Part 4: Putting case management into practice
4.1
In this Part, we set out our assessment of how effectively and efficiently ACC has put into practice claimant-focused rehabilitation services using case management.
4.2
If ACC has put claimant-focused rehabilitation services into practice effectively and efficiently, people will be supported with the appropriate treatment and rehabilitation services to return to work and/or independence as soon as is appropriate. The cost of those services and any associated weekly compensation will be reasonable in the circumstances.
Summary of our findings
4.3
ACC does not consistently deliver a claimant-focused service but elements of good practice underlie its services, such as using a claimant segmentation approach. Some claimants in the RIS stream have a more negative experience of ACC's services than other claimants. ACC could make changes to reduce the cost of case management.
4.4
ACC has used standard ways to make case management services accessible to eligible claimants. It has interpreters available, uses cultural advisors, has documents in many languages, and employs staff with a wide range of backgrounds. However, ACC needs to make its documents more accessible. It is working to achieve this.
4.5
ACC does not provide its documents in formats such as braille or large print for the visually impaired.
4.6
Day to day, case managers do not work directly with other agencies to actively manage each person's transfer between agencies.
4.7
ACC has high-level agreements with other government agencies to share information and funding.
4.8
ACC should continue to look for opportunities to make its case management services more cost-effective.
Accessibility of services
4.9
ACC has used standard ways to make case management services accessible. It has interpreters available, uses cultural advisors, has documents in many languages, and employs staff with a wide range of backgrounds. However, it needs to make its documents more readable.
4.10
ACC offers versions of its main documents, such as information sheets, in a range of languages, such as te reo Māori, English, Samoan, Tongan, Chinese, Korean, and Hindi, and has a process to ensure that these are translated appropriately. Telephone-based translation services are also available.
4.11
ACC does not provide its documents in formats such as braille or large print for the visually impaired.
4.12
ACC provides a deaf community fax facility and a dedicated email address for the hearing impaired.
4.13
A remote interpreting service is available to claimants with impaired hearing who have limited face-to-face access to New Zealand Sign Language interpreters. This service uses a web camera and video link to connect an offsite interpreter to a meeting between a case manager and a claimant. This service is available in the Whangarei, Whanganui, Gisborne, and Invercargill offices.
4.14
ACC has a website tailored to claimants with a disability caused by serious injury. It has information on the types of support available to these claimants and links to other useful information.
4.15
Access to health services is difficult in many rural areas. ACC told us that some temporary solutions are in place to make its services more available in rural areas. Examples provided to us were:
- Since 2010, providers of specialist clinical services have been able to invoice ACC for the time and cost of travelling to see ACC claimants in remote areas, such as Central Otago.
- ACC issued a contract variation in May 2014 that allows providers of vocational rehabilitation services to invoice ACC for travel (time and distance, above a certain threshold) to better support service delivery to people in remote areas.
4.16
ACC is aware that some of its documents are overly technical and not focused on the needs of claimants in terms of jargon, tone, and style. We note that ACC's Forms, Letters, and Information Sheets project is designed to significantly improve its forms, letters, and information sheets. This project uses guidelines (referred to as Tone of Voice guidelines by ACC) to improve ACC's documents.
4.17
We suggest that ACC continue to make its extensive set of standard letters, forms, and information sheets more readable. This includes ensuring that the documents, where appropriate, sufficiently explain the reasons for ACC's decisions.
4.18
We note that ACC's website does not comply with the Government's web standards (which are not mandatory) or the World Wide Web consortium's web accessibility initiative standards.
Good practice
4.19
International research has identified that, when put into practice effectively, case management can improve the experiences of users and carers, and support better care outcomes.
4.20
ACC's case management has features that some research has found support successful case management outcomes. 11 These include case managers:
- being accountable for an individual claimant;
- having access to specialist (internal and external) clinical expertise;
- focusing on one case management stream; and
- having access to information systems that support communication and data that can be used for quality improvement.
4.21
The international research identified other features that are important for successful case management outcomes, including appropriate caseloads and joined-up services. We comment on how well ACC follows these practices in paragraphs 3.46-3.56 and 4.61-4.66.
Delivering services inconsistently
4.22
People can expect different service experiences if services are organised around their individual needs and circumstances. However, the inconsistency we have observed and that ACC claimants have told us about appears to exceed the routine flexibility that might be expected in the use of case management.
