Part 3: Planning for discharge from an inpatient unit
3.1
In this Part, we cover discharge planning and:
- the effect of a high demand for beds;
- taking people's broader needs into account;
- involving all appropriate people; and
- systems and tools to support the process.
Summary of our findings
3.2
The Ministry and DHBs expect discharge planning to start between one and seven days after a person's admission to an inpatient unit. This does not always happen. Sometimes people are considered too unwell to start planning in the first few days. High demand for beds also sometimes delays discharge planning.
3.3
Most people have at least a partial plan when they are discharged from an inpatient unit. However, many people are discharged without a plan to meet all their needs, including:
- suitable accommodation – in practice, some people are discharged to unsuitable accommodation;
- finances and support for their employer and/or family; and
- what to do when arrangements break down.
3.4
Some people are discharged at short notice and before they are ready (on a "least unwell" basis, to make space for a "more unwell" person) and before the DHB has had time to set up support in the community. People can also discharge themselves if they are not subject to, or are no longer subject to, the Mental Health (Compulsory Assessment and Treatment) Act 1992.
3.5
When there are high occupancy rates in inpatient units, contact and meetings with people outside the inpatient unit (such as community mental health teams, families, and other health professionals) suffer. People can be discharged with no formal handover to the community mental health team.
3.6
Families are sometimes unable to attend and contribute when care planning or discharge meetings are called or changed at short notice, or are held at inconvenient times. When the patient and their family are involved, they do not always feel listened to.
3.7
The person being discharged and, where appropriate, their family are rarely given copies of discharge plans. Sometimes families are not told, when they should have been, that their family member has been discharged.
3.8
Discharge planning is not well supported by tools and systems. Information about a patient is fragmented between different systems, which makes it hard for mental health staff to gain a clear picture of a person and their needs.
Discharge planning is adversely affected by high demand
3.9
Discharge planning does not always start as early as it should and many people leave the inpatient unit without a plan to address their broader needs, such as getting help with a housing situation or their finances, or support for their employer or family.
3.10
In line with expectations, most DHBs aim to start discharge planning within the first seven days after someone is admitted to the inpatient unit. Two-thirds of respondents to our survey indicated that planning should start 1-3 days after admission. In practice, this does not always happen.
High demand for beds
3.11
Discharge decisions were affected by occupancy pressures on inpatient units at two of the DHBs we visited. One of the DHBs was providing inpatient services for significantly more people than it had beds for (see Figure 5). The inpatient unit occupancy rate for this DHB was particularly high, but our analysis showed that several other DHBs also had high occupancy rates in their inpatient units.
3.12
High occupancy rates in inpatient units mean that sometimes people have to be discharged on a "least unwell" basis to create a space for a "more unwell" person. People are sometimes discharged at short notice, and sometimes without the knowledge of community mental health teams or the person's family.
3.13
Demand for beds can also affect the quality of discharge planning. Short-notice discharges can lead to incomplete assessments, which increases the risk that people who are still unwell are leaving the inpatient unit without adequate support in place. We were told that staff had a backlog of paperwork when occupancy rates were high, including preparing discharge plans before people were discharged. Liaison with others outside of the inpatient unit, for example co-ordinating with the community mental health team, also suffered.
3.14
The short-notice discharges can also put pressure on other parts of the health service. For example, in one DHB, a sub-acute unit was having to treat people who were acutely unwell when it was not set up for this.
Figure 5
Inpatient unit occupancy rate per day for a DHB with a high level of bed pressure, year ended 30 June 2015
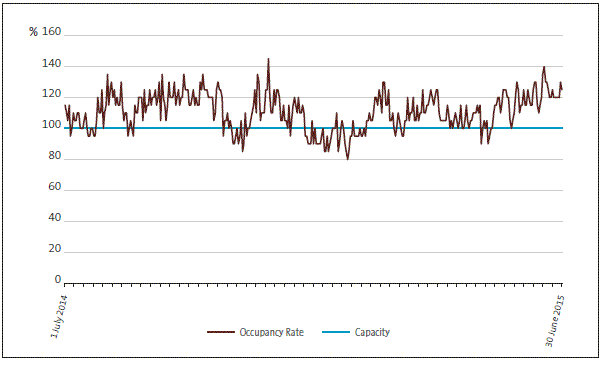
Source: Our analysis of Ministry of Health data.
