Part 7: Improving the capability of service providers
7.1
In this Part, we discuss:
- what service providers were funded to do;
- the system for funding service providers, how much funding they got, and examples of their costs;
- the information that Te Puni Kōkiri collects from service providers and researchers to assess results and what the early signs show;
- reports from the Ministry of Health and the Ministry of Social Development;
- each year's planned and actual spending; and
- what people told us about what the service providers were doing.
7.2
At the end of the Part, we make some observations.
About the service providers
7.3
For the Service Delivery Capability fund, the service providers involved were Māori and Pacific organisations that deliver community-based health and social services under contract to the Ministry of Health, and/or the Ministry of Social Development, and/or district health boards. Those services include, for example, smoking cessation, services delivered by general practitioners, immunisation, breast screening, road safety literacy, budgeting, advocacy for children and young people who witness family violence, and injury prevention. The service providers might also have contracts with other government agencies (such as the Ministry of Education, the Ministry of Justice, or the New Zealand Transport Agency) to deliver other services.
7.4
Groups of service providers (called provider collectives) were encouraged to enter into a formal relationship – such as an alliance or a joint venture – and jointly apply to Te Puni Kōkiri for funding so that they could provide whānau with easier access to a wide range of services and work together to deliver these services in a whānau-centred way. For simplicity, we use "provider collectives" to also include large single providers that already delivered a wide range of services and therefore did not need to form a collective.
What the provider collectives were funded to do
7.5
Provider collectives were funded to prepare and carry out project plans, called Programmes of Action. These take one, two, or three years to carry out. The Programmes of Action set out the specific actions, milestones, and costs involved in collectives moving to whānau-centred service delivery.
7.6
Every collective is different, which means that each Programme of Action's goals, actions, milestones, and measures of success are different. Nevertheless, Programmes of Action do have common elements because Te Puni Kōkiri required them. Figure 9 shows the core topics.
Figure 9
Core topics in Programmes of Action
| Topic | What he Programme of Action needed to discuss |
|---|---|
| Relationship management | How the provider collective would plan and work together, including communication protocols and how funding would flow. |
| Infrastructure | How the provider collective would deal with infrastructure needs to develop and implement a whānau ora approach, including privacy and information systems. |
| Integrated contracting | Whether high trust and integrated contracts would be helpful to them. |
| Workforce and practice development | How the provider collective would strengthen existing workforce capabilities and capacity, such as developing an effective and sustainable whānau-oriented workforce (such as lead practitioner or navigator positions) and using practice methods that are shaped by te ao Māori. |
| Monitoring and evaluation | How the provider collective would participate in the monitoring and evaluation programme led by Te Puni Kōkiri to assess progress against the Whānau Ora Outcomes Framework. |
| Action research plan | The processes that the provider collective would put in place to assist the research. |
Source: Te Puni Kōkiri.
Who decided which provider collectives to fund?
7.7
Officials in Te Puni Kōkiri's national office in Wellington managed the Service Delivery Capability fund. These officials put in place a system to select providers and collectives, and to fund them. Te Puni Kōkiri had help from the Ministry of Health and the Ministry of Social Development to design the funding system and to select and fund provider collectives. Te Puni Kōkiri adapted the system the Ministry of Health used for the Better Sooner More Convenient initiative.23
7.8
Te Puni Kōkiri's officials (at national office and in the regions) got advice and recommendations from the regional groups, the Governance Group, and officials from the Ministry of Health, district health boards, and the Ministry of Social Development to help make decisions. Te Puni Kōkiri put in place a method to promote consistent decision-making and fairness, and contracted a firm of chartered accountants to help with this.
The funding system for provider collectives
7.9
Provider collectives were funded to carry out their Programmes of Action by signing a contract with Te Puni Kōkiri called a Programme of Action Implementation Agreement.
7.10
To get to that point, provider collectives had to have:
- put in an Expression of Interest to Te Puni Kōkiri and had it accepted;
- signed an Engagement Agreement with Te Puni Kōkiri to prepare a Programme of Action;
- prepared and sent a Programme of Action to Te Puni Kōkiri and had it accepted;
- as needed, prepared and sent a business case to Te Puni Kōkiri and had it accepted;24 and
- as needed, prepared and sent an information services strategic plan to Te Puni Kōkiri and had it accepted.25
7.11
Provider collectives were funded to help them prepare all documents except for Expressions of Interest.