4.23
Despite elements of good practice, ACC's case management practice is inconsistent in some respects. We observed, directly or indirectly:
- case management streams, locations, and teams focusing to different extents on the needs of claimants;
- inconsistencies in case managers' communication and engagement style and frequency;
- inconsistencies in how case managers use ACC's online procedural and policy guidance, and variations in decision-making;
- inconsistencies in using and checking Customer Engagement Appraisals; and
- opportunities to improve outcomes for longer-term claimants with complex needs who are not managed in the serious injury case management stream, and inconsistencies in the way this group was case managed.
4.24
ACC has also identified that different offices apply its medical assessment policy differently.
4.25
ACC claimants told us of inconsistencies in ACC's case management services. Colmar Brunton summarised these comments by saying that "Generally, the ACC case manager experience can best be described as inconsistent." Interviewees consider that the quality of service that case managers provide varies significantly depending on the case manager assigned to the claimant.
4.26
Case managers' different approaches to accessibility, empathy, and tailored communication have a significant influence on how people perceive ACC's case management.
4.27
These differing experiences, along with inconsistencies in the intensity of case management between case management streams, result in people having four broad types of reaction to ACC's case management practice. Figure 4 describes these different reactions.
Figure 4
How claimants feel about their case management experience
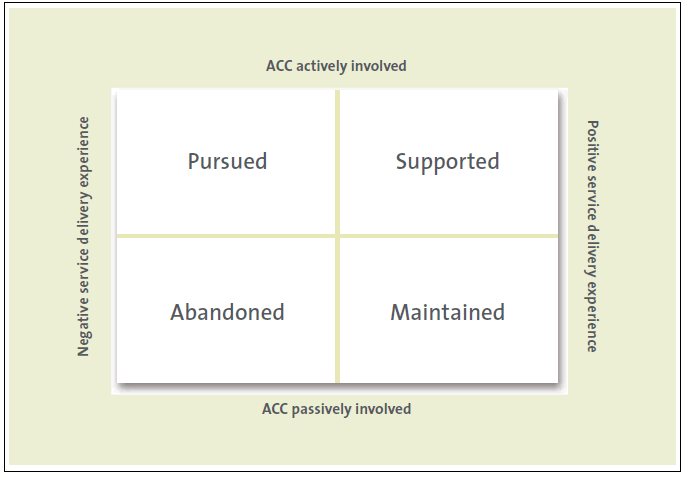
Source: Interviews with ACC claimants.
4.28
Figure 4 could be a useful tool for ACC to help inform effective communication and case management more generally between different claimants and case management streams.
4.29
Information from ACC quarterly case management survey results, research information that ACC commissioned, and ACC's complaints information shows that RIS claimants appear to feature disproportionately in complaints and report more negative experiences with ACC than others. The findings from the qualitative research that we commissioned are consistent with this evidence.
4.30
ACC can have a large and permanent effect on these claimants' lives – some have multiple and complex needs requiring long-time support from ACC. These claimants' claims are relatively expensive. There is a higher risk of damage to ACC's reputation if things go wrong. In our view, ACC should better understand how well it is delivering case management services to these claimants and make any improvements that are possible.
| Recommendation 3 We recommend that the Accident Compensation Corporation review the adequacy and appropriateness of its case management services for relatively long-term clients with complex needs who do not meet the serious injury criteria, and improve those services where necessary so that people receive the highest practical standard of service and fairness. |
4.31
Any review should look at how ACC communicates information about entitlements and obligations, how it communicates its understanding of people's individual circumstances, and how specialist assessments (both medical and vocational) are used. The specialist assessment process causes stress and anxiety for some long-term claimants.
4.32
At the time of our audit, ACC was reducing the number of days' threshold for becoming an RIS claimant.
4.33
In August 2014, when we were drafting this report, ACC told us that it had established a new senior management role of Strategy Manager, Serious Injury. ACC indicated that, along with work on serious injury, it expected that the strategy manager would investigate how ACC can better meet the needs of claimants with serious and/or complex injuries who do not meet the serious injury criteria, but who could benefit from additional case management expertise. This role appears to be in keeping with Recommendation 3.
4.34
During our audit, ACC changed its executive team structure. This included introducing the role of the Chief Customer Officer. This role is responsible for continuously improving customers' experiences of ACC.
Assessors' independence
4.35
ACC is taking a number of steps to reduce the risk of perceived or actual lack of independence in the assessment process.
