Part 6: Increasing the supply of scheduled services
6.1
In this Part, we discuss the Ministry's and DHBs' progress in increasing the supply of scheduled services. We discuss:
- increased funding for scheduled services and how it was used;
- changes in the number of patients receiving scheduled surgery;
- improvements in efficiency; and
- the effect on unmet need of providing more treatment.
6.2
According to the Strategy, the backlog of patients waiting for an FSA and treatment had been substantially reduced by 2000. Therefore, any increases in sustainable funding would be used to ensure improved levels of service for newly presenting patients – that is, the level of unmet need would be reduced.
Increased funding for scheduled services
6.3
In the first few years, DHBs used the increases in devolved funding for scheduled services to implement the Strategy. In general terms, they used the extra funding to further reduce the backlogs of patients waiting for an FSA and treatment. DHBs also used it to improve their systems for managing, delivering, and reporting on scheduled services, which also included working more effectively with GPs. At the same time, DHBs were to ensure that patients did not wait more than six months for an FSA or treatment.
6.4
DHBs used two main methods to reduce their backlog of patients. Patients were returned to their GP for reassessment and re-referral as needed, or the DHB held extra out-patient clinics for FSAs and extra operating theatre sessions.
6.5
"Residual waiting list" was the term specifically used to describe the backlog of patients waiting for treatment. Once the Strategy was introduced, DHBs were not allowed to add new patients to these lists. ESPI 4 reports on this. DHBs made good progress in decreasing the number of patients on residual waiting lists. At 30 June 2000, there were about 39,000 patients on the lists. By 30 September 2006, there were only 44 patients on lists nationally. The Ministry regularly reported these improvements in its published annual reports.24
6.6
From 2006/07, a central pool of extra funding for scheduled services was set up within the Ministry. The extra funds paid to DHBs (excluding GST) were about:
- $141 million in 2007/08;
- $197 million in 2008/09;
- $203 million in 2009/10; and
- $220 million in 2010/11 (the budgeted amount).
6.7
These funds were (or will be) used to increase the total number of patients receiving scheduled surgery. Some of the funds were (or will be) used to specifically increase the number of patients receiving cardiac surgery, cataract surgery, and hip and knee replacement surgery. Hutt Valley DHB was allocated funds to provide breast reconstructive surgery for eligible women living in the Capital and Coast, Hawke's Bay, MidCentral, Nelson Marlborough, Wairarapa, and Whanganui DHBs' districts. (DHBs in the rest of the country provide this surgery using their devolved funding.)
6.8
The DHBs had to agree to deliver more treatment services for any extra funds they were allocated in a year. If a DHB delivered more treatment than was agreed, it may have been able to get a top-up from the Ministry to cover its costs. This often depended on whether other DHBs had delivered fewer services than planned, which meant that the Ministry could shift funding between DHBs.
6.9
Because a particular year was chosen as the "baseline" year against which to measure improvements (most recently 2005/06), DHBs were providing different levels of access. This is called "historical inter-regional inequity". DHBs providing comparatively poorer access in 2005/06 were able to use less of their own funding for scheduled services and use proportionally more funding from the Ministry's central pool than other DHBs. The Ministry can also require DHBs to use devolved funding to increase scheduled services before they can access funding from the central pool.
6.10
Each year, DHBs are to provide an agreed minimum quantity of scheduled services. The previous year's treatment levels are the baseline for the current year. However, the quantity of treatment can be increased to make more progress towards correcting historical inter-regional inequity and to meet the applicable Health Target, which requires DHBs to jointly increase the number of surgical operations each year by an average 4000 surgical operations nationally.25 They are to do this and comply with the ESPIs.
6.11
The Ministry is managing this process to achieve a total of 190,000 scheduled operations in 2025/26. In that year, DHBs will need to provide 56,819 more operations than they did in 2009/10 (see Figure 17). Each DHB is expected to eventually deliver an equitable share. The Ministry tells us that 12 DHBs will need to provide between 25% and 90% more operations than they plan to provide during 2010/11.
6.12
Since 2008/09, part of the Ministry's central fund for scheduled services has been allocated to increasing the number of FSAs and procedures provided in out-patient settings to reduce waiting times for patients. The number of FSAs was not publicly reported until 2010/11. This information is provided in the Ministry's caseload monitoring reports on its website. We consider that the number of FSAs is not particularly meaningful. In our view, the number of FSAs does not necessarily reflect the efficiency of the service. In some circumstances, fewer FSAs could indicate an effective care pathway. For example, the need for FSAs can be reduced when GPs are able to order diagnostic tests for their patients.
Changes in the number of patients receiving scheduled surgery
6.13
It took time for DHBs to establish systems to enable an even flow of patients from an FSA to surgery. This meant that, from about 2005/06 to 2007/08, DHBs were not able to use all the extra funding for scheduled services that was available to them.
6.14
Figure 17 shows changes in the number of patients who received scheduled surgery from 1996/97 to 2009/10. The numbers of patients treated decreased after the Strategy was introduced and averaged about 101,400 from 2002/03 to 2005/06. It is apparent from Figure 17 that increased funding from 2006/07 led to increased service provision.
