Part 2: Audit results for 2014/15
2.1
In this Part, we discuss the 2014/15 audit results, including:
- observations and matters arising from the 2014/15 audits; and
- our assessment of the management control environment, systems, and controls for DHBs and other health sector entities.
2.2
The main matters arising from our audits relate to:
- the non-standard audit reports for all DHBs and the Ministry regarding performance information derived from third parties;
- shared services and other initiatives to increase cost-effectiveness and savings;
- procurement and contract management;
- the earnings management practices of some DHBs;
- information systems and controls;
- the transition to public benefit entity accounting standards;
- DHBs' performance reporting on appropriations;
- the Canterbury hospital rebuild projects; and
- DHBs' asset management.
2.3
We discuss DHBs' financial results and performance in Part 3.
Observations and matters arising from the 2014/15 audits
Non-standard audit reports because of third-party performance information
2.4
In 2014/15, we issued non-standard audit reports for all DHBs and for the Ministry of Health because some important performance measures used by the DHBs, including some of the national health targets, rely on information from third-party health providers, such as PHOs. The DHBs' control over much of this information was limited, and we could not obtain evidence to assure us of the reliability of the information from third parties that was used by DHBs to report.
2.5
We first issued non-standard audit reports for all 20 DHBs over this matter in 2012/13. We reported on it in detail in our health sector report for that year.
2.6
Our non-standard audit reports do not mean that the health target performance reporting by DHBs was incorrect, or that the DHBs' service delivery failed, or any wrongdoing or false reporting by DHBs, or that the information reported by general practitioners was wrong. It means that we could not verify some important performance information because we do not audit PHOs.
Performance reporting by district health boards still reliant on unaudited third-party reporting
2.7
DHBs report their performance against a number of measures. Because DHBs have overall responsibility for health services to the people in their districts, they report not only on the performance of the services they deliver themselves through their hospitals, but also on some services provided by others, such as general practitioners and PHOs.
2.8
For example, the measure for the national health target for smoking prevention is the percentage of smokers offered brief advice and support to quit smoking when being seen by a health professional in a PHO or a public hospital.
2.9
The primary smoking prevention measure relies on information from general practitioners. We could not test this information independently because our audit mandate does not extend to information held by general practitioners or PHOs. Also, the DHBs could not give us evidence that they were checking that the information reported to them by third parties was reliable.
A sector-wide issue affecting all district health board audits
2.10
The qualification relating to third-party performance information is a sector-wide issue that has affected the audits of all DHBs and the Ministry.
2.11
The Ministry reports the results against national health targets as measures of its impact. This information is reported to the Ministry by DHBs. We qualified our audit opinion for the Ministry for the same reason that we qualified those of the DHBs.
2.12
DHBs pay about $5.9 billion to other providers of services, of which $4.4 billion is to third parties such as PHOs and general practitioners, and it is important that there is reliable performance information about these services to support decision-making and to ensure public accountability.
Work to address this issue is continuing
2.13
In our audits, we recommended that the Ministry and DHBs work together, and with other relevant organisations, to devise a cost-effective way to get sufficient assurance over performance information from third parties. Because this is a sector-wide issue, we encourage the sector as a whole to consider whether the introduction of additional controls is appropriate and would be cost-effective, and, if so, how best to introduce them.
2.14
The Ministry has taken the lead in trialling an approach that might be helpful. The Ministry developed a methodology for auditing the data that general practitioners provide to PHOs, which the PHOs then report to the DHBs. We are pleased to see this progress. It is too early to say whether solutions will be available in time to affect the results of the 2015/16 audits.
Other non-standard audit reports
2.15
As well as the qualification relating to third-party performance information, we further qualified our audit opinions on Wairarapa DHB, and Capital and Coast DHB. These qualifications related to performance information reporting for their hospital services, and applied to the 2013/14 comparative information only – that is, we issued qualified opinions for the DHBs for certain measures in 2013/14. These results were reported again in 2014/15 so that readers could compare performance of the DHBs from one year to the next. Our audit opinion for Lakes DHB was also qualified for these measures in 2013/14, but the DHB chose not to report the comparative information in 2014/15. We were pleased to see that the problems that had led to these qualifications had been resolved by the DHBs for the 2014/15 performance information.