4.36
ACC has recognised that there is potential for a perceived bias in the way it chooses medical providers for the assessment process. ACC's Medical Assessments External Reference Group has identified problems with the transparency of ACC's decision-making, the perceived lack of assessor independence, and the possible bias of choosing only assessors who deliver the results that ACC wants.
4.37
The ACC claimants we interviewed made suggestions about how ACC could improve the use, conduct, and explanation of specialist assessments. These include medical, rehabilitation, and vocational assessments used to inform judgements about whether claimants are capable of returning to work or to independence. Appendix 2 lists the improvements in ACC's assessments that claimants told us they wanted.
4.38
The assessments are professional judgements by people who are not ACC staff. Carrying out the assessments requires specialist skills, and the workforce available to carry out the assessments is limited. 12
4.39
The assessments inform judgements about whether people are capable of returning to work or to independence. Because assessments can have a significant effect on people's lives, they can be contentious. In the end, the judgements can determine whether a person will continue to receive weekly compensation from ACC. These assessments are particularly important to long-term claimants who might eventually return to independence.
4.40
It is not surprising that concerns have been raised about a lack of independence in the assessment process, because:
- assessments can have a critical effect on a person;
- a limited workforce is available to carry out the assessments, which suggests that some of the workforce receives significant income from ACC, and there is a risk that relying on that income affects their independence;
- ACC does not communicate well with some claimants about the purpose and conduct of the assessments (we saw a few examples of this in our file review);
- some claimants undergo repeated multiple assessments;13 and
- a return to independence for people can involve a significant reduction in income.
4.41
ACC has recognised that negative perceptions about the independence of assessors has significantly affected public trust and confidence in ACC. ACC's Medical Assessments External Reference Group has identified that "fairness is the key aspect of quality" in terms of assessments.
4.42
These concerns have resulted in ACC taking steps last year and this year to reduce the risk of perceived or actual lack of independence in the assessment process. These include:
- analysing the patterns of referral to specialist assessors;
- piloting a "panel" approach to assessments;14
- reviewing the quality of assessments and working with providers where necessary to improve the quality;
- researching claimants' perspectives;
- preparing guidelines for case managers to help with discussions with claimants about specialist assessments; and
- working with providers to understand how the number of providers willing to perform the assessment work could be increased.
4.43
In interviews with ACC staff, we were told that, in the past, the opportunity for people to choose an assessor might not have been explained clearly. We looked at ACC's operational policy about how much choice about assessor was offered to people. The policy was changed in late 2009 from giving people a list of assessment providers to choose from to requiring a person to use an assessment provider that ACC chooses.
4.44
If a person has a genuine and reasonable concern with the provider that ACC chooses, under the new policy, the person will be offered a choice of one or two alternative providers.
4.45
The new policy requires ACC to ensure that referrals are spread as evenly as possible to each provider. It also requires how referrals are distributed to providers to be monitored. We have seen examples of this monitoring.
4.46
The criteria that ACC uses to choose an assessor are the same that it uses to work out whether a person has a genuine and reasonable concern about the assessor that ACC chooses. The criteria are:
- the provider's competency;
- the provider's location;
- needs of the claimant;
- cultural considerations; and
- cost-effectiveness.
4.47
The 2009 policy does reduce choice, but it still gives claimants the right to object. Claimants also have the right to review. Giving claimants the right to object is one aspect of ensuring assessor independence. But ACC also needs to continue the steps (of the nature that we outlined in paragraph 4.42) that it is taking to reduce the risks of perceived or actual lack of independence in the assessment process. This is because assessor independence remains a topical issue, which can affect trust and confidence in ACC.
Managing expectations
4.48
ACC should do more to inform people earlier about cover, entitlements, potential treatment and rehabilitation pathways, and its expectations of people.
Initial written contact
4.49
ACC's first written contact with most people is an automated initial cover acceptance letter. ACC sends this letter after the person has received initial treatment for their injury from a provider of treatment services, such as a general practitioner, a physiotherapist, or an emergency department at a public hospital.
4.50
The version of the letter in use during our audit did not tell the claimant what injury ACC had paid to treat, who the treatment provider was, or what the next steps, if any, might be. In our view, leaving out this information is not good practice in terms of establishing a positive relationship and keeping people fully informed about which of their injuries ACC covers.
