Home-based support services for older people
1.1
In common with many other developed countries, New Zealand has an ageing population. Statistics New Zealand predicts that the number of people aged 65 and over will double between 2011 and 2036. This would mean that by the late 2030s, people aged 65 and over will be almost one-quarter of New Zealand’s population (see Figure 1).
Figure 1
Mid-range projections of the proportion of the population aged 65 and over, from 2011 to 2036
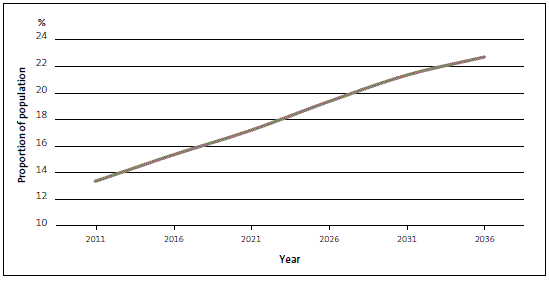
Source: Statistics New Zealand.
1.2
Statistics New Zealand says this increase in the numbers and percentage of people aged 65 and over will mean that there will be increased emphasis on older people being able to continue living in the community with some independence.
1.3
Older people, even those with considerable disability, generally prefer to live at home (which includes living in retirement villages) rather than in residential care. Staying at home lets an older person maintain their social networks and continue to be part of the community. Supporting older people to live independently at home can also bring wider financial benefits. Home-based support services usually cost less than caring for older people in rest homes or in hospital. Therefore, providing quality home-based support services that are effective and efficient is important for individuals and the economy.
1.4
In 2012/13, district health boards (DHBs) collectively spent about $263 million on home-based support services, funding an estimated 10.4 million hours of support for about 75,000 people aged 65 and over.
Background
1.5
In July 2011, we published a performance audit report entitled Home-based support services for older people. The report looked at how effectively the Ministry of Health (the Ministry) and DHBs ensured that older people get the care and support they needed to remain living independently at home.
1.6
Our performance audit examined:
- what the Ministry and DHBs had done to carry out the aspects of the New Zealand Health of Older Peoples’ Strategy that related to home-based care;
- DHB processes for providing older people with home-based support services, which included looking at InterRAI, the standardised tool used to assess and reassess older people’s support service needs;
- the delivery of home-based support services, which included looking at performance information from DHBs, providers, and the Ministry, as well as talking to several older people about the services they received; and
- how effectively the Ministry and DHBs monitor the quality of home-based support services and use this information to drive improvements.
| What is InterRAI? InterRAI is a comprehensive clinical assessment tool that helps staff to select appropriate support requirements for older people needing home-based support services. Staff can access it through the Internet when working in the community. InterRAI was introduced to DHBs from 2008 to 2012. InterRAI is designed to help staff assess an older person’s medical, rehabilitation, and support needs. The assessment is done in relation to a number of factors – for example, mobility and self-care. The Ministry believes that improving assessment outcomes for older people will enable them to stay in their own home for longer. InterRAI is also used in other parts of the health sector, and is currently being rolled out to aged residential care. The Ministry believes that this will improve needs-assessment of older people living in aged residential care. |
Source: IT Health Board and the Ministry of Health.
Our 2011 findings and recommendations
1.7
In 2011, we considered that, generally, the delivery of home-based support services was adequate. This was a qualified view because we concluded that the Ministry and DHBs needed to address deficiencies in performance information about home-based support services.
1.8
We found that there was no mandatory quality standard for providers of homebased support services. DHBs did not have a consistent and robust approach to managing quality. Therefore, we could not give positive assurance about the quality and consistency of services throughout the country. However, the limited information that was available did not point to widespread problems, and the small number of older people we interviewed told us that services were responsive and met their needs.
1.9
We made five recommendations for improvement. We recommended that the Ministry:
- collect and use reliable information to ensure ongoing service quality and value for money of home-based support services;
- evaluate by June 2013 whether using a standard approach to assessment and reassessment [InterRAI] is improving the way that older people’s needs are assessed and home-based support services are allocated; and
- consider making NZS 8158:2003 Home and Community Support Sector Standard (the Standard) mandatory for providers of home-based support services to older people.
1.10
We recommended that DHBs:
- work with others in the aged care sector to develop a complaints system that enables older people to feel confident about making complaints; and
- strengthen management contracts to ensure that home-based support staff provide high-quality services and are well trained and supervised.
1.11
These recommendations can be seen in full in our 2011 report.
Progress with achieving improvements
1.12
Overall, the Ministry and DHBs have made mixed progress with achieving improvements. The Ministry, with the assistance of DHBs, has made good progress in updating the Standard and making compliance with it a requirement in all provider contracts with DHBs. DHBs have also made good progress piloting a complaints process that seeks to standardise the way that providers record complaints. Some progress has been made in strengthening management contracts with providers to ensure that home-based support service staff are well trained and supervised.