Shared services – initiatives to increase cost effectiveness and savings
2.16
Considerable efforts continued in the sector to increase effectiveness and achieve savings by using shared-services agencies. Below are summaries of the results of our audits of these entities.
Health Benefits Limited
2.17
HBL's financial statements were prepared on a non-going-concern basis, as its assets and liabilities were transferred to a new company, NZ Health Partnerships Limited (NZHP) on 1 July 2015.
2.18
HBL reported savings of $72.6 million in the sector for 2014/15. This makes cumulative sector savings of $374.4 million since HBL began reporting them.
2.19
In previous years, we found that HBL had difficulty securing verifiable information from DHBs about the benefits that were being realised and then reported on by HBL. We made recommendations for improving the transparency of HBL's reporting, and over time we have observed some improvements in this area, including the enhanced checking of savings reported by DHBs.
2.20
In 2014/15, HBL further improved their reporting of benefits by providing, for the first time, a breakdown of benefits from applying its savings methodology. This allowed it to report "budget-impacting" and "non-budget-impacting" savings separately. The two kinds of savings are defined as follows:
- Budget-impacting savings: those with a clear effect on the DHB's "bottom line" (that is, in the Statement of Comprehensive Revenue and Expense, including any depreciation effect).
- Non-budget-impacting savings: those that do not meet the definition of budgetary. They may include increases in costs that have been avoided, benefits that have been carried forward, and qualitative improvements (such as reductions in complexity or clinicians' time spent on administration).
2.21
Both types of benefits are reported as dollars saved. In 2014/15, budget-impacting savings were $20.1 million, and non-budget-impacting savings were $52.5 million.
2.22
Despite the improvements we note above, HBL still found it difficult to report benefits in 2014/15. There was a notable deterioration in some DHBs' communication with HBL, with long delays in providing HBL with information about savings they had realised. Four DHBs did not respond to requests for confirmation of benefits to be reported. Delays in establishing the National Infrastructure Programme also resulted in benefits initially recorded for the programme being removed from the final annual report.
2.23
Because of these challenges and delays, HBL breached section 156(1) of the Crown Entities Act 2004. This requires HBL to forward its annual financial statements and certain other information to the Auditor-General within three months of the end of the financial year, and to forward its annual report in time to allow the Auditor-General to review it and provide an audit report within four months of the end of the financial year.
2.24
HBL's successor, NZHP, will clearly need to work hard to establish and maintain effective communication channels with DHBs. This is vital to the successful delivery of shared-services programmes. As part of our audit, we made a number of recommendations on ways to improve matters.
healthAlliance N.Z. Limited
2.25
healthAlliance N.Z. Limited (healthAlliance) is owned by the four northern region DHBs. It was established to provide "back office" functions (procurement, supply chain, finance, information systems, and payroll processing) to generate efficiencies and savings for the shareholding DHBs.
2.26
In July 2014, healthAlliance (FPSC) Limited, a subsidiary of healthAlliance, began running the National Procurement Service, which is available to all 20 DHBs. This service provides a national catalogue of goods and services, with a view to reducing costs and increasing savings for DHBs. Goods and services made available in this way include clinical supplies and non-clinical support services.
2.27
healthAlliance (FPSC) Limited also manages the Oracle financial management platform for Hutt Valley DHB. When Hutt Valley DHB started using the platform in April 2014, it was the first (and remains the only) DHB to do so.
2.28
healthAlliance has expanded to take on these new functions while continuing to provide services to its established clients in the northern region. The resulting challenges have been further complicated by the disestablishment of HBL and its replacement by NZHP. We noted the uncertainty affecting healthAlliance (FPSC) Limited while NZHP decides how to continue the programmes it inherited from HBL.
