Part 5: Suicide statistics and reports
5.1
In this Part, we discuss:
- how mortality data is collected;
- the Ministry of Health's reports on suicide statistics; and
- the factors affecting when mortality and suicide statistics are released.
How mortality data is collected
5.2
Collecting suicide statistics is part of the wider system for recording births, deaths, and marriages, and for collecting mortality data. Mortality data is used to identify population groups that experience diseases or injury disproportionately, show high-level progress in reducing preventable deaths, and set research priorities.
5.3
The New Zealand Mortality Collection (the Mortality Collection) is a database that was established in 1988. (Data from earlier years is held elsewhere.) It holds data on causes of death, and personal details about a person such as their name, sex, and age. Data is collected for all deaths registrable in New Zealand, including stillbirths. An international coding system is used to code the main and any secondary causes of death. The Ministry of Health sends data to the World Health Organization for use in international comparisons.
5.4
Figure 5 indicates how data is collected, processed, and disseminated. It shows the relationship between coronial inquiries and reports, the Births, Deaths, Marriages, and Citizenship Registry, and the mortality collection and other data sources. It also shows some of the checks that are made to ensure that data is accurate. The figure refers to the Mortality and Demographic Data and Suicide Facts reports, which we discuss in this Part.
Figure 5
Overview of mortality data collection, processing, and dissemination
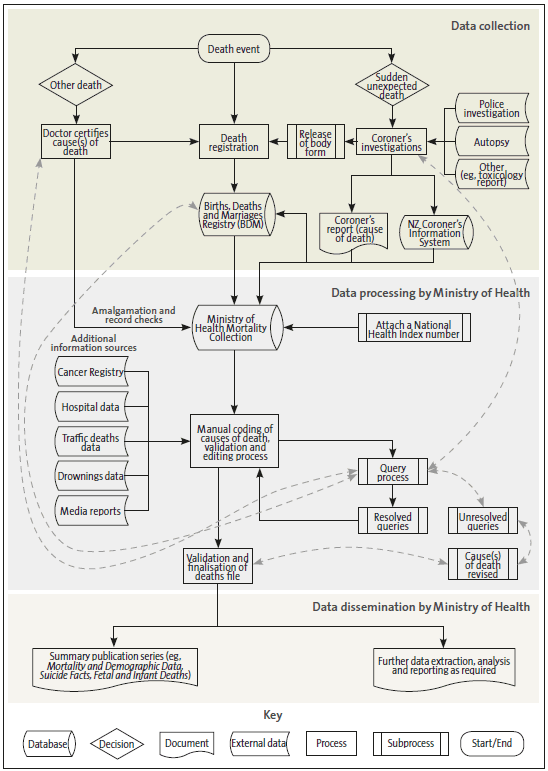
Note: This chart appears in every Mortality and Demographic Data report. Source: Ministry of Health.
5.5
The staff working with the Mortality Collection are long serving and their experience in data validation helps improve the quality of coding, and so confidence in the statistics. The Ministry of Health checks on the quality of coding. One way to do this is to compare the percentage of deaths where a cause has not been identified with the same codes in other countries. A low percentage of deaths coded to non-specific causes is good. The Ministry found that for 2011, the percentage of deaths coded to selected non-specific causes was about 1.7% for New Zealand, 4.3% for Australia, 5.3% for England and Wales, and 5.4% for Canada.
Reports on suicide statistics
5.6
In our view, there are three purposes for reporting population-level data on suicide:
- making detailed data tables publicly available as soon as possible, for anyone to use;
- informing the Ministry of Health's analysis of the data and comments on major suicide trends; and
- producing regular reports, for accountability purposes, on progress in reducing suicide rates.
5.7
The Ministry of Health's reports mostly meet our expectations, although some improvements could be made.
5.8
The Ministry of Health publishes online data tables for all causes of death (including suicide) and more detailed data tables for suicide and non-fatal intentional self-harm.