4.51
It is important that the letter is clear that, although ACC is confirming cover of an injury, it is not confirming entitlements for that injury – that is, the specific subsequent services and/or payments that a person can receive for that injury. It would also be helpful if the letter could give claimants some indication of what those entitlements might be. Without this information, the person is left with no guidance on whether they will have further contact with ACC, what ACC expects them to do, or what ACC might provide them with.
4.52
Omitting injury and treatment provider information could cause confusion when people have multiple injuries and/or multiple claims. For example, we reviewed some ACC files where people had more than 20 claims each.
4.53
Omitting injury and treatment provider information also could result in people expecting that ACC will automatically pay for further treatment and rehabilitation associated with an unspecified injury, when this might not be so.
4.54
The content of the letter has been the subject of much discussion within ACC. There are considerable practical, and potentially expensive, challenges in amending the letter to include accurate injury and provider information. Improvements to the tone of the letter have been recommended as a first step of ACC's Forms, Letters, and Information Sheets project, but there appears to be little enthusiasm for the more comprehensive system and business process changes that would be required to fundamentally improve the letter.
Support needs assessment
4.55
For some people, the next step will be a phone call from ACC to make an initial support needs assessment. The phone call's main purpose is to help ACC allocate the person to the appropriate case management stream. In our view, the information exchange is largely in one direction – from the person to ACC.
4.56
As part of the support needs assessment conversation, ACC tells the person that their claim will be allocated to a "case owner". The case owner will consider and confirm any entitlements, and will continue ACC's conversations with them. The person receives no indication of time frames for further communication from ACC, who the case owner might be, or the case management stream they are being assigned to. The lack of this information provides no certainty about any next steps.
4.57
We suggest that ACC consider using the support needs assessment to better inform people's expectations and obligations, as well as collect information.
Protecting and using information
4.58
We did not look in detail at privacy of personal information as part of our audit, but we did receive comments about privacy in our interviews with claimants. Appendix 2 lists the changes that claimants who we interviewed told us they wanted in how ACC manages personal information.
4.59
It was clear from our fieldwork that case managers are well aware of the importance of maintaining privacy. It was also clear that ACC's responses to its previous large-scale privacy breaches have been extensive and have affected day-to-day case management practice.
4.60
ACC intends that Shaping Our Future will help it to better protect and manage personal information.
Working with other agencies
4.61
Because of people's many needs and the potential for several agencies to be involved in supporting those needs, people might "fall between the cracks" if agencies do not work effectively with each other.
4.62
At an organisational level, ACC has agreed to collaborate with government agencies and interagency groups, including the Ministry of Social Development, Inland Revenue Department, Ministry of Health, and former Department of Labour (now part of the Ministry of Business, Innovation and Employment). The agreements with these organisations involve a mixture of sharing information and knowledge and funding.
4.63
These agreements can mean that some case managers take part in meetings with other agencies, but – day to day – case managers do not work directly with other agencies to actively manage each person's transfer between agencies.
4.64
Although case managers do not actively manage a claimant's transfer to another agency, some case managers help some of their claimants prepare to move from weekly compensation to a state-funded benefit, by providing support such as budgeting advice. Case managers refer people who are able to return to work to Work and Income and, with the person's consent, provide information on suitable work choices to Work and Income. There is a form for this purpose. It is not clear to us to what extent that form is used. We did not see this form used in any of the files we reviewed.
4.65
People who might transfer from ACC to the Ministry of Social Development include those who reach the eligible age for national superannuation. It also includes those who have been assessed as being vocationally independent, but who are unemployed at the end of their ACC entitlements. Between 5% and 15% of ACC's long-term claimants go on to receive a benefit from the Ministry of Social Development.
4.66
In our view, ACC should work more actively with other agencies, particularly the Ministry of Social Development, to manage the transfer of people between ACC and other public entities.
| Recommendation 4 We recommend that the Accident Compensation Corporation more actively manage the transfer of clients between it and other public entities to reduce the potential for people to miss out on services they are entitled to and to ensure that people are appropriately prepared for transfer to another public entity. |
4.67
There are clear expectations in the Accident Compensation Act 2001 about what happens if, for whatever reason, a person inappropriately receives a social security benefit and an ACC payment for the same period. Money paid inappropriately is to be recovered. In 2013/14, ACC had overpaid nearly $4 million that people were not able to repay immediately. This is a relatively small amount in terms of the $2.7 billion that ACC spends each year on treatment, rehabilitation, and compensation.