Pharmaceutical Management Agency
2.29
The main role of the Pharmaceutical Management Agency (Pharmac) is to manage the list of subsidised medicines formally known as the Pharmaceutical Schedule. Since 2010, the Government has expanded Pharmac's area of responsibility to include helping DHBs to purchase vaccines, and medicines and medical devices for hospital use.
2.30
Pharmac is well established in the management of the Combined Pharmaceutical Budget and has had notable success in securing savings on pharmaceuticals. But it is still developing its approaches in its newer areas of responsibility, which could take several years to reach similar maturity.
2.31
To secure the greatest possible savings for DHBs, Pharmac expects to progress to full budget management of the purchase of hospital medicines and medical devices, of the kind it currently exercises over the Combined Pharmaceutical Budget. However, making this transition will require Pharmac to have access to accurate purchase and usage data from DHBs.
2.32
Our audit did not find any negative effect on the control environment and associated internal controls from Pharmac's growth and expanded responsibilities. We noted that Pharmac is working closely with stakeholders to help it achieve the best outcome.
Procurement and contract management
2.33
DHBs spend a large portion of their funding on procuring goods and services. Each DHB needs to carefully manage a number of major contracts to ensure that the DHB and the public receive what is being paid for. Many DHBs are engaged in large projects or programmes that also need sound procurement and contract management processes.
2.34
Procurement in the DHB sector is complex because of the role of other parties in helping the DHBs manage procurement. On a day-to-day basis, the Ministry provides the important service of processing the DHBs' payments for nationally contracted services. A number of regional and national initiatives also involve other parties providing procurement services for the DHBs – for example, the national procurement service run by healthAlliance (FPSC) Limited.
2.35
For some years now, our audits of DHBs have identified potential improvements in aspects of procurement and contract management, such as updating procurement policies and practices to ensure that they are in line with the Government Rules of Sourcing and with good procurement practice. In general, DHBs have been slow to address these findings. We understand that DHBs have possibly deferred improvements because they were expecting national and regional initiatives for procurement services to provide solutions, or to change processes to the extent that improvements made now would need to be redone.
2.36
Although shared services and systems will have an increasing role in DHB procurement, it remains the individual DHB's responsibility to ensure that they have robust and effective procurement and contract management. DHBs need to be confident that their policies and processes provide sufficient assurance. We will continue to monitor this and tell DHBs where we consider improvements are needed.
Earnings management practices at district health boards
2.37
As we have reported in previous health sector reports, DHBs are very focused on meeting their forecast financial targets.
2.38
During our 2014/15 annual audits, we observed that some DHBs seemed overly focused on achieving a particular "bottom line" result. Our auditors noted that DHBs are managing their financial results carefully with the objective of reporting close to break-even results or budgeted surpluses or deficits. We noted that a number of DHBs could not support the way they had accounted for some revenue and expenditure, because of judgements made about accruals, provisions, asset lives, and estimated leave liabilities. Some DHBs chose not to adjust for misstatements that we found, if adjusting would significantly affect their financial positions relative to their budgeted positions. Where we found this was happening, we reported it to the DHB and included it in our reporting to the Minister and to Parliament.
2.39
Although this "bottom line" focus and financial pressure on DHBs has been present for a number of years, it seemed to be more evident in the 2014/15 audit round.
2.40
In no instance did our auditors consider these issues serious enough to affect the audit opinion. Nevertheless, DHBs need to approach financial year-end cut-offs and valuation assumptions consistently, without bias toward the desired year-end result.
2.41
We will continue to focus on this issue in 2015/16 and beyond.
Information systems and controls
2.42
In our annual audits, we consider IT controls that affect the reliability of the financial statements and service performance reporting. This involves assessing general IT controls, business application controls, and data analysis.
2.43
Balancing IT business requirements against the availability of resources is a continuing challenge for DHBs. We are interested in DHBs' information service risks, particularly in the regionalisation of IT operations, business continuity and disaster recovery, information security, emerging technologies, and the role of IT in governance.
