Part 3: How the Strategy is meant to work
3.1
In this Part, we discuss:
- how scheduled services are rationed for groups of patients;
- how scheduled services are rationed for individual patients;
- whether patients are able to receive scheduled services from other DHBs;
- the pathway from referral to treatment; and
- what happens when ACC declines requests to fund scheduled surgery.
Rationing scheduled services for groups of patients
3.2
In 2004, the Ministry began to set minimum levels of funding for scheduled services. Before an individual patient and GP consider whether the patient needs scheduled services, the Government, the Ministry, and each DHB have already decided how much funding is available for:
- scheduled services, compared to all other services that the Home DHB funds;
- specialties within scheduled services that the Home DHB provides; and
- patients who will be treated by a Treating DHB.
3.3
Ideally, these decisions would be made using information about the health needs of each DHB's population, national priorities, and the cost-effectiveness of scheduled services at the population level and for individuals. In reality, these decisions are affected by a complex interaction of factors, such as:
- hesitation to use economic tools, such as Quality Adjusted Life Years or Patient Reported Outcome Measures, to decide which scheduled services to fund and by how much;
- historical funding and service provision;
- inadequate information about the cost-effectiveness of many treatments;
- increasing sub-specialisation in medicine and surgery;
- local concerns and lobbying by community groups or health professionals;
- the available workforce;
- the DHB's financial situation; and
- the priorities of the Government.
Rationing scheduled services for individual patients
3.4
Rationing is not needed if everyone who needs treatment can have it. However, funding for health care is always limited compared with the demand, and health workforce shortages are a continuing problem. The Strategy accepts that no-one is automatically entitled to scheduled services. Some conditions or levels of health need have no realistic prospect of treatment within the public system.
3.5
Specialists and health authorities have always decided "who will get what", but the methods for reaching those decisions were not necessarily clear and consistent. Conceptually, the Strategy sets out a relatively simple method for systematically rationing the resources available for scheduled services to individual patients. For each patient, the system involves a series of important decisions about whether they could benefit from scheduled services and, if they could, whether the DHB can deliver those services within time limits set by the Government.
3.6
To help reduce unrealistic expectations, some DHBs send to GPs lists of the conditions – such as haemorrhoids, hernias, varicose veins, and bunions – that they do not routinely manage. This is because most patients with these conditions will have low priority relative to other patients. These may not be the same conditions in every DHB.
3.7
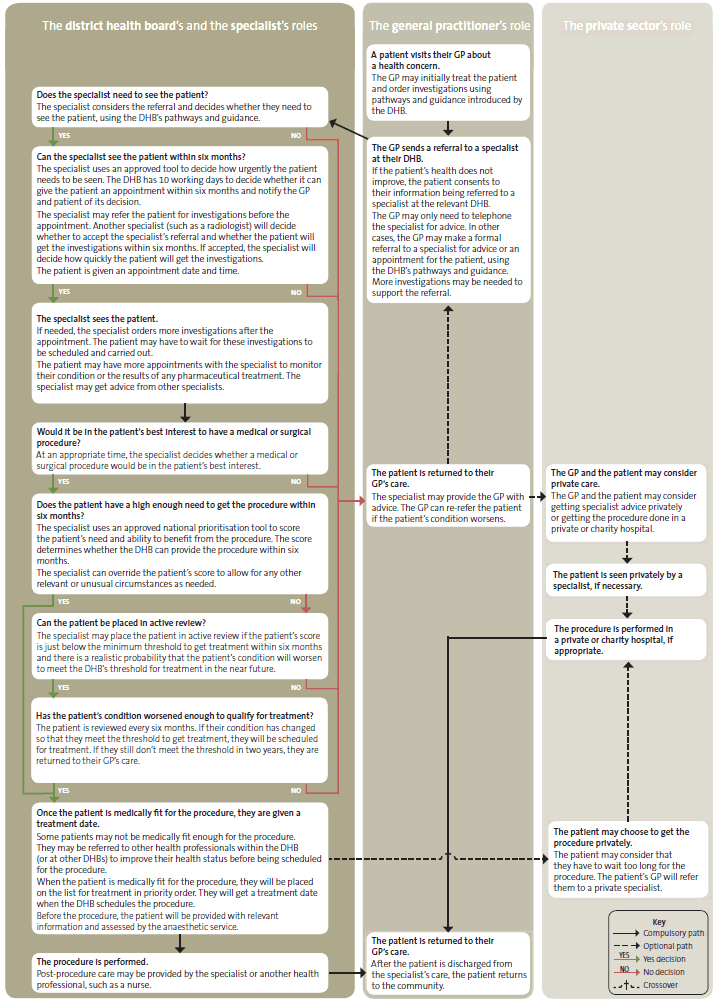
Figure 1 sets out the intended process for making prioritisation decisions. It separates the responsibilities and decisions of the GP, specialist, and DHB in determining whether patients receive scheduled services. In summary:
- With the patient's agreement, the GP decides whether to put the patient forward for specialist advice and/or treatment, and provides information and advice to the specialist.
