Part 2: Background
2.1
In this Part we discuss:
- what diabetes is;
- who it affects;
- what its effects are;
- the costs of diabetes;
- the health sector’s response to diabetes; and
- the “Get Checked” programme.
What is diabetes?
2.2
Normally the amount of glucose (or sugar) in the blood stream is controlled by
a hormone1 called insulin,2 which is made by the pancreas.3 Insulin controls the
amount of glucose in the blood by enabling the cells in the body to take glucose
from the blood and use it for energy.
2.3
People with diabetes have more glucose in their blood than normal because:
- The pancreas is not producing any or enough insulin (referred to as type 1 diabetes). Type 1 diabetes more commonly starts in children and younger adults, but it can occur at any age.
- The body produces insulin, but stops responding to it (referred to as type 2 diabetes).
Who does diabetes affect?
2.4
Diabetes is a common condition that potentially affects all New Zealanders.4 The
effect of diabetes on illness and mortality is significant, and will become more so
as the prevalence increases. Forecasts by the Ministry estimate that the number of
people diagnosed with diabetes will be 145,000 by 2011 (a 180% increase on the
numbers in 1996).5
2.5
In 2005, an estimated 125,000 people had diagnosed diabetes. About 85% to
90% of these had type 2 diabetes. Potentially, an equal number of people have
undiagnosed diabetes. Insulin-making capacity falls steadily with age, so diabetes prevalence increases with age. Up to one in six of those aged over 60 years has
diagnosed diabetes.
2.6
Some population groups, including Māori and Pacific Island peoples, are more
predisposed to diabetes and its complications. The 2002/03 National Health
Survey6 of people over 15 years of age suggests a prevalence of diagnosed
diabetes of:
- 3.4% for males and 2.4% for females of European or other origin;
- 9.5% for males and 6.7% for females among Māori; and
- 8.1% for males and 11.9% for females among Pacific Island peoples.
2.7
The risk of developing type 2 diabetes increases with a number of factors. These
include:
- being overweight;
- lack of physical activity; and
- having a family/whānau history of diabetes.
The effects of diabetes
2.8
In New Zealand, diabetes is a leading cause of blindness, kidney failure, and
complications leading to lower extremity amputation. It is also a major risk
factor for nerve damage (leading to problems with, for example, a person’s feet,
bowel, bladder, and digestion), stroke, heart attack, heart failure, and early death. Diabetes is a leading cause of congenital abnormalities, stillbirth, and miscarriage. It is also a major cause of admission to hospital with infections. (Refer to Appendix
1 for some of the complications that people with diabetes are predisposed to.)
2.9
The damage caused by diabetes is directly related to glucose, lipid,7 and blood
pressure control. Good diabetes care reduces the rate of complications and the
high cost of hospitalisation. It was reported in 1997 in Strategies for the Prevention
and Control of Diabetes in New Zealand (the 1997 Diabetes Strategy) that “Access
to good diabetes care is poor and inequitable”.8
The costs of diabetes
2.10
The 1997 Diabetes Strategy noted that there was only limited information on the
costs of diabetes. It said that people who had diabetes bore a major part of the
costs of diabetes, and this had not been calculated. There were also significant
indirect costs, both to the individual and to society. In 1997, the only elements of direct costs that could be estimated were the inpatient costs (estimated at $95
million per year) and some prescription costs (estimated at $29 million per year).
2.11
In 2000, Diabetes New Zealand9 commissioned PricewaterhouseCoopers to
develop an economic model to predict the costs of diabetes. The model predicted
that:
- the services provided for diabetes would cost the taxpayers $247 million for 2001/02; and
- the estimated costs, if services were maintained at the 2001/02 level, would be more than a billion dollars each year by 2021.
2.12
This increase was based on the projected increase in the numbers of people
developing conditions requiring hospitalisation, such as blindness, kidney failure,
or complications that lead to limb amputation.
2.13
A study reported in December 200610 looked at the cost of preventable kidney
failure and assessed the cost to be $90 million each year. The study noted that the
data in the “Get Checked” programme could provide a powerful mechanism for
preventing or delaying chronic kidney disease.
