review national services purchasing and contract management.
2.51
In March 2013, the Ministry established a Procurement Optimisation Programme. The objectives of the Programme are to enhance procurement practices within the Ministry, provide a greater strategic view, and demonstrate value for money. We will follow the progress of this Programme with interest.
Pharmaceutical Management Agency
2.52
Pharmac is a Crown agency that decides, on behalf of DHBs, which medicines and related products are subsidised for use in the community and public hospitals. It was created in 1993 to actively manage government spending on medicines. Pharmac reported that, from 2000 to 2013, it saved DHBs more than $5 billion.
2.53
In recent years, Pharmac has experienced significant change and growth as a result of its increased responsibilities and functions. It is now responsible for managing the national immunisation schedule, establishing the national hospital medicines list, working with HBL, and managing all hospital medical device procurement on behalf of DHBs (by mid-2015). Our auditors reported that Pharmac maintained an effective control environment, and associated internal controls, while it took on these expanded responsibilities in 2012/13.
Asset management by district health boards
2.54
At 30 June 2012, DHBs collectively held about $5 billion of property, plant, and equipment. Many of these assets – $4.3 billion worth – are considered significant (mostly land and buildings). At 30 June 2013, DHBs' property, plant, and equipment had increased to $5.4 billion and their total assets were worth nearly $7 billion (see Part 4).
2.55
Asset management is about effectively managing assets during their economic lives, which includes improving the quality and relevance of information to support decision-making, future service delivery, and asset performance.
2.56
We have an ongoing interest in effective asset management by DHBs and have reported regularly on our work. In 2011, our high-level review of how DHBs manage their assets10 found that most DHBs had not improved how they plan to manage their assets since 2009. In the past two years, we have followed up on our recommendations with individual DHBs as part of our annual audits.
2.57
In June 2013, we published Managing public assets, which reported our findings from gathering information about asset management practice from 340 public entities (those owning assets worth more than $2 million). We gathered information about the regularity of reporting of asset condition information to decision-makers, the extent of deferred maintenance or deferred renewals, and whether the entities had asset management plans.
2.58
We found that 90% of DHBs:
- check the condition of their buildings regularly;
- had documented information on their significant assets; and
- documented maintenance and/or renewal profiles for their buildings.
2.59
We also found that 80% of DHBs carry out planned maintenance or renewal of their buildings.
2.60
However, many DHBs still do not have up-to-date asset management plans. In 2012/13, our auditors reported that more than half of the DHBs needed to update or improve their asset management plans and practices. Some DHBs had delayed updating their plans pending regional asset management plans and a national plan. If a DHB decides to delay updating its asset management plan, then in the meantime it needs to ensure that there is still high-quality and relevant information to support decision-making, future service delivery, and asset performance.
2.61
We expect decision-makers in DHBs to have good information about their assets and future asset needs. We plan to carry out more in-depth work on DHB asset management in our 2013/14 audits. This will include a focus on building and clinical equipment asset classes. Both types of assets are critical to the delivery of public health services.
2.62
The work will allow us to improve our inventory of asset management information, including information about practices for valuation and depreciation, the extent and reliability of physical asset knowledge, asset condition, and asset performance. We intend to report to Parliament on this work.
Canterbury District Health Board's hospitals redevelopment
2.63
The redevelopment of Christchurch and Burwood hospitals is expected to cost more than $650 million and is the largest ever health-related building project in New Zealand. Burwood Hospital is being rebuilt first, including the construction of a new 230-bed facility, and is expected to be finished in stages from mid- to late-2015. There is an expected overlap when construction at Christchurch hospital starts in 2015.
2.64
A Hospitals Redevelopment Partnership Group was established in September 2012 to prepare the final business case for the redevelopment of Christchurch hospitals, which was approved by the Government in March 2013.
2.65
The Partnership Group, with representatives from Canterbury DHB, government departments, including the Ministry, and others in the health sector, is overseeing the project.
2.66
We will continue to maintain our interest in effective governance arrangements for this large and complex project.
Our assessments of public entities' management environment, systems, and controls
2.67
As part of annual audits, our auditors comment on the management control environment, financial information systems and controls, and service performance information and associated systems and controls. We assign grades that reflect our recommendations for improvement (see Figure 4).
Figure 4
Grading scale for assessing public entities' environment, systems, and controls
| Grade | Explanation of grade |
|---|---|
| Very good | No improvements are necessary. |
| Good | Improvements would be beneficial and we recommend that the entity address these. |
| Needs improvement | Improvements are necessary and we recommend that the entity address these at the earliest reasonable opportunity. |
| Poor | Major improvements are required and we recommend that the entity urgently address these. |
2.68
We include the results of our assessments in our audit reporting to management and governing boards. We also report the results to the Minister of Health, the Ministry (as the monitoring department), the three central agencies,11 and Parliament's Health Committee.
2.69
Grades for a particular entity can fluctuate from year to year depending on several factors, such as changes in the operating environment, standards, good practice expectations, and auditor emphasis. For example, a downward shift in a grade might not indicate deterioration – it could be that the entity has not kept pace with good practice for similar entities between one year and the next. How an entity responds to an auditor's recommendations for improvement is important, and the long-term trend in grade movement is a useful indication of general progress.