Progress in addressing risks of regionalisation and collaboration for the IT environment
2.44
In our previous health sector report,6 we discussed the potential risks to DHBs' information controls in an environment of increasing regionalisation, collaboration, and shared services. These risks arise from conflicts between regional and local priorities, a single point of failure in a regionalised or national system, and a lack of standardised operating procedures.
2.45
We have recommended that DHBs plan carefully, to align local priorities properly with those in regional and national IT plans, and that governance arrangements for regional activities be clearly defined in information systems plans.
2.46
In the last year, we observed a marked improvement in this area. Although the risks we note remain, we are satisfied (after our 2014/15 audits) that the sector has reasonable processes and controls for ensuring that significant risks relating to regionalisation are promptly recognised, mitigated, and reported. We were pleased to see this progress in response to our recommendations.
Business continuity and disaster recovery still a risk
2.47
The lack of formal disaster recovery plans remains a risk for DHBs. Close alignment is needed between the disaster recovery plan and the expectations set out in business continuity plans. Provisions for business continuity planning must be seen as a DHB-wide initiative rather than as a task for the IT department. IT disaster recovery is a key component of continuity planning, to ensure that crucial systems are up and running in the required time.
2.48
The sector's disaster recovery systems can potentially benefit from NZHP's development of the National Infrastructure Platform. To use the platform, DHBs are expected to move their data to two data centres that meet government standards for information security and resilience, in line with the "Information as a Service" model developed by the Government's Chief Information Officer. However, this programme will take some years to complete. In the meantime, DHBs need to consider how to manage their disaster recovery risks.
DHB governance – better strategic understanding of IT needed
2.49
The reliance of DHBs on information systems and technology for effective and efficient delivery of healthcare services is increasing. Now more than ever, executive management and boards need to ensure that they understand the information systems risks a DHB faces. We encourage boards to regularly examine strategic IT projects and related risks, as routine good governance practice.
Information security needs closer attention
2.50
DHBs need to devote more attention to information security, particularly at the network level. We continue to note issues, including weak password settings and a lack of periodic review of user access rights. This is particularly important given the large amount of sensitive information that DHBs are responsible for. These observations have been consistent for the last five years.
2.51
Some DHBs have formal information security arrangements, but most DHBs' information security arrangements are on a "best efforts" basis. We continue to recommend that DHBs work at improving the security of their information.
2.52
However, we have seen some improvement in this area. The number of security-related issues we have found in the DHB sector declined in the last three years. Although the pace is slow, the trend is positive.
2.53
We note that the topic of information security is gradually gaining attention outside of IT departments. Given its importance to entities that manage large amounts of sensitive information, a whole-of-entity approach to information security is needed.
The transition to public benefit entity accounting standards
2.54
The 2014/15 year was the first in which DHBs were required to comply with public benefit entity (PBE) accounting standards. These standards have been developed recently by the External Reporting Board7 for entities whose primary objective is to provide goods or services for community or social benefit, and where equity has been provided to support the pursuit of this primary objective rather than a financial return. The new standards require DHBs to consider how they account for revenue and expenditure, using new definitions. Because we were aware that this could require some time and effort on the part of DHBs, we reminded them of the need to prepare for the new standards.
2.55
In general, we found that DHBs were poorly prepared for the transition to the PBE accounting standards, and additional time and effort were needed in the audit to ensure that DHBs accounted for their revenue appropriately.
2.56
It is essential that public entities apply accounting standards correctly so that people can rely on the accuracy of their reported information, and can compare the performance of one entity with another.
2.57
Despite these problems, the transition to the new PBE accounting standards did not much affect the DHBs' financial results. The transition had no opinion implications, and all DHB audits were completed on time.
2.58
This will remain a focus for auditors in 2016, but we expect it to become routine as DHBs become more familiar with the new standards.
