Part 1: Introduction
1.1
In this Part, we describe:
- why we carried out our audit;
- what home-based support services are;
- the roles of the Ministry of Health and district health boards;
- our previous audit on residential care;
- how we carried out our audit;
- what we did not audit; and
- the structure of this report.
Why we carried out our audit
1.2
We carried out a performance audit to establish how effective the Ministry of Health (the Ministry) and district health boards (DHBs) are in ensuring that, where appropriate, people aged 65 and over (older people) get the care and support they need to remain living independently at home.
1.3
Older people prefer to live at home for as long as possible because doing so improves their quality of life. It is also better for taxpayers that older people live at home for as long as possible, because home-based support services are much less expensive than residential or hospital care.
1.4
In 2009/10, DHBs collectively spent about $224 million on home-based support services, funding an estimated 9.2 million hours of support for about 75,000 older people. DHBs' forecasts indicate that, in 2010/11, they will collectively spend about $232 million on home-based support services.
1.5
We wanted to know whether the current processes used to manage and deliver home-based support services ensure that services are available to those who need them, are of an appropriate quality, and are able to meet current and future demand. Most users of home-based support services are aged over 75, and in the next 20 years New Zealand is expecting marked increases in the number of people aged 75 and over (see Figure 1).
Figure 1
Mid-range projections of the number of people aged 75 and over, from 2011 to 2036
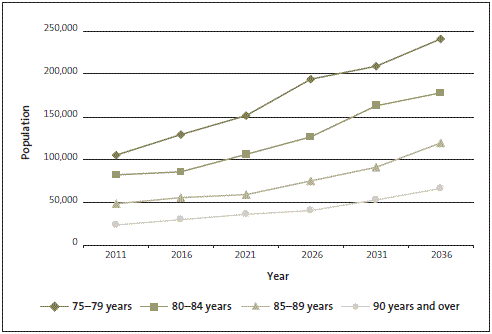
Source: Department of Statistics.
1.6
Home-based support services are not formally regulated, and any self-regulation occurs through a voluntary code of practice. We wanted to know whether this approach limits DHBs' ability to regulate services and ensure that high-quality services are delivered equitably throughout the country and are integrated with other health services.
1.7
Given the ageing population and the current economic climate, we also wanted to know whether the Ministry and DHBs were using performance information to identify risks to future service delivery and plan to mitigate them.
About home-based support services
1.8
In this report, we use the term "home-based support services" specifically to mean services funded by DHBs and provided to older people so that those older people can live more independently and avoid or postpone living in residential care (rest homes and hospitals).
1.9
People of any age can receive home-based support services for a short term as part of the post-operative support provided by their DHB. This sort of support is outside the scope of our audit (see paragraph 1.29).
1.10
Most older people are fit and healthy. However, the likelihood of becoming disabled in some way increases with age. Around 36% of all people aged 75 and over have a moderate disability (requiring some assistance or special equipment, but not daily assistance) and 18% have a severe disability (requiring daily assistance).
1.11
Most people aged between 65 and 74 years (74%) live at home without any assistance. However, the proportion of people needing assistance increases with age. Most older people receiving home-based support services are older than 75 years. Around half the population aged 85 years and over live at home with assistance, and 28% live in residential care. Other older people do not require any help to live independently at home, are supported informally by family and friends, or pay for support services privately.
1.12
Older people, even those with considerable disability, generally prefer to live at home (this includes living in retirement villages) rather than in residential care. Staying at home lets an older person maintain their social networks and continue to be part of the community.
1.13
As well as these social advantages for older people, there are clear financial advantages for DHBs in providing support to people who cannot receive the care they need from their friends and family. Effective home-based support services can delay or avoid a person's admission to a rest home. The average annual government subsidy for a person in a rest home is about $37,000. In contrast, the needs of someone living at home are often much lower, and the average annual cost to DHBs for a person receiving home-based support services is about $3,000.
1.14
The types of home-based support services provided to an older person depend on that person's needs. People assessed as having "low-level" needs can get help with household tasks, such as housecleaning, preparing meals, shopping, and laundry.
1.15
Some older people require more intensive personal care services, such as help with dressing, toileting, and bathing. These are described as "medium-level" needs. Other older people are assessed as having "complex" or "high" needs, which usually means that the older person has several health, functional, and/or social problems. The needs of older people with complex needs are comprehensively assessed and an ongoing treatment, rehabilitation, and care plan is developed with the older person. This care plan can include various services, such as occupational therapy, physiotherapy, support for informal carers (including respite care), care provided at a centre for older people, socialisation services, and rehabilitation.
Roles of the Ministry of Health and district health boards
1.16
The Ministry is the principal advisor to the Government on health and disability matters, and is responsible for leading and supporting the health and disability sector.
1.17
The Ministry published the New Zealand Health of Older People Strategy (the Strategy) in 2002. The primary aim of the Strategy is to develop an integrated approach to health and disability support services that responds to older people's varied and changing needs.