1.13
However, there has been limited progress in other areas – evaluating the InterRAI assessment tool, and collecting and using reliable information to ensure ongoing service quality. The reasons for limited progress include problems in meeting deadlines as well as delays because the project to evaluate InterRAI has been re-scoped.
1.14
The rest of this article provides further information on the progress that the Ministry and DHBs have made.
Progress with introducing a minimum standard of home-based support services
1.15
The Ministry has made good progress with setting a minimum standard for homebased support services. In December 2011, the Ministry and other partners – for example, the Accident Compensation Corporation (ACC) and the New Zealand Home Health Association (NZHHA) – started a quality assurance programme. This quality assurance programme:
- set a minimum standard for home-based support services through DHBs contractually requiring providers to conform to the updated Standard;
- developed a voluntary self-assessment tool that providers could use to assess compliance with the Standard; and
- developed consistent processes and tools throughout the funders of homebased support services (DHBs, ACC, and the Ministry) for auditing compliance with the Standard.
1.16
In February 2011, Standards New Zealand started reviewing the Standard, as part of its ongoing review of the standards it administers. A revised Standard was published in April 2012. This revised Standard subsequently became a key component of the quality assurance framework.
| What is the Standard? The Standard sets out the minimum standard that home-based support service providers must achieve when delivering home-based support services to older New Zealanders. It is included in all DHB contracts with providers of home-based support services. |
| How do DHBs know whether providers comply with the Standard? The Director-General of Health appoints Designated Audit Agencies (DAAs) to carry out audits of healthcare services. One type of healthcare audit that some DAAs carry out is certification audits against the Standard. Providers that meet the Standard are issued certificates of conformance. Having independent audits should help provide assurance that certified home-based providers adhere to the Standard. Providers of home-based support services pay for these certification audits. |
Source: Ministry of Health.
1.17
The Ministry and DHB Shared Services see the 2012 Standard as a significant improvement on the previous one. The new Standard focuses more directly on client outcomes (instead of provider processes), and it takes into account clients’ varying and complex needs. The new Standard also promotes restorative care, a form of care that focuses on restoring some self-sufficiency to older people’s lives. The Standard has the support of people we talked to, including staff at the Ministry, DHB Shared Services, and the NZHHA. Staff at DHB Shared Services told us that DHBs and providers also support the new Standard. Having strong crosssector support should improve adoption of the Standard.
1.18
The Ministry ensured that stakeholders in the home-based support sector understood the implications of the Standard. The Ministry created guidance for providers and funders of home-based support services, which details how the new Standard differs from the old one, as well as highlighting challenges that funders or providers might face. The Ministry also participated in seminars across New Zealand, which were facilitated by the NZHHA. This should help to ensure a good understanding of the new Standard.
1.19
The quality assurance programme also produced a set of brochures for older people, which sought to improve awareness and understanding of home-based support services and the rights that they have as clients. One brochure encourages older people to make a complaint if something bad happens. It seeks to help older people identify the situations that could justify them making a complaint, and how they can go about addressing the situation or raising a complaint with their provider. DHB Shared Services told us that these brochures are a good first step in improving older people’s confidence to make a complaint.
Progress with introducing a complaints system
1.20
Through DHB Shared Services, DHBs have made steady progress with developing a complaints system that allows older people to confidently raise complaints. In October 2012, the quality assurance programme involving the Ministry and DHBs started work on creating a complaints categorisation process for home-based support services. That process aims to standardise how DHBs capture and record complaints.
1.21
In January 2013, DHB Shared Services began to prepare a pilot project on complaints categorisations. That pilot project is currently under way. In determining what a potential complaint could be, DHB Shared Services has linked categories of complaints to the ten consumers’ rights set out in the Code of Health and Disability Services (see Figure 2).
Figure 2
Categories of complaints linked to consumers’ rights
| Complaint categorisation for reporting to funder |
Consumers’ rights |
| Attitude | Right 1: Right to be Treated with Respect Right 3: Right to Dignity and Independence |
| Discrimination and Harm | Right 2: Right to Freedom from Discrimination, Coercion, Harassment, and Exploitation Service Delivery Right 4: Right to Services of an Appropriate Standard Communication Right 5: Right to Effective Communication Right 6: Right to be Fully Informed Right 7: Right to Make an Informed Choice and Give Informed Consent Right 9: Rights in Respect of Teaching or Research |
| Advocacy | Right 8: Right to Support Right 10: Right to Complain |
Source: DHB Shared Services.
1.22
The complaints process includes a template for reporting and addressing complaints. A likelihood and consequence matrix assigns a severity assessment code (SAC) to the incident complained of, to enable it to be prioritised and classified. Reporting requirements vary with the severity of the incident (see Figure 3).
Figure 3
Severity Assessment Coding and reporting process
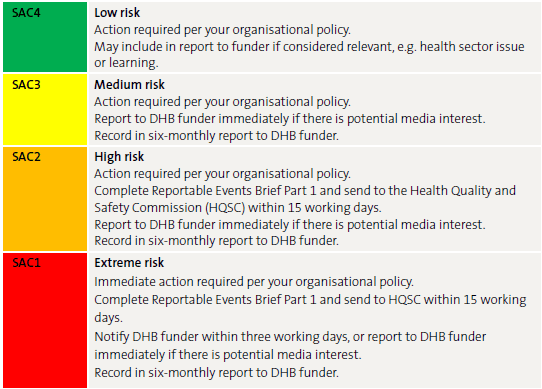
Source: DHB Shared Services.