2.14
However, there is still a lack of actual information in New Zealand on the current
costs of diabetes.
The health sector’s response to diabetes
2.15
In 2000, the Ministry identified reducing the incidence and the effect of diabetes
as one of the 13 immediate action priorities for population health.11
2.16
The strategic direction for diabetes management set out by the Ministry of
Health in the 1997 Diabetes Strategy advocated a disease management approach
to diabetes care. The aims of the 1997 Diabetes Strategy were to improve coordination
and information flows among stakeholders in diabetes care, and to
improve diabetes services by integrating primary, secondary, and allied health
services. There were four focus areas:
- preventing type 2 diabetes;
- identifying people with diabetes and enrolling them into structured programmes in primary care;
- monitoring people with diabetes through free annual health checks, and using this information for quality improvement and service planning; and
- planning treatment throughout the range of services available.
2.17
The Health Funding Authority’s Diabetes 2000 implementation plan gave effect to
this. Diabetes 2000 notes that:
There are measures that predict the “severity” or future impact of diabetes and its complications. These include blood HbA1c, blood lipids, and blood pressure. 12
2.18
Diabetes 2000 then went on to note that, although some primary care
organisations (in place before PHOs were set up) collected this data for their
enrolled populations, it was not generally available for benchmarking or
identifying trends. Three initiatives put in place under Diabetes 2000 were aimed
at addressing this problem.
2.19
First, Diabetes 2000 supported the development of regional diabetes registers. It identified primary care organisations (now PHOs) as the appropriate place for
the registers to be located, because their general practitioners (GPs) generally
provided the initial diagnosis and treatment for almost all people with type 2
diabetes and its complications.
2.20
Secondly, one LDT was to be set up in each Regional Health Authority (now DHBs)
throughout New Zealand to reflect the needs of each region. The teams were to
include clinicians and consumers, and they were to be responsible for identifying
the needs of the region, monitoring the use of resources, and recommending any
improvements that needed to be made. The teams were to focus on the needs of
rural communities, Māori, and Pacific Island peoples.
2.21
Thirdly, a free annual review was to be provided for each person diagnosed with
diabetes. This initiative became the “Get Checked” programme. The intended
benefits of the free annual review were:
- Patients diagnosed with diabetes could be systematically screened, to detect and treat complications at an early or preventable stage.
- It provided an opportunity to review and update the patient’s treatment and management plan.
- The diabetes registers could be updated with a nationally consistent dataset of core information on each patient, which would then be used as a basis of clinical audit and for planning improvements to diabetes services. The results of this information were to be presented to the LDTs and reported by the LDTs to DHBs.
- Patients could be prescribed new treatment, and referred for specialist or other care if appropriate.
2.22
In addition, increased funding was put into education and management services
to try and make them nationally equitable, more eye screening was to be done,
and primary prevention and screening of certain patients for diabetes was to be
further investigated.
The “Get Checked” programme
2.23
The programme was launched in June 2000 at the beginning of a time of
significant change in the health sector. For example, DHBs were established on
1 January 2001, and the Primary Health Care Strategy released in February 2001
resulted in the establishment of the current 81 PHOs between mid-2002 and
April 2006.
2.24
The programme entitles people who have been diagnosed with type 1 or type 2
diabetes to a free annual health check, carried out by their GP or an appropriately
trained registered primary healthcare nurse (diabetes nurse). The purpose
of the check is to ensure that key tests (which assist in identifying diabetes
complications early) have been completed for the year and to plan treatment for
the year ahead.
2.25
Under the terms of the Tier 3 Free Annual Review for People with Diabetes Service
Specification13 (the annual check service specification), the GP or diabetes nurse
carrying out the annual check must:
- provide information about the service to the person with diabetes and receive consent from that person14 to forward identifiable clinical information to the programme administrator for the purpose set out in the service specification;
- review symptoms and concerns raised by the person with diabetes or their family/whānau;
- examine for risk factors and complications, including:
- a check of smoking status;
- an eye check, ensuring that retinopathy screening has been done;15
- a blood pressure check;
- a foot examination (according to clinical guidelines) and advice about basic foot care;
- a fasting blood test for total cholesterol and HDL;16
- a fasting blood test for triglycerides;
- a blood test for HbA1c;
- a urine test for early nephropathy,17 as indicated in clinical guidelines; and
- a review of medication and management, including prescriptions for medication, glucose test strips, and glucose monitors as required.