- The specialist selects those patients who would benefit from an FSA or treatment. The specialist might provide information and advice to the patient and GP about the patient's care, whether or not the patient needs an FSA.
- The DHB decides whether the patient can receive scheduled services within six months (with the existing resources) and provides the administrative system and management support for GPs, specialists, and patients.
Figure 1
Intended process for managing a patient referral for scheduled services
Figure 1 is also attached as a PDF (118kB)
Receiving scheduled services from another district health board
3.8
If the Home DHB does not have the necessary clinical expertise, patients can be referred to a Treating DHB. It is common practice for GPs to send referrals to Treating DHBs without getting the Home DHB's permission. In other instances, a patient will start out with an FSA at their Home DHB. The Home DHB will refer the patient to a Treating DHB when their health needs are clearer. The Treating DHB will prioritise all referrals using its usual criteria, regardless of the source of the referral.
3.9
Each DHB treats its own patients, refers its patients to be treated by another DHB, and treats patients who are the responsibility of other DHBs. Appendix 4 shows how many patients each DHB treated in each category from 2005/06 to 2009/10. Many DHBs treat patients from neighbouring DHBs.
3.10
If the Home DHB has the expertise to provide the scheduled service that a patient is seeking, but chooses not to for an individual patient, the patient and their GP can try to get the service from another DHB. Whether they achieve this depends on the Treating DHB's capacity and whether the patient meets its threshold for treatment.
Getting treatment that is not available in New Zealand
3.11
Treatments not offered in New Zealand may be got from other countries. The Treating DHB can apply to the Ministry for special funding from the Special High Cost Treatment Pool. The Ministry holds the funding on the DHBs' behalf. In 2010/11, the budget for the pool is $2.5 million. Information about the pool is available from www.moh.govt.nz.
Pathway from referral to treatment
3.12
Under the Strategy, patients are cared for in the community until they reach the threshold for hospital treatment. The Strategy prevents the long hospital waiting lists of the 1970s, 1980s, and 1990s by accepting only those patients who meet the thresholds to receive an FSA or treatment within six months.
3.13
These time limits deal with only part of the patient's experience from referral for an FSA to treatment (sometimes known as end-to-end care or the care pathway). For example, the time that patients wait for most diagnostic tests is not monitored. Figure 1 sets out the care pathway for a generic surgical patient, and we give an example of a care pathway that is specific to patients needing a hip or knee replacement in Appendix 5.
3.14
The Health and Disability Sector Standards, which are used to certify DHBs' services, state that patients should receive services (that is, assessment, planning, provision, evaluation, review, and exit) within time frames that safely meet their needs.3
3.15
The Ministry was not able to tell us how long it took for patients to be treated from the time that their referral was received or accepted at each DHB. We were disappointed that these reports were not available by DHB or nationally by specialty.
3.16
We were told that the DHBs have this information (but it may not be readily available), and we understand that they use it to varying degrees to improve the flow of patients through the scheduled services system. We encourage the DHBs to continue with projects to deliver scheduled services to patients in a timely manner. Individual patients will benefit, and DHBs' capacity to treat more patients may increase within the funding that is already available.
3.17
Matters that affect the total time for the patient to progress through the care pathway are:
- access to diagnostic tests and waiting times for these;
- the effect of an increase in the need for unscheduled services on scheduled services;
- potential conflicts of interest for specialists working in public and private sectors; and
- possible "queue jumping" by patients.
Access to diagnostic tests and waiting times
3.18
Access to diagnostic tests plays a critical role in providing effective and efficient scheduled services. For example, a trial at Waikato Hospital showed that it was possible to reduce waiting times for an FSA for patients with suspect skin lesions by using tele-dermatology. Faster access to a suitable diagnostic test meant that patients could be reassured more quickly if their skin lesion was benign or have their treatment arranged and/or provided more quickly if it was not, as either an unscheduled or a scheduled service.
3.19
The need for FSAs can be reduced when GPs are able to order diagnostic tests for their patients. For this reason, the number of FSAs is not especially meaningful for monitoring whether access to scheduled services is adequate. Some DHBs use virtual FSAs to speed up access to diagnostic tests.
3.20
The Strategy discussed access to diagnostic tests in its description of problems with access to scheduled services. Despite this, efficient access to diagnostic tests has not been a consistent and major focus of the Ministry's and DHBs' implementation of the Strategy.
Interaction between unscheduled and scheduled services
3.21
Hospitals need to plan to provide unscheduled and scheduled services. The need to postpone scheduled services because the number of patients needing unscheduled services is more than was planned for can be reduced by good systems and management.
3.22
Postponement is not entirely preventable. Many hospitals have high rates of bed occupancy, which means that relatively small increases in the number of unscheduled in-patients can have disproportionately large flow-on effects. Although an inconvenience – and potentially a cause of increased anxiety for the patient – postponing an FSA or treatment may not necessarily compromise the patient's care (see paragraphs 1.16-1.17).