Figure 17
Number of patients receiving scheduled surgery, from 1996/97 to 2009/10
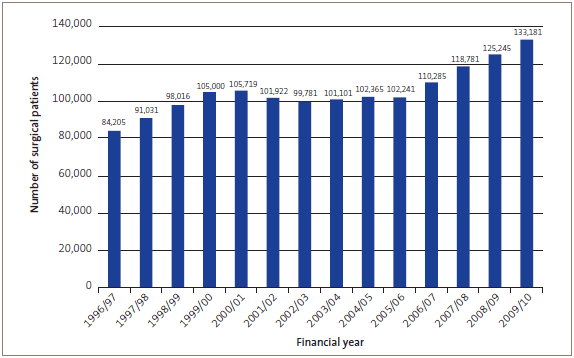
The data in this graph has been adjusted to retrospectively apply changes made to the way surgery was coded. This provides a comparison across years, although some changes may slightly influence the results. The figures differ, substantially in some cases, from earlier data that the Ministry has published. This is because the data is retrospectively adjusted when coding practices change.
Improvements in efficiency
6.15
Evidence of improvements in efficiency tends to be anecdotal. By this, we mean that there are case studies about changes made in one DHB that:
- increased the number of patients seen and/or treated;
- decreased waiting times for patients;
- improved the effectiveness of the working relationship between the hospital and GPs; or
- saved money, which was used to see more patients.
6.16
The projects to make these improvements were usually started because a specialty had long waiting times or were (or were at risk of) turning away referrals for patients who should rightly see a specialist. The projects were successful in ensuring that more patients received scheduled services and received them more quickly.
6.17
We were repeatedly told about the same handful of case studies. This reinforced our impression that a culture of willingness to learn from the experience of others is not widespread throughout the DHBs. When we discussed improvements we had learned about in one DHB with other DHBs, we were often told "But that wouldn't work here." Sometimes, we were told this by another service in the same DHB where a project had been successful.
6.18
Few of the reasons we were given to justify a lack of action seemed to be significant enough to prevent an attempt to achieve similar improvements.
6.19
We consider that every DHB and every specialty providing scheduled services can increase the efficiency of its delivery. Improvements would enable patients and GPs to get more and faster access to specialist advice, reduce waiting times for an FSA and treatment, and reduce the total time for patients to complete their care pathways. DHBs need to ensure that the methods they use to fund scheduled services encourage innovation instead of inhibiting it.
Day-of-surgery admission and day-case treatment
6.20
DHBs have more widely improved the use of day-of-surgery admission (DOSA) and day-case treatment.
6.21
Most specialties and DHBs admit patients on the day of surgery to maximise the use of their in-patient beds. For DOSA to work effectively, DHBs must select appropriate patients and have efficient systems for sending them home on time so that a new patient can use the same bed or chair later in the day. Patients are relied on to begin preparing for surgery at home the night before or on the morning of their procedure.
6.22
Some patients do not need to stay in hospital overnight for treatment. These patients are brought into hospital for the day and go home at night. One DHB told us that it had encouraged each of its hospital's surgical specialties to meet the national and international benchmarks for day-case rates. This has helped the DHB increase its day-case rate for surgery.
The effect on unmet need of providing more treatment
6.23
The Strategy holds several objectives in balance. When more resources are available, DHBs are expected to offer scheduled services to patients with the highest needs and ability to benefit from treatment relative to other patients. Effective prioritisation is needed to identify these patients. DHBs are also expected to offer scheduled services only to patients they can treat within mandated time limits. It is assumed that DHBs will make the best use of the resources available by continuously improving their practices.
6.24
Baseline information about the amount of unmet need in a population is needed for DHBs to know whether increased resources have reduced unmet need. Otherwise, it is difficult to know whether increased service provision has done more than keep pace with population growth or changes in the population's demographic profile. DHBs told us that they need to do more work on this (see paragraphs 5.56-5.57), and we agree.
6.25
In 1993/94, the Ministry considered that the national level of access to publicly funded surgery was roughly comparable to that in similar countries for which data was available. The Ministry reached its conclusion after analysing data for "key marker" cases, which were hip and knee replacements, coronary artery bypass grafts, angioplasty, cataract operations, and prostatectomy operations.
6.26
In late 2003, the Ministry started a project to assess whether orthopaedic patients in five DHBs were receiving similar access to scheduled services. This led to the Orthopaedics Initiative in 2004. A Cataract Initiative started in 2005. Part of each initiative involved increased funding to increase the number of operations for hip and knee replacements and cataract surgery. Targets were set that were largely achieved and/or exceeded.
6.27
The national initiatives were intended to correct perceived failures of DHB-level prioritisation. The patients who received these operations benefited from them. However, a review of the initiatives found that the increased level of service for these patients had generated inequities of access for conditions not covered by the initiatives. This was of particular concern for the care of patients with chronic conditions that can cause permanent, irreversible loss of vision in patients of working age.26 Vision loss from cataracts is reversible.
6.28
Prioritisation tools that are consistently used and continuously audited and updated will gradually produce enough good quality data to better inform the debate about where funding should be allocated and why (see paragraph 5.68).
24: There are several reports that the Ministry is statutorily required to publish each year on behalf of the Ministry, the Director-General of Health, and the Minister of Health. Information about scheduled services was contained in more than one of these reports in most years.
25: Patients receiving scheduled medical procedures do not count towards the Health Target.
26: Gandar, Philip (7 July 2008), A review of the elective services orthopaedic major joint and ophthalmology cataract initiatives: report prepared for the Ministry of Health, www.moh.govt.nz, page 4.
page top