District health board reporting on appropriations
2.59
Some changes to the Public Finance Act 1989 and Crown Entities Act 2004 came into effect in 2014/15. One of them was the requirement, under section 19C of the Public Finance Act, for some Crown entities to report information about appropriations if this was required explicitly in the Estimates of Appropriation. The Estimates for DHBs are set out in Vote Health, which specified DHBs as performance reporters for some appropriations.
2.60
As the appropriation administrator for Vote Health, the Ministry is responsible for ensuring that the relevant health-related entities are aware of their reporting obligations. During 2014/15, the Ministry did not communicate adequately with DHBs about their obligations to report. As a result, DHBs did not report the required information. However, the aggregated information for all DHBs is included in the Minister's reporting (as required by section 19B of the Public Finance Act). The Ministry's annual report also includes a reference to where the information can be found.
2.61
DHBs disclosed the non-reporting in their annual reports and also stated where the information could be found.
2.62
We recommended that the Ministry ensure that it communicate adequately with DHBs in future on their reporting requirements, so that they can report the information required by legislation.
Canterbury District Health Board Facilities Development Project – new governance model
2.63
The Canterbury District Health Board Facilities Development Project, which includes redevelopment at Burwood Hospital and the construction of the Acute Services Building at Christchurch Hospital, is the largest single investment in public health facilities ever made in New Zealand. The overall cost is expected to be about $650-700 million.
2.64
The Government established a Hospital Redevelopment Partnership Group, which includes representation from Canterbury DHB and the Ministry, and independent members to provide governance oversight of the project. The Ministry is taking a central role in management of the project. Previously, hospital building construction projects were managed and governed by DHBs.
2.65
When this role was given to the Ministry in 2013, it was a new role. The Ministry has had to build this capability and will need to continue to build capacity to reflect the additional projects it is delivering. We understand that the Ministry will soon hand over the completed Burwood Hospital to Canterbury DHB.
2.66
In our report Governance and accountability for three Christchurch rebuild projects, we examined the new governance model as it applied to the construction of the Acute Services Building. The project appeared to be progressing well, but significant risks were caused by a lack of clarity about roles and responsibilities in the new arrangements, which had been brought together hastily. We recommended that the Ministry ensure that lessons from this project and elsewhere in the public sector are applied to other projects using this model.
2.67
The construction of the new Grey Hospital for West Coast DHB currently under way and the planned Dunedin Hospital build for Southern DHB are also using this model. We will continue to monitor the governance arrangements for these projects and the Ministry's response to any recommendations arising from the review.
Asset management
2.68
DHBs rely heavily on physical assets, such as hospital buildings. DHBs have $5.7 billion invested in physical assets and plan more than $6 billion of capital expenditure in the next 10 years. During our audits in 2014/15, we noted that a number of DHBs had started or were planning major asset replacements. In at least one instance, the Dunedin Clinical Services Building belonging to Southern DHB, the replacement work was considered urgent because of difficulty maintaining the building at appropriate standards for delivering services. We also noted that some other DHBs were obliged to manage their accommodation needs carefully because they owned buildings that required earthquake strengthening.
2.69
The Ministry started requiring DHBs to prepare asset management plans in 2009. At that time, our auditors looked at how DHBs responded to the requirements. Since then, we have reported concern about whether DHBs have the asset management information they need to support the delivery of health services that depend on assets.
2.70
We decided to take a more in-depth look into the state of DHB assets and the approach that DHBs are taking to manage them. To inform our work, we analysed all DHBs' reported financial results and forecasts that were relevant to how they managed their assets. We also collected, as part of our 2013/14 audits, information about how DHBs manage two classes of assets: their buildings and clinical equipment. We also analysed information provided by the Ministry and the Treasury from recent initiatives to improve asset management.
2.71
Effective asset management begins with a good understanding of each DHB's population, current asset base, and future service needs – and a sound asset management plan to support future service delivery.