5.9
Data tables for all causes of death are published along with the Mortality and Demographic Data series of reports. The data tables are released online before the Ministry of Health's written report is prepared and released. This makes the data available promptly to other government agencies and the public so that it can be used as soon as possible.21
5.10
Data tables for suicide are published as part of the Suicide Facts series of reports. The data tables and the written reports are published at the same time. The reports also give an in-depth look at data for people treated in emergency departments for non-fatal intentional self-harm who stayed in hospital for one night or longer. It is common practice for this to be reported with the aim of finding intervention points to prevent suicide. We consider that the data tables could be released as soon as they are ready, rather than withheld until the reports are also ready.
5.11
For both series of reports, the Ministry of Health publishes analysis and commentary on the data in a written report, and discusses notable trends. Because the Mortality and Demographic Data reports focus on the leading causes of death, they discuss suicide.
5.12
The Suicide Facts reports look in depth at the latest year's demographic data on suicide, and discuss trends.22 The Ministry of Health is clear that its data and reports do not explain causes of suicide and non-fatal intentional self-harm, or give reasons for changes in the data. This is because it is difficult to attribute changes to particular events or actions (see Part 2). We suggested, and the Ministry agreed, that the Suicide Facts would have more value if they focused on trend reporting (see Part 2). In our view, limited insight can be achieved from a detailed examination of a single year's demographic suicide data.
5.13
Both series of reports help the Ministry of Health to meet its responsibility to report mortality statistics generally and to report on progress in reducing suicide (see also Part 2).
5.14
These two series of reports are the main source of statistical information about suicide. We found the format and content of each set of reports is largely consistent from year to year.
5.15
We consider that both series of reports are fit for purpose and well presented. Nevertheless, we suggested some relatively minor changes that we consider would improve them. The Ministry of Health has already started work on adopting some of our suggestions and is considering how others could be taken up.
5.16
We suggest that the Ministry of Health:
- use consistent starting years for trend reporting to avoid the risk of biased reporting;23
- comment when changes in suicide rates are statistically significant, to prevent relatively small year-to-year changes being misinterpreted;
- make more use of confidence intervals for selected suicide data to make the potential range of error clear;
- report only suicide rates that are statistically credible;24
- make the Suicide Facts data tables available online as soon as they are ready to publish so that people can use them;
- include statistics on deaths from undetermined intent in the Suicide Facts reports;25
- change the Suicide Facts reports to focus on trend reporting; and
- include a technical note in the Suicide Facts reports that when coroners do not specify whether self-inflicted poisoning is accidental or with intent to harm, the coding rules require the death would be coded to accidental poisoning (not undetermined intent). The note should also explain that this rule could lead to an overstatement of accidental poisonings and an understatement of deaths from undetermined intent.
5.17
In May 2016, the Chief Coroner issued a practice note intended to improve the quality and consistency of findings. It includes a requirement for coroners to specify in their Certificates of Findings whether or not they have found a death to be suicide. We consider that adopting the practice note will ensure that coroners' decisions are clear to the bereaved and to agencies. It will reduce the risk of overstating accidental poisonings and understating deaths from undetermined intent.
Looking ahead
5.18
During our audit, it became clear that some proposed changes in the next 12-18 months could affect the way suicide statistics are reported. Such changes include:
- whether a Suicide Mortality Review Committee is re-established and how it will report on its work;
- the implementation of the new suicide prevention outcomes framework; and
- the release of an updated New Zealand Suicide Prevention Strategy and new suicide prevention action plan.
5.19
We asked the Ministry of Health to consider a "stocktake" of suicide publications to be clear about each report's contribution to good quality information about suicide. The Ministry and the Health Quality and Safety Commission should aim to prevent "data clutter", which is a risk when data is published in multiple reports using data extracted on different dates.
5.20
We are pleased by the Ministry of Health's early response to our suggestions and encourage them to discuss their plans with stakeholders, such as the Health Quality and Safety Commission, the Ministry of Justice, the Chief Coroner, and frequent users of the data (such as researchers). The Health Quality and Safety Commission told us that it supports a stocktake, even if a Suicide Mortality Review Committee is not re-established.
When statistics are released
5.21
To ensure public confidence in mortality statistics, the Ministry of Health waits until it holds full information on nearly all deaths before it publishes data and reports on the cause of death for a specified period (a calendar year). The pace at which coronial inquiries are completed is the main factor affecting data completeness.