3.15
We also found that some people could not be discharged because there was nowhere suitable to discharge them to. This reduces the number of beds available for other people. Our data analysis identified about 80 people nationally who have extremely long lengths of stay, which number months or years rather than days.
3.16
We looked at whether occupancy rates were lower for DHBs where there were more beds for every 100,000 people in the local population, and did not find a strong indication that this was the case. This suggests that occupancy pressures are about more than the availability of beds.
Discharge planning often fails to cover broader needs
3.17
Most people have at least a partial plan to meet their mental health needs when they are discharged from an inpatient unit. However, many people are discharged without a plan to meet their broader needs. Sometimes the planning for broader needs does not happen until after a person has been discharged.
3.18
Most DHBs expected a person's broader needs, including needs for services that are not provided by the health sector, to be considered as part of discharge planning. We found a lack of consensus about which needs should be included, and variability in how DHBs assess a person's needs.
3.19
In our case file review, we found that broader needs that were identified were not always included in any formal plan. We also found gaps in planning for early intervention and crisis management. Some staff told us that plans did not cover what to do when arrangements broke down.
3.20
Accommodation needs were more likely to be assessed than anything else, and we saw from case notes that hospital-based social workers were proactive in this aspect. Staff told us they are not supposed to discharge people who have nowhere to stay. In practice, some people were discharged to tenuous or unsustainable accommodation.
There is scope for better collaboration in discharge planning
3.21
All DHBs seek to promote a collaborative approach to discharge planning, involving staff from different disciplines from both the inpatient unit and community mental health teams. Most patients and, where appropriate, their family make some contribution to discharge planning. However, we were told that they could be more and better involved.
3.22
In our view, more could be done to involve all relevant people in discharge planning, even when the demands on inpatient units are high. In particular, we found that communication could be improved:
- between health professionals who are part of a multi-disciplinary team in inpatient units;
- between health professionals and the patient and, where appropriate, their family;
- between inpatient unit staff and community mental health teams; and
- in giving copies of discharge plans to the patient and, where appropriate, their family.
Multi-disciplinary approaches
3.23
Most respondents in our survey agreed that a range of hospital-based mental health staff, including clinical and allied health staff, should be involved in identifying needs. But there are practical difficulties and tensions that can impede this approach. For example:
- although most inpatient units held weekly multi-disciplinary team meetings where a patient's progress is discussed, not all people who should have been at the meetings could attend;
- inpatient unit staff in one DHB told us there was a lack of formal process around multi-disciplinary team meetings;
- notes from the multi-disciplinary team meetings were often not entered into clinical notes; and
- other staff, such as psychologists and occupational therapists, have limited input into a patient's care plan and treatment.
Involving patients and their family
3.24
It is generally considered good practice to involve the patient's family in treatment, including forming a discharge plan, but this is sometimes not appropriate – such as when the patient does not want the family involved, the patient is not in contact with their family, or family involvement is considered detrimental to the patient's well-being.
3.25
Community mental health teams and families were concerned with inpatient unit staff calling, or changing the timing of, care planning or discharge meetings at short notice. Both groups told us that this affected their ability to contribute and be informed. Both groups also told us that sometimes patients had been discharged without their knowledge. Family members who worked during the day were often unable to attend meetings because these were held during office hours. People who work as advocates or advisors for patients reported that when patients and their family were involved, they did not always feel listened to.
Handing over care to the community mental health team
3.26
People were frequently discharged from an inpatient unit without a clearly identified "keyworker" – the person who is responsible for co-ordinating care and support in the community – and without a formal handover to the community mental health team. This increases the risk that people might not receive the support they need after they leave the inpatient unit. In our review of case files, only one-half to two-thirds of people had a clearly identified keyworker. There was no evidence of a formal handover between the hospital and community psychiatrists in one-half to two-thirds of the files we reviewed.
3.27
In the three DHBs we visited, keyworkers could be allocated at short notice or after a person was discharged, or not assigned at all. Late allocation of keyworkers means they may not have met the patient before they were discharged, or may not have been at the discharge planning meeting.
Copies of discharge plans
3.28
Most DHBs expect that patients receive a copy of their discharge plan. This is in keeping with good practice and a patients' rights under the Health and Disability Act 1994 to be informed and involved in their own care. However, we heard that plans were not often shared with patients and sometimes not with community mental health teams. The sharing of discharge plans with patients and community mental health teams by inpatient units is generally poor.