7.12
The joint agencies commented on each document, and provider collectives might have had to make changes before Te Puni Kōkiri accepted the documents. We were told that provider collectives were sometimes given conflicting comments from the joint agencies on what needed to change to get that agency's backing for a particular document.
7.13
The Governance Group preferred to fund one provider collective in each area within a region to prevent duplication. After the first batch of provider collectives had been selected, Te Puni Kōkiri identified those areas without a provider collective. Providers working in those areas were encouraged to put in an Expression of Interest and work towards signing a Programme of Action Implementation Agreement.
7.14
Although there are provider collectives in each Te Puni Kōkiri region, they are not in every area within a region. National coverage was not an objective of Whānau Ora.
How much were provider collectives paid at each stage?
7.15
We did not examine the amounts paid to each provider collective to build their capability. Figure 10 shows that:
- Engagement Agreements were signed in one year and most Programme of Action Implementation Agreements were signed in the next year;
- eight provider collectives were offered funding to prepare a Programme for Development;26
- the Initiatives eventually involved 32 provider collectives (made up of 163 providers);27 and
- the largest amount paid to a provider collective to implement a Programme of Action was about $5.3 million.
Figure 10
Programme of Action stages funded each year and the range of payments made to provider collectives for each stage, 2010/11 to 2013/14
| Programme of Action stages | 2010/11 | 2011/12 | 2012/13 | 2013/14 | Total | Amount paid (range) |
|---|---|---|---|---|---|---|
| Programme for Development | 1 | 5 | 2 | 0 | 8 | $15,000 to $70,000 |
| Engagement Agreements to prepare Programmes of Action/business cases | 25 | 7 | 2 | 0 | 34 | $107,125 to $445,520 |
| Short business cases | 22 | 4 | 1 | 2 | 29 | $50,000 to $150,000 |
| Programme of Action Implementation Agreements | 0 | 19 | 10 | 3 | 32 | $685,000 to $5,330,000 |
| Information services strategic plans | 10 | 2 | 2 | 0 | 14 | $40,000 to $70,000 |
Source: Te Puni Kōkiri.
Notes: If provider collectives wanted an advance on funding that they were likely to get when their Programme of Action Implementation Agreement was signed, they could put in a short business case for a specific action (such as training) for Te Puni Kōkiri's approval. On two occasions, a provider left a collective before a Programme of Action Implementation Agreement was signed. Te Puni Kōkiri negotiated new agreements with the remaining providers to carry out relevant parts of the Programme of Action. The data does not include these contracts.
What the provider collectives could get funding for
7.16
Providers had two sets of costs. First, there were costs in preparing, negotiating, and finalising the documents required by Te Puni Kōkiri. Secondly, after the Programme of Action Implementation Agreement was signed, there were costs in implementing the Programme of Action, which included working with researchers and reporting on progress to Te Puni Kōkiri.
7.17
Examples of the kinds of costs that provider collectives had include:
- directors' and trustees' fees to attend meetings;
- meeting costs, such as venue, catering, equipment hire, and travel;
- hiring new staff or contracting in specialist help, such as project managers, cultural advisors, lawyers, accountants, administration support, website developers, workforce development advisors, and business analysts;
- engaging with whānau to get a better understanding of their needs, such as completing baseline surveys or holding workshops attended by several generations;
- training and development on such topics as managing for outcomes, te ao Māori, and how to use whānau-centred assessment, planning, and monitoring tools;
- preparing a list of services available in a community, so providers could easily refer people to other services that could help them;
- introducing quality awards and scholarships for workers and whānau to recognise success;
- website and Facebook development to communicate with whānau;
- promotional material, branding, and marketing to encourage the community to contact and get involved with the provider; and
- attending national conferences and forums to discuss progress and share practices.
7.18
Funding also paid for a new workforce, commonly called navigators, who work intensively with whānau. Navigators were mostly funded through Programmes of Action.28
7.19
Te Puni Kōkiri prepared a set of expectations for navigators. Most navigators have three main roles:
- working with whānau to help them get more control over their lives, such as by helping whānau to identify their needs and prepare a whānau plan, and helping whānau use services effectively;
- if needed, helping whānau to get services that meet their needs; and
- helping the provider collective that they work for to change their mind-set and practices to deliver whānau-centred services, which might include proposing new services.