2.72
Among our findings were that:
- about two-thirds of DHBs have not substantively updated their asset management plans since 2009;
- DHBs tend not to specify the levels of service they expect from their assets and, as a result, reporting on asset performance is generally weak;
- DHBs generally do not systematically collect, maintain, analyse, and use asset information, particularly on clinical equipment; and
- there is limited reporting to governors and senior managers about the performance and condition of assets.
2.73
We also looked at capital expenditure management in DHBs, because of its connection with asset management. We found that:
- there has been sizable over-budgeting or under-spending of capital, suggesting that the DHBs might not be investing the capital needed to continue to deliver their services in the future; and
- almost half of all capital expenditure is funded externally rather than from DHBs' operating cash flows, indicating that DHBs rely heavily on funding from the Crown to renew and replace assets.
2.74
These results lead us to ask how well DHBs are positioned to support future service delivery and financial decision-making. Our audit results depict DHBs focused on delivering short-term results. In our view, the DHBs will need to take a longer-term perspective on health services and associated capital investment and asset management.
2.75
We expect DHBs to give more attention to their asset management, and a number of them have told us of their commitment to improving in this respect. DHB asset management practitioners told us about the part that they expect the Health Asset Management Improvement Group, formed in 2015, to play in this.
2.76
We also recommended that the Ministry and the Treasury provide support to help DHBs to improve, and consider how to provide incentives for DHBs to balance short-term results with longer-term service and asset management needs. We were told that complying with the 2015 Cabinet Office Circular on Investment Management and Asset Performance in the State Services is an important component of this. We will continue to monitor DHBs' asset management.
Our assessments of public entities' management control environment, systems, and controls
2.77
In annual audits, our auditors comment on the management control environment, financial information systems and controls, and performance information and associated systems and controls. We assign grades for each of these three aspects to reflect the scale of our recommendations for improvement. The grades are based on the accountability documents relating to the particular year. They are not an assessment of overall management performance, or of an entity's effectiveness in achieving its financial and service performance objectives. Figure 2 provides explanations for each grade we assign.
Figure 2
Grading scale for assessing public entities' environment, systems, and controls
| Grade | Explanation of grade |
|---|---|
| Very good | We have made no recommendations for improvement. |
| Good | We have recommended that some improvements be made. |
| Needs improvement | We have recommended that major improvements be made at the earliest reasonable opportunity. |
| Poor | We have recommended that fundamental improvements be made urgently. |
2.78
Overall, the grades assigned show that the health sector entities have generally maintained sound management and financial controls, and have improved their performance information and associated controls.
2.79
Figure 3 shows the spread of grades for DHBs against all three aspects in 2014/15.
Figure 3
Environment, systems, and controls grades for district health boards, 2014/15
| Grade | Management control environment | Financial information systems and controls | Performance information systems and controls |
|---|---|---|---|
| Very good | 2 | 0 | 1 |
| Good | 16 | 18 | 17 |
| Needs improvement | 2 | 2 | 2 |
| Poor | 0 | 0 | 0 |
2.80
We include the results of our assessments in our audit reporting to management and governing boards. We also report the results to the Minister, the Ministry (as the monitoring department), the three central agencies,8 and Parliament's Health Committee.
2.81
Grades for a particular entity can fluctuate from year to year depending on several factors, such as changes in the operating environment, applicable standards, good practice expectations, or the auditor's emphasis. For example, a downward shift in a grade might not show deterioration – the entity might have simply not kept pace with good practice in similar entities from one year to the next. How an entity responds to an auditor's recommendations for improvement is important, and the long-term trend in grade movement is a useful indication of general progress.
2.82
Appendix 2 sets out the grades for 2014/15 and the previous year for each DHB.
Grades for district health boards
2.83
In this section, we discuss the 2014/15 grades and five-year trends in grades for DHBs' management control environment, financial information systems and controls, and service performance systems and controls.
Management control environment
2.84
Figure 4 sets out the grades for the DHBs' management control environment for the last five years.