2.26
It is not intended that all tests and examinations be carried out at the time of the
free annual check. Rather, the annual check is to ensure that the indicated tests
and examinations have been done within the time frames indicated in clinical
guidelines, and to arrange for any outstanding tests to be completed.
2.27
Data obtained as a result of the annual check must be entered into the diabetes
register. The minimum data to be recorded – known as the minimum dataset – is
set out in Appendix 2.
2.28
The Ministry reported that 70,456 people (56% of an estimated 125,000 eligible
people) had participated in the programme during the year ended 31 December
2005.
Why have annual checks?
2.29
An important goal of diabetes treatment is to prevent complications. Over time,
higher than normal blood glucose levels will damage the heart, blood vessels,
eyes, kidneys, and nerves. However, the person may not know that the damage is
taking place.
2.30
Diabetes 2000 notes that:
Diabetes is a direct cause of symptoms, but the significant burden of the disease (and the majority of costs) relates to the development of complications that typically lead to hospitalisation or death.18
2.31
The free annual check aims to ensure that regular tests are carried out to identify
and treat complications at an early stage, and to agree individual treatment
plans for patients. The types of complications being tested for and the types of
treatment are set out in Appendix 1.
What happens to the information collected?
2.32
The Tier 3 Local Diabetes Team National Service Specification (LDT service
specification) sets out the required information flows:
- First, a GP or diabetes nurse carries out the free annual check. They review the patient’s treatment against guidelines, carry out any outstanding checks, agree a treatment plan for the next year, and refer the patient to other services if necessary. The general practice maintains records of the check on its patient management system. The general practices send a minimum dataset collected as part of this check to the programme administrator.
- Secondly, the DHB ensures that there are registers of data from the free annual checks (the diabetes registers, maintained by programme administrators). This information is used to improve the quality of diabetes care by giving feedback to general practices. Aggregated diabetes data is also reported to the LDT.
- Thirdly, each LDT combines all the information received from programme administrators and collects information from hospital and non-hospital specialist diabetes services. It analyses the information, develops recommendations for service improvements, prepares an annual report, and sends it to the DHB and the Ministry.
- Fourthly, the DHB considers the LDT report recommendations when planning diabetes services.
2.33
In addition to the data provided from the free annual check, the diabetes
retinopathy eye screening service, and all hospital- and non-hospital-based
specialist diabetes services, should provide feedback to the referring GP and
should also provide information to the LDT.
2.34
The information flows are shown in Figure 2.
Figure 2
Information flows among the key stakeholders involved in diabetes care
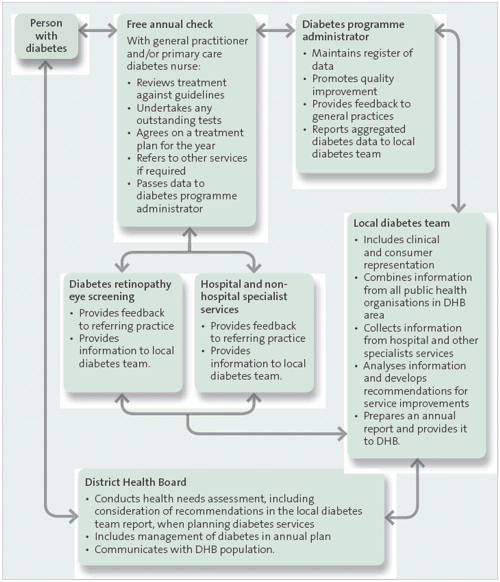
Source: Adapted from the New Zealand Health Strategy’s DHB Toolkit: Diabetes (2003).
The “Get Checked” programme in relation to other services
2.35
The 1997 Diabetes Strategy recommended that team-delivered care for people
with diabetes be developed by integrating primary and secondary diabetes
services. It recommended developing patient-based diabetes services with
enhanced co-ordination and improved access (for example, teams consisting of
the GP, dietician, diabetes nurse specialist, diabetologist, podiatrist, psychologist,
social worker, urologist, ophthalmologist,19 and community educators).