7.20
Te Puni Kōkiri expects each navigator to co-ordinate services to 15 or more whānau each year. Te Puni Kōkiri also expects that navigators can explain whānau development principles and understand tribal networks, Māori and/or Pacific culture, and community development principles. Navigators must know the services available in their area that whānau might want or need to use.
What provider collectives could not get funding for
7.21
Provider collectives could not get funding to pay for capital costs. For example, funding could not pay for information, communication, and technology infrastructure or systems (ICT). However, some provider collectives identified that their existing ICT was not suitable for bringing together information about whānau and documenting the services delivered to them. The Government decided to fund a Whānau Ora information system for provider collectives (see Part 8).
Examples of how provider collectives have changed how they work
7.22
The following two examples show the sort of positive changes that provider collectives have made.
Example 1
7.23
A woman had episodes of mental ill health for about 40 years. She had been hospitalised intermittently and relied on her children. Her state of health meant that she was not able to look after her grandchildren. The woman's experience was that mental health services were delivered reactively and did not support her to stay well. By the time she attended an appointment with a psychiatrist, she was fine because she had taken medication. The psychiatrist would say that there was nothing more they could do for her.
7.24
The last time she became mentally unwell, another relative referred her to a provider involved in Whānau Ora. The provider assigned a community worker to work with the woman and her family. The community worker met with the woman and her children together to assess the situation and discuss what the family wanted to achieve.
7.25
The community worker visited the mother weekly to provide support for more than a year. During this period, the woman felt supported and listened to, avoided hospitalisation, and met with a psychiatrist to review her medication. After twelve months, the woman felt better than she had for most of her adult life. She was no longer dependent on her children, had a part-time job, and her children trusted her to care for her grandchildren. The family were shortly to stop meeting with the community worker because there was no need to. The woman's son told her, "Mum, you're normal … and it's good."
Example 2
7.26
A man was referred to a provider participating in Whānau Ora by one of his children. At the time, he was an insulin-dependent diabetic who had suffered amputations. He was unable to support his own weight without aids and could not use a motor vehicle because it needed modifications. He had been admitted to hospital for rehabilitation but was having difficulty getting access to prosthetic limbs.
7.27
A navigator worked with the man and his children (and their partners and grandchildren) to:
- get him prosthetic legs and other aids, which involved advocating for him with the hospital, writing support letters, and applying for grants;
- get funding – from three sources – for vehicle modification, bathroom alterations, and house modifications;
- resolve delays in getting financial help he was entitled to, which resulted in an improved financial situation (including Family Tax Credits); and
- refer him to the rural nurse for help in managing his diabetes.
7.28
We have not listed other goals that were achieved. The approach the navigator took enabled family relationships to be strengthened in a range of ways, and the family achieved a greater level of self-management.
Information reported to Te Puni Kōkiri about provider collectives
7.29
Te Puni Kōkiri checks on the provider collectives' transformation and its effects on whānau through quarterly reports sent in by the collectives. The reports discuss the collectives' progress in describing changes to service design and transformation to whānau-centred service delivery and a "navigational approach".29 The collectives must also report on progress against the specific goals in their Programmes of Action, including those on workforce capability, governance and management, workforce development, and information technology infrastructure.
7.30
Collectives must also report on some standard measures, such as the number and proportion of whānau:
- with social, economic, and cultural goals achieved through whānau planning;
- reporting improved social, economic, and cultural outcomes;30
- with capacity goals achieved through whānau planning or another aspect of whānau-centred service delivery;
- reporting improved whānau connections;
- reporting improved knowledge and tools;
- getting whānau-centred service delivery;
- satisfied or very satisfied with whānau-centred service delivery; and
- satisfied or very satisfied with navigational support.
7.31
Other standard measures are:
- self-reported satisfaction of whānau engagement with the provider;
- the number of whānau working with navigators employed by the collective; and
- the number of active whānau plans that the provider collective is involved with.
How researchers help provider collectives
7.32
Te Puni Kōkiri contracted researchers to work with each provider collective to help them shift their service delivery approach from focusing on one person to focusing on the needs of whānau. Te Puni Kōkiri told us that an important part of the research was to instil in each provider collective the notion of building learning organisations and to give them methods to help with this. Te Puni Kōkiri told us that the purpose of collecting information through research was to check on the providers' capability building and its effect on whānau.