Figure 4
District health boards' management control environment grades, 2010/11 to 2014/15
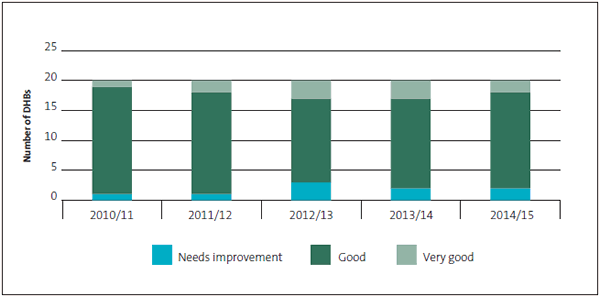
2.85
The grades for DHBs' management control environment show reasonably consistent results with small changes over the five years covered. The number of DHBs graded as "very good" has fallen from three to two in 2014/15, with a corresponding rise in the number graded as "good", from 15 to 16. Two DHBs were graded "needs improvement".
2.86
We changed the grade for Canterbury DHB from "very good" to "good" because we noted some improvements that should be made. They included revisiting the budget assumptions from the earthquake repair programme and facilities rebuild, and management reviewing and obtaining board approval for the capped inter-district flow agreement with West Coast DHB, which sets the cost that Canterbury DHB charges for clinical services provided to West Coast residents.
2.87
All other grades remained the same as in 2013/14.
2.88
The most common recommendations were for DHBs to improve their policies and processes for procurement and contract management, ensuring that they have adequate reporting frameworks for contracted providers of healthcare services. Recommendations also included reviewing and monitoring contracts to ensure reporting on quality as well as quantity; training staff in formal processes for procurement and contract management; and strengthening controls to mitigate risk of conflicts of interest, internal or with contracted parties.
Financial information systems and controls
2.89
Figure 5 sets out our grades for DHBs' financial information systems and controls for the last five years.
Figure 5
District health boards' financial information systems and controls grades, 2010/11 to 2014/15
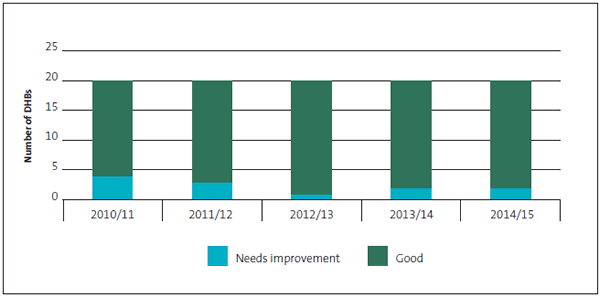
2.90
The grades for DHBs' financial information systems and controls have shown improvements since 2011, with the number of "needs improvement" grades falling from four to two. All the DHBs retained their grades from 2013/14 to 2014/15.
2.91
Two DHBs, Southern and Wairarapa, were rated as "needs improvement".
2.92
For Southern DHB, we noted serious weaknesses in the budget and forecasting processes. We also observed that the very long time it has taken to finalise budgets with the Ministers of Health and Finance contributes to these weaknesses. Its annual plan for 2014/15 was not signed by the end of 2014/15, and its 2015/16 annual plan was not signed until March 2016.
2.93
We recommended that Southern DHB make major improvements to its financial systems and controls as soon as reasonably possible.
2.94
We made other recommendations to DHBs for improving their financial systems and controls:
- we advised some DHBs in shared-services arrangements to consider additional reporting or assurances, to enable the board and management to maintain appropriate controls over expenditure and delivery of services.
- we recommended that some DHBs review their processes to ensure that provisions and accruals are accurately disclosed in the draft financial statements and that the amounts are in line with the supporting documents.
- we noted gaps in some DHBs' disaster recovery and business continuity planning and processes.
- We continued to note some basic IT issues with user-access controls in some DHBs.
2.95
We noted a particular risk for Wairarapa DHB, which has no support for its current financial management information system. Wairarapa DHB is expecting to move to a new system as part of NZHP's National Oracle System, but delays in completing that project has extended the period of risk substantially. We consider that other DHBs should take note, and ensure that they have measures in place to mitigate the risks should a similar transition situation arise.