5.22
For the Mortality and Demographic Data series, data is considered good enough to publish when there are fewer than 10 deaths remaining for the reporting period on which nothing is known or the cause of injuries is unknown.
5.23
For the Suicide Facts series, data is considered good enough to publish when there are fewer than 30 remaining deaths on which nothing is known or the cause of injuries is unknown. Because there could be up to 30 deaths on which data is missing (which is a lower standard than applied to the Mortality and Demographic Data report), the Ministry of Health considers that the latest year's suicide data is provisional. In this case, provisional means that the number of suicides could increase until all coronial inquiries for that year are complete. To decide when to publish, the Ministry considers three factors:
- the total number of deaths awaiting coroners' decisions (not the total number of suspected suicide deaths awaiting coroners' decision);
- whether staff have been able to assign provisional codes for some deaths using available data; and
- whether data processing is complete.
5.24
Reports are published when these completeness requirements are met, which is why data for a reporting period is published between two and three years later and reports may not be published at the same time each year. If all (or nearly all) coronial inquiries could be completed sooner (see paragraph 6.29), the Ministry of Health would be able to publish mortality statistics sooner.
5.25
Any missing information is included in later reports and any errors corrected, which is why the latest report always has the most reliable data. The latest report is also the most reliable because there could have been changes to the way that data is coded. When such changes are made, the Ministry of Health usually recalculates older data using the new method so that data can be compared.
Conclusions
5.26
The Ministry of Health produces two series of reports that make detailed statistics on suicide available to the public. The reports are made up of detailed data tables and written reports that discuss the Ministry's analysis of the data, including trends. The reports help the Ministry meet its responsibility to publish mortality data and report on progress in reducing suicide.
5.27
We consider that the Ministry of Health's reports on suicide statistics are fit for purpose. Nevertheless, we suggested some relatively minor changes that would improve them. The Ministry welcomed our suggestions and is already planning to implement some of them in 2016 and others in 2017.
5.28
When statistics are released depends on the time taken to complete coronial inquiries. If inquiries could be completed sooner, the Ministry of Health could publish mortality data sooner.
21: In the Mortality and Demographic Data reports, suicide is called "intentional self-harm". There are 17 different codes for suicide. Two codes are for "intentional self-harm by smoke, fire, and flames" and "intentional self-poisoning by and exposure to narcotics and psychodysleptics [hallucinogens] not elsewhere classified". There are other groups of codes for self-inflicted accidental deaths and self-inflicted deaths of undetermined intent (that is, the coroner did not decide whether death was accidental or intentional).
22: Data is reported by sex, ethnicity, age, deprivation quintile, DHB, and suicide method. The last three reports also included data by urban/rural profile.
23: The Ministry has used a range of starting dates for trend reports. We suggested that it select two or three starting dates and use them in all their reports. For example, we suggested that they pick one starting year for historical reporting (such as 1948 or 1950, which are currently used) and another showing more detailed trends for a minimum of 20 years. This is partly because three-year moving averages are not useful for shorter periods, such as 10 years. There is also a time lag between changes in society and suicide rates, which are more obvious over longer periods.
24: The Ministry of Health publishes suicide rates for each DHB. We questioned the value of the results produced for some DHBs when the range of error is more than half of the data range.
25: Coroners may not to be able to decide whether someone's death was an accident or suicide because the person's intent was unclear or there was a lack of evidence. From a suicide prevention perspective, the person's intent is not necessarily the only factor determining which deaths could or should be studied. The method is also important. Looking at data on deaths from undetermined intent helps to increase the opportunities to prevent suicides and accidental deaths by the same methods. Because the number of suicides is relatively small compared to deaths from other causes (such as ischaemic heart disease) it is harder to spot patterns below the population level. This makes it harder to work out how to intervene to prevent suicide and to determine whether prevention actions are effective. We noticed that the Scottish Government uses data on "probable" suicides (deaths from suicide and undetermined intent) to assess and report on progress in preventing suicide. See The Scottish Government (2013), Suicide Prevention Strategy 2013-16, www.scotland.gov.uk.