7.33
The research question was "How could agencies and providers most usefully contribute to the achievement of best outcomes for whānau?"
7.34
A research method was chosen that would give whānau an opportunity to discuss their experience of services and what their expectations of service delivery were. It also gave providers an opportunity to:
- consider whether what they were doing was effective;
- work out how they could share effective practices more widely; and
- become aware of challenges or barriers and how they could be dealt with.
7.35
The researchers' final reports are completed while the Programmes of Action are in progress (see Figure 12).
How research collectives were chosen and contracted
7.36
Interested researchers put in an Expression of Interest to Te Puni Kōkiri, which grouped the successful applicants into research collectives. Te Puni Kōkiri matched each research collective to a provider collective. Te Puni Kōkiri organised workshops to ensure that researchers could consistently use the chosen research method.
7.37
Researchers were employed in two stages. The first contract covered the first two phases of the research (which were relationship/engagement and planning). If the researchers' work was satisfactory, a second contract covered the last three phases of the research (which were data collection, action, and reflection).
Information Te Puni Kōkiri collects from researchers
7.38
Te Puni Kōkiri gets reports from the research collectives at certain milestones. Figure 11 shows the range of quantitative and qualitative data that researchers must report on, and the reason for collecting the data.
Figure 11
Researchers' reporting requirements
| Standard data needed | Reason |
|---|---|
| Document whānau and provider/collectives' experience of transformation and effects | Monitoring data:
|
Whānau input into provider transformation:
|
Evidence of:
|
Workforce development:
|
Evidence of:
|
Governance and infrastructure:
|
Evidence of:
|
Whānau planning and profiling:
|
Evidence of:
|
Navigational approach:
|
Evidence of:
|
Source: Te Puni Kōkiri.
7.39
The provider and research collectives report on some of the same topics in their reports. This means that Te Puni Kōkiri gets two perspectives on the progress of provider collectives.
When Te Puni Kōkiri will know whether providers have achieved their goals
7.40
Te Puni Kōkiri will be able to prepare a full report on Programmes of Actions' effectiveness when it has a full set of reports from provider and research collectives. Figure 12 shows when the final reports are due. It shows that the last research report is due by 31 March 2015 (the third quarter of 2014/15, Q3) and the last provider collective report is due by 30 June 2016 (the last quarter of 2015/16, Q4).
Figure 12
When researchers' and provider collectives' final reports are due, 2013/14 to 2015/16

Source: Te Puni Kōkiri.
Note: The Service Delivery Capability fund paid for services that were not part of Programmes of Action but were allied to the Initiatives, such as youth mental health and home-based rehabilitation. Te Puni Kōkiri got those reports by 31 July 2014, and they are included in the data.
What do the early signs show?
7.41
Early signs of the providers' transformation are promising, but there are issues. In our view, three reports published in 2013 reflect the general impression we got from the range of documents we read, which includes published information and Te Puni Kōkiri's regular reports to the Minister for Whānau Ora.
7.42
The first of the three reports summarised data from quarterly reports sent to Te Puni Kōkiri by 15 provider collectives between September 2012 and March 2013.31 It reported that improvements in provider capability have helped services become more whānau-centred and that providers can show they are more whānau-centred.
7.43
The report also says that whānau engagement and capacity is improving, by which it means:
- vulnerable whānau are engaged with providers where they were not before;
- relationships within whānau are improving through being engaged with providers;
- whānau who lacked these skills are learning to set goals and priorities;
- whānau are completing courses and training;
- whānau are resolving crises and reducing their needs; and
- most whānau are achieving aspirations and some are now self-managing.
7.44
The second report discussed research findings, which reinforced the provider collectives' reports and highlighted some difficulties.32 The researchers found that there was growing confidence in a collective approach and that navigators are an important driver of change for provider collectives, sectors, and regions. As a tool for change, whānau planning is helping whānau get a sense of control and priority in their lives. The providers' workforce is improving skills in engaging with whānau as well as individuals, in whānau planning, and in Results-Based Accountability.