Performance information and associated systems and controls
2.96
Figure 6 sets out our grades for DHBs' performance information and associated systems and controls for the last five years.
Figure 6
District health boards' performance information and associated systems and controls grades, 2010/11 to 2014/15
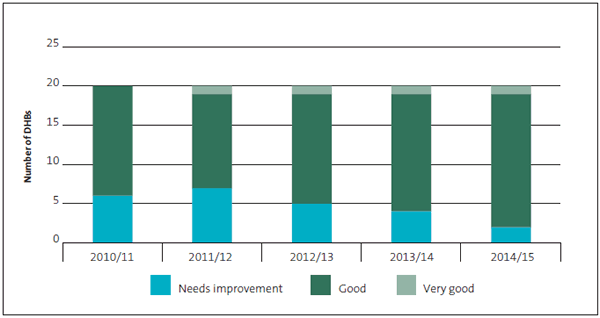
2.97
Our consideration of DHBs' performance information and associated systems and controls excluded the third-party performance information matter that resulted in a non-standard audit report for all DHBs. We excluded this from our consideration because it is a sector-wide matter, and we did not feel that any one DHB could make the improvements that are needed.
2.98
The third-party performance information matter aside, this is the most improved aspect of DHBs' control environment and information in the last five years. There was further improvement in 2014/15, with two more DHBs moving from "needs improvement" to "good". Wairarapa and Tairāwhiti DHBs remained at "needs improvement". For Wairarapa DHB, this was because of the lack of evidenced controls that we could rely on in auditing its performance information. In the case of Tairāwhiti DHB, we identified improvements that the DHB could make to the way it reports on outcomes, impacts, and outputs, so that readers of its annual report can gain a better understanding of its performance.
2.99
All the other DHBs retained the grading they received in 2013/14.
Grades for the Ministry and other Crown entities
2.100
The grades for the Ministry and the health sector Crown entities were all "good" or "very good" in 2014/15. This means that, in general, these entities maintained robust systems and controls during 2014/15, and that our auditors did not find any major concerns. For entities assessed as "good", we recommended improvements. We excluded the sector-wide issue about third-party performance information reporting from our grading of performance information and associated systems and controls when assessing the Ministry.
2.101
The grades for the Ministry, the New Zealand Blood Service, and the Health Promotion Agency were unchanged from the previous year. The New Zealand Blood Service maintained "very good" grades for all three aspects for the fourth consecutive year.
2.102
The Health Research Council moved from "very good" to "good" for its financial systems and controls because we assessed the new system the Council uses to manage research contracts, which went live in September 2014, as needing some additional processes.
Audit results for regulatory authorities
2.103
We audit the 16 regulatory authorities (see Appendix 1) whose members are appointed by the Minister under the Health Practitioners Competence Assurance Act 2003. We also audit two secretariats, which each support two or three of the authorities.
2.104
The regulatory authorities are responsible for the registration and oversight of health professions. Each authority prescribes scopes of practice and required qualifications for its profession, registers practitioners, and issues annual practising certificates. The authorities are funded by their professions through membership fees.
2.105
In our previous health sector report, for 2012/13, we discussed the lengthy period of uncertainty for the authorities as they considered a proposal to establish a shared secretariat organisation. We considered that both the prolonged uncertainty and any eventual transition created risks to the entities' control environments, which would need to be managed carefully.
2.106
We understand that the authorities have decided not to proceed with the shared secretariat option.
2.107
The three regulatory authorities with June or September balance dates began using the new PBE accounting standards in 2014/15. They were well prepared and the audits went smoothly as a result.
6: Health sector: Results of the 2012/13 audits, available at www.oag.govt.nz.
7: The External Reporting Board is an independent Crown entity responsible for developing and issuing accounting and auditing and assurance standards in New Zealand.
8: The three central agencies are the State Services Commission, the Treasury, and the Department of the Prime Minister and Cabinet.