2.70
Appendix 2 sets out the 2012/13 and prior year grades for each DHB and the other health sector entities that we grade.
Grades for district health boards
2.71
In this section, we discuss the 2012/13 grades and five-year trends in grades for DHBs' management control environment and financial information systems and controls. Part 3 discusses grades and trends in grades for DHBs' service performance information and associated systems and controls.
Management control environment
2.72
Figure 5 sets out our grades for DHBs' management control environments for the past five years.
Figure 5
Grades for district health boards' management control environment, 2008/09 to 2012/13
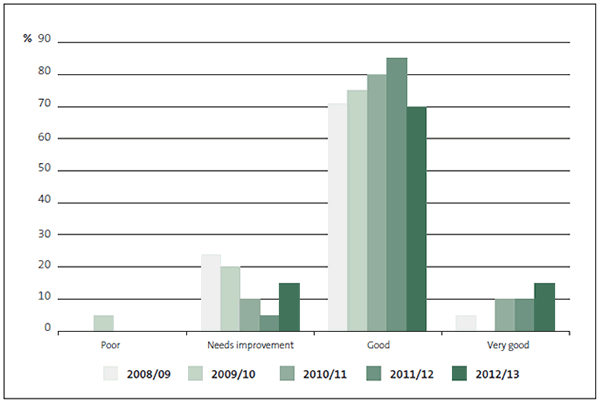
2.73
The grades for DHBs' management control environments show a steady overall improvement in the years to 2011/12, followed by a slight drop in 2012/13. Although one more DHB was graded as "very good" in 2012/13 than in 2011/12, two more DHBs were graded as "needs improvement" in 2012/13 than in 2011/12.
2.74
The grade for Bay of Plenty DHB's management control environment improved from "good" in 2011/12 to "very good" in 2012/13. Two other DHBs (Canterbury and South Canterbury) were also graded "very good" in 2012/13, which is consistent with their 2011/12 grades.
2.75
In 2011/12, one DHB (Capital and Coast) was graded as "needs improvement" and in 2012/13 three DHBs were graded "needs improvement" (Capital and Coast, Lakes, and Southern).
2.76
We changed the grade for Lakes DHB's management control environment from "good" to "needs improvement" because of deficiencies in the control environment, identified after an investigation by the internal auditor.
2.77
The investigation identified that a senior manager and a subordinate colluded with IT suppliers to obtain false invoices. The false invoices were to support accruals for work that had not been done. The manipulation of the accruals was intended to preserve a department's unspent budget in 2012/13. The actions were not in keeping with accounting standards or the expected behaviour of staff members or suppliers. There was no identified personal gain to staff or suppliers and no loss incurred by the DHB. The amount involved was about $316,000, which was corrected prior to the finalisation of the DHB's financial statements.
2.78
The DHB dealt with the staff members involved in keeping with their employment contracts and the DHB's policies.
2.79
We changed the grade for Southern DHB's management control environment from "good" to "needs improvement" in 2012/13 because of deficiencies in the control environment:
- The DHB has used one-off accounting adjustments to secure the deficit position that it agreed with the Ministry, rather than a focus on sustainable solutions to the budgetary position. In 2012/13, an adjustment was used that was not consistent with accounting standards (relating to asset depreciation), which had the effect of reducing the DHB's reported deficit by $3.4 million (from $15.3 million to $11.9 million).
- There was an ongoing and historical dispute between the DHB and South Link Health (SLH), which had not been resolved at the time of our audit. The dispute was about the use of money thought to be held by SLH (possibly about $5 million). The matter was bought to the attention of our auditors, including an allegation that there could be fraud involved. We recommended that, if the DHB considered that there is evidence of fraud, then it should refer the matter to the Police. If not, it should reach an agreement with SLH on future actions. The DHB has since engaged forensic accountants to investigate.
Financial information systems and controls
2.80
Figure 6 sets out our grades for DHBs' financial information systems and controls for the past five years.
Figure 6
Grades for district health boards' financial information systems and controls, 2008/09 to 2012/13
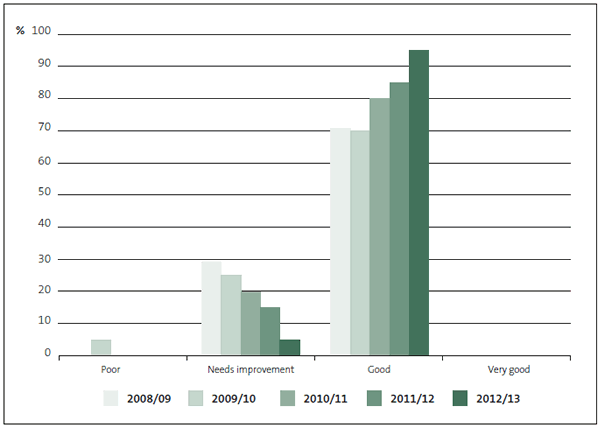
2.81
The grades for DHBs' financial information systems and controls show a steady improvement over the past five years, with only one DHB graded as "needs improvement" in 2012/13.