7.45
However, the report said that there was a mismatch between the services that providers must deliver under their contracts with funders (such as the Ministry of Health, district health boards, the Ministry of Social Development, and others) and providing whānau-centred services. Providers needed to have the resources to do both. The report said that providers need more resources to respond to complex whānau needs, while delivering contracted services to individuals. For example, researchers' reports gave repeated examples of staff "working beyond the contract" and "being there 24/7".33
7.46
The report showed that provider collectives were starting to work together on contracts and regional priorities, which increasingly placed them in a strong position to respond to government priorities and initiatives to improve service delivery.
7.47
In 2013, Te Puni Kōkiri published a brief report on the results from the first set of user satisfaction surveys. The survey was of 51 whānau, representing 235 people. The report does not say how many provider collectives were involved or the period the survey covers. The surveys are run six-monthly, but trend reports have not yet been published.
7.48
The survey found that:
- 85% of respondents agree or strongly agree that whānau planning has brought their whānau closer together;
- 84% agree or strongly agree that they have more confidence in parenting and caregiving;
- 83% agree or strongly agree that they have improved confidence in tīkanga;
- 78% agree or strongly agree that, as a result of their work with provider collectives, their whānau has improved the amount or regularity of exercise they do;
- 77% agree or strongly agree that their whānau has an improved housing situation;
- 71% agree or strongly agree that their whānau has improved their income; and
- 54% agree or strongly agree that their whānau has a reduced rate of smoking.
7.49
In 2010/11, the service performance measures for the Service Delivery Capability fund mainly reported on progress with establishing provider collectives and approving Programmes of Action for implementation. Figure 13 shows the performance measures for the Service Delivery Capability fund from 2011/12.
Figure 13
Selected measures of service performance for the Service Delivery Capability fund, 2011/12 to 2013/14
| 2011/12 | 2012/13 | 2013/14 | |
|---|---|---|---|
| Number of provider collectives implementing organisational, information system, and workforce development changes to provide co-ordinated services to whānau | 26* | 34 | 34 |
| Number of whānau actively engaged by provider collectives in whānau ora services | At least 5000 | 5176 | 8916 |
| Number of whānau ora navigators co-ordinating services to at least 15 whānau | Not applicable this year | 138 FTE | 157 |
| Percentage of children supported to access or participate in early childhood education^ | 95.7% | 95.9% | |
| Percentage of children supported to access immunisation^ | 85% | 83.5% | |
| Percentage of engaged whānau that have taken steps to strengthen whānau connections (and cultural identity in 2013/14) | 89% | 72% | |
| Percentage of whānau actively engaged by provider collectives that have taken steps to improve education, employment, or housing outcomes | 71% | 59% |
Source: Vote Maori Affairs Report in relation to the Whānau Ora-based Service Development Multi-class output appropriations (non-departmental appropriations) for the years ended 30 June 2012, 2013, and 2014, www.treasury.govt.nz.
* The 2012/13 report said that there were 33 provider collectives in 2011/12.
^ Figure 3 shows that these measures replaced earlier measures on the same topic.
Reports from the Ministry of Health and the Ministry of Social Development
7.50
The Ministry of Health has introduced a series of three-monthly reports that compare results on 11 primary health indicators by some general practices that are part of a provider collective (the Whānau Ora sample) with other general practices' results (called the national sample).34 The Ministry of Health, Te Puni Kōkiri, and Tumu Whakarae (Māori managers within district health boards) picked these indicators because they are strongly associated with illness and death for Māori.
7.51
The reports show that providers in the Whānau Ora sample achieve better results for some indicators than the national sample. On other indicators, the national sample gets better results than the Whānau Ora sample. Nevertheless, the Ministry of Health considers that the Whānau Ora sample's results are encouraging because they have a higher proportion of high-needs patients (60%) than the national sample (26%). Even so, the Ministry of Health cautions that the results cannot be credited to any one programme or initiative.
7.52
The Ministry of Social Development has not published any reports on the effect that the Initiatives have had on the services it funds.
Each year's planned and actual spending
7.53
Figure 14 shows planned and actual spending for the Service Delivery Capability fund by financial year. In all four years, actual spending was less than the amount available.
7.54
In total, $67.9 million was spent through the Service Delivery Capability fund (which was 49% of total spending over the four years).