Potential conflicts of interest for specialists working in public and private sectors
3.23
The public and people working in the public health system sometimes express concern about specialists who work in both the public and private sectors. They consider that these specialists could have conflicts of interest that disadvantage both the public health system and patients who are not able to get treatment privately.
3.24
The main concern is that, during their clinics at the public hospital, specialists may encourage patients to get treatment at a private hospital because they understand that it is likely to be quicker than at the public hospital.
3.25
The risk of this occurring is commonly limited to patients in good general health who need less complicated procedures and who have the ability to pay. Most surgeons and anaesthetists are keen to treat patients at greater risk in a facility that has appropriate back-up. Private hospitals do not necessarily have the services available on site to deal with unexpected major complications or patients with complex health needs. Information supplied by private hospitals to the Ministry for 2005 to 2007 shows that about 99% of patients who funded their treatment privately did not have complex conditions and did not experience complications. (This data might not be complete because, according to the Ministry, some private hospitals do not regularly and routinely provide this data on a timely basis.)
3.26
DHBs' contractual requirements with the Ministry oblige them to tell patients about publicly funded options before the patient chooses to pay for treatment in private facilities. Our observations lead us to consider that this occurs in most instances.
3.27
DHBs are also contractually obliged to offer patients the opportunity for independently vetting any referral that a DHB specialist makes to themselves in a private capacity.4
3.28
We saw letters from a DHB to patients offering them surgery within six months that also made patients aware that their surgery might be available at a private hospital in the district. These letters did not tell patients – and should have – that, before they seek private treatment with the surgeon they had seen at the DHB, they are entitled to get a second opinion from the DHB about:
- their priority score;
- the urgency of any proposed treatment; and
- how long they might wait for treatment at a public hospital.
3.29
We consider that DHBs could also publish general information to this effect on their websites. This would enable patients to independently research their options before and after an offer of treatment is made. It is important that patients are not steered towards using the private sector only because they do not have up-to-date information about the services that are available to them in the public sector.
3.30
Most DHBs do not produce or publish information that is reliable enough to enable specialists to indicate when the DHB can provide treatment. When offering patients scheduled treatment, the Ministry's guidelines require DHBs to write to patients confirming that treatment will be provided within six months, the priority score given, and an estimated time for treatment.5 We saw letters from DHBs to patients that gave a maximum treatment time but did not provide the other information that they should have.
3.31
Some staff at the DHBs we visited told us that they could be more specific about when patients were likely to receive treatment – in some specialties, at least – because they know what the average waiting times for treatment are. However, they were reluctant to be more specific – even to give an indicative range – for fear that patients would complain if scheduled services were not delivered within the estimated period.
3.32
DHBs' complaints management processes are sufficiently onerous that the prospect of an increase in the number of complaints deters staff from giving patients more specific information. We acknowledge that this is a valid concern, but we consider that it is not a reason to prevent DHBs from trying to provide better information to patients and more fully implement the Strategy.
"Queue jumping" by patients
3.33
GPs refer patients to specialists in the private sector for many reasons, such as convenience, location, the patient's preference, and to have a choice of specialist. The GP and patient might not have up-to-date information about waiting times for FSAs and might assume that private is always quicker. If they do have up-to-date information, they will know which is quicker. However, this may not be the only criterion they use in deciding where to seek scheduled services.
3.34
In some situations, the GP may know that the referral will not be accepted by the DHB because the DHB has stated that it does not routinely care for patients with certain conditions. However, after the patient is seen privately, the specialist might consider that the patient would now meet the DHB's threshold for publicly funded treatment.
3.35
Patients diagnosed in the private sector are considered to have "jumped the queue" if they are put onto the waiting list for treatment sooner than they would have been had they had an FSA in the public health system. To prevent this, a DHB can require these patients to have an FSA before being accepted for treatment, even if this means they will see a specialist who could assign a priority score without an FSA.
3.36
DHBs have different views on this matter, and the Ministry's requirements do not specify whether an FSA is needed to assign a priority score. Many people we spoke to about this matter took a pragmatic approach. They considered that patients should be prioritised for treatment regardless of where they had been diagnosed and that FSAs should be scheduled only if this was necessary. They also considered that patients who had received their diagnosis privately had freed up an FSA for someone else. People expressing this view considered that repeating the FSA was a waste of the DHB's resources and the patient's time. We agree.
What happens when the Accident Compensation Corporation declines a request to fund scheduled surgery
3.37
If ACC declines a request from a surgeon for funding to operate on a patient, the specialist can refer the patient to their Home DHB or a Treating DHB or encourage the patient to get surgery privately. If the patient meets the DHB's thresholds, they will be offered scheduled services. We discuss ACC's approach to scheduled services in more detail in Appendix 2.
3: Standards New Zealand (2008), Health and Disability Services (Core) Standards – Continuum of service delivery, NZS 8134.1.3, Standard 3.3, Criteria 3.3.3.
4: Ministry of Health (2010), 2010/11 Operational Policy Framework, page 63, paragraph 4.18.10.c, www.nsfl.health.govt.nz.
5: Ministry of Health (2006), Generic Requirements for Patient Letters.
page top