3.29
In most of the case files from the three DHBs we reviewed, neither patients nor their families received a copy of the discharge plan. Responses to our survey indicated that only about one-half of patients, GPs, community psychiatrists, and social workers, and only one-third of families, received copies of discharge plans.
3.30
Some of the reasons we were given for not providing copies of discharge plans to patients and their families included:
- patients would need to make a formal request;
- it is illegal;
- it would upset/distress them (patients) to read it; and
- they (patients) would leave it laying around.
3.31
There was uncertainty among staff in one DHB we visited about what information they could and should share with patients, and some reluctance to share discharge plans. We were told that discharge plans are not generally shared with patients and that discharge documentation is often not prepared until after the person has been discharged, partly because of workload.
Systems and tools do not support effective and efficient discharge planning
3.32
DHBs have a range of tools (such as forms and checklists) and guidance available to help discharge planning. We focused on:
- processes and forms to support needs assessment;
- tools to help refer people to the right services; and
- information systems.
Processes and forms to support needs assessment
3.33
Over half of DHBs have a formal process/checklist to help staff complete needs assessments. These include mental health, physical health, education, employment, and addiction issues. However, during our case file review, we found that there were many forms in use, mostly poorly completed, and often duplicating information. One DHB had three different types of risk assessment forms. None of these forms focused systematically on identifying broader needs.
3.34
In the three DHBs we visited, forms were not always completed properly. There was also no monitoring of whether and how well risk assessments and other forms were completed.
3.35
In our view, forms and checklists for supporting needs assessments could be streamlined and better used. This could help to reduce the pressure on staff and avoid the late or partial completion of discharge plans when occupancy rates are high.
Tools to help refer people to the right services
3.36
All DHBs have documented "pathways" for people entering and exiting the mental health service. These pathways describe the requirements for discharge and admission and explain different treatment and care options depending on what each person needs.
3.37
Some DHBs had good tools to aid referrals to other services. One DHB uses a central list of all services available in that DHB and how to access them. This was a good example of clear documentation to help staff decide where and how to refer people. In our view, there is an opportunity for DHBs to share these good practices and learn from each other.
3.38
Only a few DHBs had tools to help staff refer people to the right services after discharge from the inpatient unit. Few DHBs provided good information about the services available and how to match people to them, based on need.
3.39
Some DHB staff told us that they would like better information about service providers and their performance in improving outcomes. This would help them refer people with acute mental health problems to the most appropriate services available.
3.40
Without formal processes in place, DHB staff use a range of informal processes to connect people to the services they need. In our survey, most respondents indicated that although they draw on a wide range of resources to help them decide which services to refer a person to, the primary source was local and/or previous knowledge. Care pathways was the second most frequently named source of information.
Information systems
3.41
In some DHBs, information about patients was fragmented across different systems, and those systems did not support co-ordinated discharge planning between inpatient units and community mental health teams. For our case file review, we looked at electronic and paper records. On average, we had to look in at least six places to build up a holistic picture of a patient and their needs. A senior manager told us that having a shared care record is fundamental to seamless service delivery.
3.42
One DHB we visited had an integrated computer system that helped the sharing of information between different parts of the mental health service. This DHB was also seeking to improve communication with non-governmental organisations by allowing them access to the DHB's main information technology system.
3.43
Systems at another DHB were not as good at sharing information with non-governmental organisations and primary care services. This hampered assessment and referrals. The DHB did have a system that was integrated with two neighbouring DHBs. This helped keep the records for people who move around, and might enter and re-enter the system in different parts of the region, up to date. However, this system was not integrated with some of that DHB's other systems (for example, its electronic medication system).
3.44
Some DHBs have found practical ways to help support communication between different parts of the mental health service. Some teams in our fieldwork sites had been co-located, such as the acute and community mental health teams, which helped with integration and continuity of care. One DHB also used video conferencing to facilitate communication between services located in different areas.
| Recommendation 1 |
| We recommend that district health boards urgently find ways for inpatient and community mental health teams to work together more effectively to prepare and implement discharge plans, ensuring that all those who need to be – the person to be discharged, family, other carers, and all service providers – are appropriately involved and informed. |
| Recommendation 2 |
| We recommend that district health boards help staff by improving the guidance and tools to support discharge planning (including information systems) so that the information needed for discharge planning can be accessed and brought together easily and efficiently. |
| Recommendation 3 |
| We recommend that district health boards regularly review the standard of discharge planning and follow-up work to identify and make improvements. |