7.55
In 2010/11, the joint agencies took from July to October 2010 to select the first batch of provider collectives that would progress through the stages to achieve a Programme of Action Implementation Agreement. Consequently, $63,000 was transferred into the WIIE fund, and $9.9 million was transferred into two future financial years:
- $4.3 million moved from 2010/11 to 2011/12.
- $5.6 million moved from 2010/11 to 2012/13.
Figure 14
Service Delivery Capability fund: Planned and actual spending by financial year, 2010/11 to 2013/14
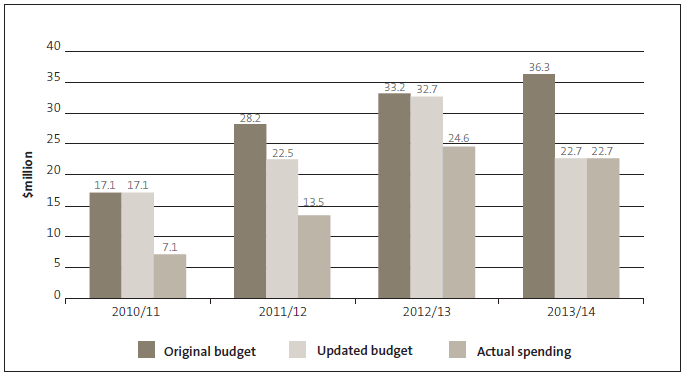
Source: Te Puni Kōkiri's annual reports, www.tpk.govt.nz.
7.56
In 2011/12 (the second year), there was a general election. Te Puni Kōkiri told us that it was not prudent to commit funding until the new Government was in place and the Initiatives were confirmed. This decision contributed to underspending, and subsequently almost $9.0 million was transferred into 2012/13. Budget 2011 included $10 million extra Service Delivery Capability funding, and this was also transferred, in two equal parts, from 2011/12 to 2012/13 and 2013/14.
7.57
Halfway through 2012/13 (the third year), the Minister for Whānau Ora launched a review of the Initiatives. Te Puni Kōkiri told us that it was not appropriate for it to make further funding commitments while the future direction of the Initiatives was unclear. This hiatus contributed to underspending. Consequently, $7.7 million was transferred to 2013/14, along with the $5 million that had earlier been transferred from 2011/12.
7.58
In 2013/14 (the fourth year), $10 million of the Main Estimates was transferred from Vote Māori Affairs to Vote Health for the Whānau Ora information system. In June 2013, Cabinet decided that any Service Delivery Capability funding that Te Puni Kōkiri did not have under contract by the end of December 2013 would be used to set up the commissioning agencies.
What people told us about provider collectives
Provider collectives
7.59
We got two perspectives on provider collectives from the people we spoke to. On the one hand, providers seem to be benefiting from working more closely together. Benefits include sharing effective practices and staff, co-operating to deliver contracts, and reducing duplication of services.
7.60
On the other hand, some people were not sure that provider collectives can consistently deliver whānau-centred services and get funded to deliver them, especially when funding to implement their Programmes of Action stops.
7.61
When we did our work, the Ministry of Health and the Ministry of Social Development told us that they had no plans to introduce new service specifications and contracts for whānau-centred services when the provider collectives can deliver them. Some people we spoke to hoped or speculated that the commissioning agencies might buy whānau-centred services from the collectives.
7.62
We heard concerns about whether provider collectives could afford to pay navigators when their Programme of Action is completed (and funding stops). Officials told us that funding for navigators was originally intended to be once-only funding so navigators could help the provider collectives put in place navigational approaches. However, the navigators became a fixed feature of service delivery. Budget 2014 committed an estimated $5 million a year for navigators from 2015/16 to 2017/18.
Provider participation
7.63
Officials from the joint agencies told us that they needed to move at the pace of the provider collectives and that this was the main reason affecting the pace of spending. The collectives needed time to work through each of the steps to achieve a Programme of Action Implementation Agreement when they were delivering business as usual, which might have included getting new service delivery contracts.
7.64
Officials told us that the joint agencies also needed to take time and put effort into agreeing funding arrangements. For example, the Expressions of Interest were considered in early July 2010, and the first batch of provider collectives entered into Engagement Agreements to prepare Programmes of Action in October 2010. It also took time to co-ordinate the activities of the government agencies, the Governance Group, regional groups, and the provider collectives.