1.18
One of the objectives of the Strategy relating to home-based support services is that people with high and complex health and disability support needs will have equitable access to flexible, timely, and co-ordinated services and living options that take account of the needs of family and whānau carers. This includes developing a comprehensive range of service options and accommodation to enable older people with long-term health and support needs to live at home for as long as possible.
1.19
The Strategy provides guidance and sets the delivery of services for older people in context. The Ministry's work programme has focused on developing home-based support services for older people.
1.20
The Operational Policy Framework also sets out requirements for home-based support services. The Operational Policy Framework is a set of business rules, policy, and principles issued annually by the Ministry, which describes the operating functions of DHBs (and sets out their accountability requirements). When DHBs sign their Crown Funding Agreement (which provides funding for DHBs in exchange for DHBs providing the services specified in the agreement), they are effectively agreeing to the Operational Policy Framework.
1.21
The Ministry's Operational Policy Framework does not prescribe how DHBs should determine access thresholds for allocating services, how they are to prioritise the services, or at what level these services should be provided. DHBs decide these matters according to their financial resources, the needs of their population, their strategic priorities, and service availability. However, there is an expectation in the Strategy that access to services will be equitable – that is, that older people with similar needs will receive similar services, regardless of where they live.
1.22
DHBs use contract specifications to describe and define the services that they will fund and that providers must deliver. These specifications set out service aims, identify the eligible service users and how services are accessed, describe what the service components are, and set out the quality and reporting requirements.
Our previous audit
1.23
This audit follows on from our performance audit of the effectiveness of the arrangements to check the standards of services provided by rest homes. That audit examined the monitoring of residential facilities that care for older people who are no longer able to live independently at home.
1.24
We reported our findings on rest home monitoring in December 2009.1 Overall, we found that the certification of rest homes (introduced in October 2002) had not provided adequate assurance that rest homes were meeting criteria in the published Standards that applied to rest home care. Also, the Ministry had not responded quickly enough to address weaknesses and risks in the arrangements that it had known about since 2004.
How we carried out our audit
1.25
We reviewed what the Ministry and DHBs had done to implement the aspects of the Strategy that were relevant to home-based support services. We recognise that the Strategy was published in 2002 and that priorities can change over time. However, the Strategy provided the main framework for the delivery of home-based services, so we concentrated on DHBs' progress towards implementing it.
1.26
We also examined DHBs' processes for providing older people with home-based support services. We included the processes currently used and implementation of standardised needs assessment through the use of a single nationwide tool (InterRAI, discussed in Part 3). We surveyed all 20 DHBs and discussed the effectiveness of the assessment process with the Ministry and other stakeholders. We analysed audit and service review information from DHBs and information from the Ministry, and looked at a sample of 100 files from three DHBs about older people who receive home-based support services. We also reviewed printed and electronic information provided by DHBs about home-based support services.
1.27
To assess the delivery of home-based support services, we analysed information from our survey of DHBs and carried out fieldwork at five DHBs. We looked at performance information from providers, DHBs, and the Ministry. We reviewed documents and reports from the Ministry and DHBs. We discussed service delivery with other stakeholders and assessed the quality and consistency of contract arrangements between DHBs and providers. We also talked to several older people about their experiences of home-based support services. Their stories appear as case studies throughout this report.
1.28
To assess how effectively the Ministry and DHBs monitor the quality of services and use this information to drive improvements, we reviewed audit information made available by DHBs' shared service agencies.2 We also analysed data provided by the Ministry and DHBs, including the number and types of complaints made by older people about home-based support services.
What we did not audit
1.29
We did not audit any health and support services for people younger than 65 years, or health and support services for older people other than home-based support services. We also did not look at any related services funded by DHBs, such as services provided to support an older person's carer or low-level post-operative care.
Structure of this report
1.30
In Part 2, we examine:
- how well the Strategy has guided the delivery of home-based support services since it was published in 2002;
- what overall progress has been made under the Strategy; and
- some of the challenges the Ministry and DHBs face in continuing to manage and support the delivery of home-based support services.
1.31
In Part 3, we examine how well older people are able to access home-based support services. We look at whether:
- information on services is accessible;
- assessments of need are effective and consistent; and
- assessments and reassessments of need are timely.
1.32
In Part 4, we examine whether the quality of home-based support services supports the needs of the older population. We look at whether:
- the Ministry and DHBs have adequately specified the quality of services;
- services are of the required quality; and
- the Ministry and DHBs are adequately monitoring the quality of services.
1.33
In Part 5, we examine how well the Ministry and DHBs are managing the risks to the quality of services by:
- collecting and using performance information; and
- working with providers to manage the risks to service delivery.
1: Effectiveness of arrangements to check the standard of services provided by rest homes.
2: Shared service agencies are owned by groups of DHBs to carry out work that all DHBs require (including audits to check whether service providers are meeting their contractual obligations).
page top