Case management costs
4.68
ACC tracks overall costs of handling claims as a percentage of total claims expenditure, and, more generally, the percentage of its total expenditure paid directly to claimants or for services to claimants.
4.69
ACC could make some changes to potentially reduce case management costs. ACC anticipates gains in claims-handling productivity and cost savings resulting from its Shaping Our Future change programme.
Direct case management costs
4.70
ACC reports that claims-handling costs were 12.5% of its total claims expenditure in 2012/13. This covers all claims, including those that ACC's short-term claims centres manage, which were outside the scope of our audit. This performance was against a forecast of 12.1% for 2012/13.
4.71
We have estimated, using information that ACC provided for the last week in June for each of the years from 2011/12 to 2013/14, that direct management costs for the claims that our audit covers are about 9%-11% of total expenditure on those claims.15
4.72
ACC provided information to us about the direct case management costs for the case management streams that our audit covers (see Figure 5). These costs range from $156.7 million in 2011/12 to $171.3 million in 2013/14 (excluding GST). Figure 5 shows a breakdown of these costs for case management streams for 2012/13.
Figure 5
Total annual direct case management costs, 2012/13
| Front-end | Recover Independence Service | Serious Injury Service | Total direct costs | |
|---|---|---|---|---|
| Salaries* | $96.8 million | $12.7 million | $10.9 million | $120.4 million |
| Claims network overheads | $38.3 million | $0.5 million | $0.7 million | $39.5 million |
| Total direct costs** | $135.1 million | $13.2 million | $11.6 million | $159.9 million |
* Salary costs include the cost of salaries and wages, employer superannuation contribution, annual leave, and sick leave.
** Excluding GST. Source: ACC.
4.73
As well as these direct costs, there are is a further $24.6 million in 2012/13 in salary costs of other staff supporting ACC's Claims Management Group, which includes case managers.
Cost savings
4.74
ACC anticipates gains in claims-handling productivity and cost savings resulting from Shaping Our Future: "The reduction in cost is driven by the need for fewer interactions with happier clients, fewer complaints, and a more engaged and productive workforce." Anticipated savings in terms of reduced weekly compensation costs through quicker return to work are also a factor.
4.75
To achieve the anticipated cost savings, ACC expects to make a large capital investment, mainly in information technology. This is reflected in a capital budget of $109 million for 2014/15 compared with capital expenditure in previous financial years of about $50 million or less a year.
4.76
Although ACC is not a provider of insurance16 and the ACC scheme is unique, the most obvious source of comparative cost information is other workers' compensation schemes and insurance companies, including those providing services related to accident insurance. Because of the commercial nature of insurance companies, the latter information is not readily available to us. The value of comparisons with other workers' compensation schemes is limited by differences in the funding and nature of each scheme.
4.77
However, we consider it important for ACC to continue to look at how much it costs to handle claims, including the costs of case management, against whatever comparative metrics are available and to keep looking for ways to be more efficient.
4.78
ACC gave us information from a consultant from 2010 that suggested that ACC's costs were satisfactory to good when compared with the comparative cost information available at that time.
4.79
However, ACC could improve some aspects that could reduce case management costs. These are:
- better integrating evidence in ACC's information systems;
- improving how it manages quality;
- having better performance information about case management streams (in particular the RIS stream); and
- reducing case managers' entering information manually and duplicating information.
11: Ross S, Curry N, and Goodwin N (2011), Case management – What it is and how it can best be implemented, The King's Fund, page 1.
12: The main assessments that ACC buys are initial medical assessments (which work out whether a client is fit for work or not), vocational independence medical assessments (which work out whether a client can work for 30 or more hours a week in jobs identified as suitable), and medical case reviews (which are one-off assessments used to work out cover, entitlement, or incapacity).
13: We saw a few examples of these in our file reviews. For example, in one of the complex files we reviewed, a client had a workplace assessment, an initial occupational assessment, an initial medical assessment, a specialist medical assessment, another initial medical assessment, a functional capacity evaluation, a vocational independence occupational assessment, an assessment by an orthopaedic surgeon, and a further planned initial medical assessment.
14: The panels are expected to improve transparency of the assessment processes and raise confidence in the assessments. The success of the pilot project had not been evaluated at the time of our audit.
15: ACC has defined direct case management costs as including salaries and wages, employer superannuation contribution, annual leave, sick leave, and specified overhead costs.
16: See section 262 of the Accident Compensation Act 2001.