7.65
A range of people we spoke to told us that provider collectives needed to establish high levels of trust to work together effectively. This took differing amounts of time depending on how well the providers in a collective knew each other and how similar their governance and management arrangements were.
7.66
Provider collectives also needed to have confidence in the joint agencies about the potential longevity of the Initiatives. About the same time the Initiatives were introduced, government agencies were mooting or piloting other methods of contracting for health and social services, such as social sector trials, investing in services for outcomes, and, later, social bonds.35
7.67
Some providers we spoke to had been concerned that taking part in the Initiatives could have adversely affected their involvement in these other government initiatives, which were being run by government agencies that regularly funded providers for service delivery. They were concerned that these other initiatives might have greater benefits for them and their clients, and a longer "shelf life". These providers had gone on to participate in the Initiatives, but we were told that other providers did not. The joint agencies gave us conflicting views on whether this was a valid concern.
7.68
Providers' experience of earlier capability schemes influenced their views of the Initiatives. They told us that they were wary of schemes closely linked with a particular Minister and/or Government because it was not uncommon for such schemes to be cancelled or significantly changed, sometimes before they had been fully implemented and properly evaluated.
7.69
We were told that some providers preferred to wait for the commissioning agencies to be set up before getting involved in the Initiatives.
7.70
Two providers' chief executives who we met with were part of collectives that did not achieve a Programme of Action Implementation Agreement. Both gave credit to the Initiatives for providing the impetus for them to put serious effort into working with other providers in their area, and for improving the way that they deliver services.
7.71
One of the chief executives told us that they considered that there were some advantages to not having a Programme of Action Implementation Agreement. For example, they could work with other organisation of different kinds (not only providers) at their own pace and embed changes before making more changes. They expect to achieve increased effectiveness and efficiency by sharing successful management and service delivery practices, and potentially staff. They considered that they were able to do this in a cost-effective way without extra funding. They were using funding available through existing and new contracts to reach out to people who are not engaged (or not effectively engaged) with services. This included working with organisations in their community, such as marae, providers, and businesses.
Our observations
7.72
Te Puni Kōkiri has not yet published a comprehensive report on what the Service Delivery Capability fund has achieved in the first four years. In 2015/16, Te Puni Kōkiri will get the last set of final reports from providers and research collectives.
7.73
Early signs are that providers are becoming more focused on whānau, and that providers and navigators are helping whānau take more control of their lives. However, there are issues. There is extra work involved in delivering services in a whānau-centred way, which providers are partly funded for through their Programmes of Action and through funding for navigators.
7.74
When we did our work, the Ministries of Health and Social Development had no plans to change to a funding model that would take advantage of the effort and $68 million paid to providers to help them shift to whānau-centred service delivery. The signals currently sent by different parts of government are, at best, mixed.
7.75
Providers have expressed similar concerns in their reports to Te Puni Kōkiri.
23. The Better Sooner More Convenient initiative is about ensuring that the right care is delivered in the right place, at the right time. Information about this initiative is available at www.health.govt.nz.
24. As the Initiatives progressed, provider collectives were able to combine the Programme of Action and business case into one document.
25 An information services strategic plan is a long-term plan (usually for three to five years) that describes how information technology resources will contribute to the organisation's strategic goals.
26. Programmes for Development were intended to enable provider collectives to reach the standard needed to get an Engagement Agreement.
27. A list of the provider collectives and their members is available at www.tpk.govt.nz.
28. Some navigators were funded through the WIIE fund.
29. That is, the provider collective working intensively with whānau in the way that a navigator would.
30. Te Puni Kōkiri told us that this is how it has summarised the taskforce's six outcomes goals for whānau (see Figure 1).
31. Te Puni Kōkiri (2013), Whānau Ora results September 2012 – March 2013, www.tpk.govt.nz.
32. Te Puni Kōkiri (June 2013), Whānau Ora action research (June 2013), www.whanauoraresearch.co.nz.
33. The taskforce's report had highlighted similar issues.
34. Ministry of Health, Report on the performance of general practices in Whānau Ora collectives, www.health.govt.nz.
35. Information about social sector trials and investing in services for outcomes is available at www.msd.govt.nz. Information about social bonds is available at www.health.govt.nz.