1.23
The Auckland, Waikato, and Hutt Valley DHBs (and their service providers) are piloting the standardised complaints process. If the pilot project is successful, DHB Shared Services and the Ministry expect that all DHBs will be using the process by August 2014. In our view, having a standardised complaints process should improve accuracy in recording and reporting complaints and form a sound basis for improving how complaints are responded to and used to make improvements.
Progress with contracting for improved staff training and supervision
1.24
In our view, the Ministry and DHBs have made some progress in strengthening management contracts as a way of ensuring that service providers’ staff are adequately trained and supervised.
1.25
In June 2012, the Ministry drafted a service specification requiring provider staff to have a minimum level of training and supervision from clinical staff. However, DHBs and their providers were concerned about the unquantified costs of including the service specification in contracts. In October 2012, the Ministry decided to not include the service specification in contracts with providers until the cost to providers could be quantified. It is unclear when the service specification will be included in DHB contracts with providers.
1.26
However, the new Standard does provide some controls around ensuring that staff are adequately trained and supervised. Two audit reports of providers on their compliance with the Standard showed that contracted auditors were checking that there was training and supervision of staff at both providers. However there was some variance between both providers, as one provider had a timedependent component to their training, while the other did not.
Progress with collecting and using performance information
1.27
The Ministry has designed indicators to monitor service quality, but these are not yet being used as sufficient data from InterRAI is not yet available.
1.28
The Ministry drafted a set of relevant home support quality indicators in 2011 and tested them in 2012. The national home support quality indicators aimed to provide information on the levels and quality of assessments and home-based support services. Information collected through InterRAI will be used to inform the national home support quality indicators. There are about 100 indicators, measuring aspects that include:
- the number of new people who have been assessed using InterRAI;
- the cost of people receiving home-based support services; and
- the number of people who experience events or circumstances that affect their quality of life, such as the number of people who experience falls, and the number of people who have suffered weight loss.
1.29
The national home support quality indicators have not yet been implemented at a national level because sufficient useable data is not yet available from InterRAI to provide a national picture of service quality. DHBs implemented InterRAI at different times, but all DHBs have now been using InterRAI since June 2012.
1.30
However, the use of InterRAI is not consistent, as the proportion of older people receiving home-based support services in each DHB who have been assessed and reassessed using InterRAI is variable. An evaluation of InterRAI commissioned by the Ministry, which we discuss in paragraphs 1.32 to 1.36, found other issues that had also limited the use of InterRAI data.
1.31
The Ministry has plans to address consistency in the use of InterRAI and the quality of data, but no clear timetable has been outlined. When good quality data is obtained, this will support monitoring of service delivery and potentially lead to service improvements.
Progress with evaluation of InterRAI
1.32
The Ministry is part way through a staged approach to evaluate InterRAI. The Ministry has commissioned the evaluation to assess the extent to which using InterRAI has improved the way that needs are assessed and home-based support services are allocated.
1.33
The first stage of the evaluation was completed in December 2013 and examined:
- the extent to which the Ministry and DHBs have collated and/or used InterRAI data to inform ongoing service improvements and to identify and share good practice; and
- what needed to be done to enhance and support the use of aggregated data.
1.34
The evaluation found that analysis of InterRAI data was done at a regional level in some DHBs but there was limited use of InterRAI data at a national level. It concluded that the limited use was because there was no overall plan or strategy guiding and informing the use of data at DHB, regional, or national levels. The evaluation recommended that a more co-ordinated approach, guided by a strategy, would lead to more information sharing, and improve stakeholder engagement. It also recommended that consideration be given to establishing a centrally driven and resourced programme of regular reporting, as such a programme would help address DHB concerns of having limited resourcing and capability to undertake useful data analysis.
1.35
Stage two of the evaluation focused on identifying a framework and process for collecting and collating baseline data and information on the assessment for, and the allocation of, home-based support services. This stage of the evaluation has also been completed.
1.36
In the third and final stage of the evaluation, the Ministry is undertaking an evaluation of the governance arrangements for InterRAI. This has not yet been completed.
Further monitoring
1.37
We will continue to monitor the progress made by the Ministry and DHBs in making further improvements, particularly in the following areas:
- the Ministry and DHBs achieving national consistency in InterRAI data and the Ministry implementing its national home support quality indicators, so that accurate and reliable performance information is captured, analysed, and used to monitor service quality and make improvements where needed;
- the Ministry’s response to any recommendations resulting from its evaluation of InterRAI;
- piloting of the complaints system being completed and all DHBs using the final system to handle and respond to complaints; and
- implementing contractual arrangements by all DHBs to ensure that provider staff are adequately trained and supervised.