2.82
We changed the grade for West Coast DHB's financial information systems and controls from "good" in 2011/12 to "needs improvement" in 2012/13. Internal controls and processes in the main financial systems had not been consistently applied during the year because of several staff changes within the financial team and because resources were stretched.
2.83
We increased the grade for three DHBs (Hutt Valley, MidCentral, and Southern) from "needs improvement" in 2011/12 to "good" in 2012/13. These DHBs continued to strengthen their financial information systems and controls.
2.84
DHBs' financial information systems and controls will undergo significant change as they move to the FPSC. Clarity about roles and responsibilities is important. DHBs and service providers need to be clear about what each agency is responsible for in a shared services environment.
2.85
Maintaining the capability of financial and other staff during the transition period is also a potential challenge for DHBs. They will need to manage risks, such as the potential loss of staff and reduced staff morale.
Grades for the shared services agencies
2.86
In our 2013 report on the health sector,12 we included audit results and observations for HBL and the DHBs' regional shared services agencies because of their increasing role in providing services to DHBs.
2.87
Appendix 2 sets out the grades for HBL and Central Region's Technical Advisory Services Limited. For healthAlliance and HealthShare Limited, our auditors provided feedback to management and the boards about the control environment, systems, and controls, and about what improvements were needed. We will grade these entities as part of our 2013/14 audits.
2.88
We discussed our main audit observations and risks for the DHB sector earlier in this Part. They included the need to maintain effective control environment and systems, and that there is appropriate capacity and capability and effective governance for the increasing scope and functions of these agencies in providing services to DHBs.
Grades for the Ministry and other Crown entities
2.89
The grades for the Ministry and the health sector Crown entities were all "good" or "very good" in 2012/13. This means that, overall, these entities maintained robust systems and controls during 2012/13, and that our auditors did not identify any significant concerns. For entities assessed as "good", we recommended improvements.
2.90
The grades for the Ministry, Health and Disability Commissioner, Health Research Council, and New Zealand Blood Service were all unchanged from 2011/12. Of particular note is the New Zealand Blood Service, which was graded "very good" for all three aspects for the second consecutive year.
2.91
The Health Quality and Safety Commission improved two of its grades, from "good" to "very good" for the management control environment and from "needs improvement" to "good" for service performance information and associated systems and controls. This is the second consecutive year that the Health Quality and Safety Commission has improved two of its grades. This reflects continued steady progress in developing its control environment since the Health Quality and Safety Commission was established in November 2010.
2.92
The Health Promotion Agency was established on 1 July 2012 from the merger of the Alcohol Advisory Council and the Health Sponsorship Council. The Health Promotion Agency also took on some health promotion functions previously delivered by the Ministry.
2.93
When entities merge to create a new organisation, there is an inherent risk of an ineffective control environment or a breakdown in internal controls. In our first audit of the Health Promotion Agency, we found that the Agency had managed its change programme effectively and that it had an effective control environment. We graded the management control environment as "very good", and the financial information systems and controls, and the service performance information and associated systems and controls as "good".
Audit results for regulatory authorities
2.94
We audit the 16 regulatory authorities (see Appendix 1) whose members are appointed by the Minister of Health under the Health Practitioners Competence Assurance Act 2003. We also audit two secretariats that each support two or three of the authorities.
2.95
The regulatory authorities are responsible for the registration and oversight of health professions. Each authority prescribes scopes of practice and necessary qualifications for its profession, registers practitioners, and issues annual practicing certificates. The authorities are funded by their professions (through membership fees).
2.96
In February 2011, Health Workforce New Zealand issued a consultation document proposing a single shared secretariat and office functions for the 16 authorities. In late 2012, it funded a detailed business case for establishing a shared secretariat organisation.
2.97
In our audit reports for the 16 regulatory authorities and the two secretariats in 2012/13, we drew attention to uncertainty about the delivery of office functions for the authorities because of a proposal to combine the secretariats and office functions of the regulatory authorities.
2.98
We have drawn attention to this uncertainty in our audit opinions for the past two years. We note the length of time that this uncertainty has remained. Extended periods of uncertainty can elevate risks for entities, such as the risk that staff will leave or that capability might decline, if decisions to upgrade or maintain systems or infrastructure are delayed.
2.99
We understand that the regulatory authorities are now considering other options for improving their co-operation.
7: There are three types of modified opinions: an "adverse opinion", a "disclaimer of opinion", and a "qualified opinion". For a plain-English explanation of audit reports, see The Kiwi guide to audit reports at blog.oag.govt.nz.
8: We described HBL's work programme in our 2013 report on the health sector – see Health sector: Results of the 2011/12 audits, Part 4.
9: Health sector: Results of the 2011/12 audits, Part 4.
10: Health sector: Results of the 2010/11 audits, Part 4
11: The three central agencies are the State Services Commission, the Treasury, and the Department of the Prime Minister and Cabinet..
12: See Health sector: Results of the 2011/12 audits, Parts 2 and 4.