2.36
Quality diabetes care needs an integrated approach involving the patient, the
patient’s family/whānau, and health workers in both primary and secondary care.
2.37
This team relationship is set out in Figure 3.
Figure 3
Relationship between providers
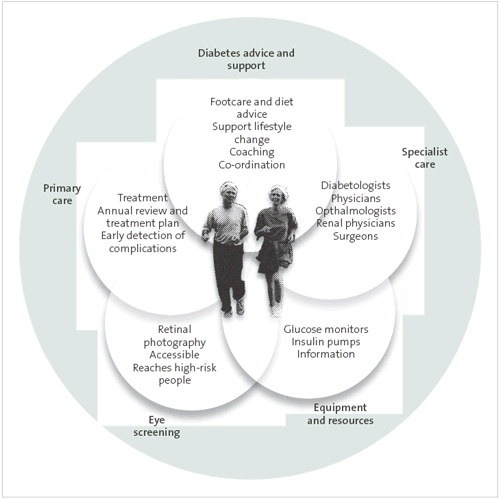
Source: Adapted from Diabetes 2000
2.38
The free annual check is an integral part of the work of primary care in diabetes
management.
The “Get Checked” programme in relation to other chronic care programmes
2.39
Diabetes is a chronic condition.20 The National Health Committee has recently
released a report which “sets out the need for a comprehensive approach to addressing the needs of people with chronic conditions in New Zealand”. 21
2.40
During our audit, we noted that three other programmes were being used with
the free annual check to assist people who needed to visit their GP or diabetes
nurse more often because their diabetes was more complex. Two of these
– Services to Improve Access and Care Plus – are national initiatives, and one
– Chronic Care Management – is a local initiative. They all aim to increase access
to health services to reduce inequalities and address chronic conditions.
2.41
Funding from Services to Improve Access enables PHOs and community groups
to use innovative approaches to reaching people with high health needs. The initiatives include providing outreach services from a bus, arranging transport
for appointments, and providing services in community venues such as marae,
schools, or workplaces.
2.42
The Care Plus programme is a Ministry of Health initiative set up on 1 July 2004
and offered through PHOs. It is intended to provide co-ordination of care for
people with chronic conditions and more complex needs. It is offered to people
who have been assessed by their GP or practice nurse as requiring at least two
hours of care from the primary care team over the next six months and who have
at least two chronic health conditions (which most people with complex diabetes
problems have). Care Plus provides the patient with an initial comprehensive
assessment and an individual care plan that sets goals related to health and
quality of life, with regular follow-ups. Care Plus assists patients to better
understand their conditions, and supports them in making lifestyle changes. The
services are provided at a low or reduced cost.
2.43
The third programme, the Chronic Care Management programme, is a significant
initiative within the chronic care model that Counties Manukau DHB uses as the
framework for a number of chronic conditions, including diabetes. Initiatives
within the chronic care model are determined by regional strategic priorities
and plans as well as objectives from the national health and disability strategies. Individual disease projects are aligned to the model.
2.44
The Chronic Care Management programme is available to patients who are
registered with a PHO in the Counties Manukau DHB. It is positioned as a step up
from Care Plus, and focuses on patients at high risk who require a more intensive
level of care and interaction with greater access. It aims to provide greater support
to patients to make healthy lifestyle changes. The Chronic Care Management
programme provides quarterly free visits for the patient. The free annual check
has been integrated into this programme, in that the first visit for the year is
classified as the free annual check.
1: A hormone is a chemical substance secreted by certain glands in the body, which can stimulate certain organs of the body.
2: Insulin is a hormone that helps the body use glucose (sugar) for energy. When the body cannot make enough insulin on its own, a person can inject insulin made from other sources.
3: The pancreas is a large digestive gland behind the stomach that produces insulin and assists with the breakdown of complex proteins and fats.
4: Health Funding Authority (2000), Diabetes 2000, Wellington, page 3.
5: Ministry of Health (2002), Modelling Diabetes: Forecasts to 2011, Public Health Intelligence Occasional Bulletin No. 10, page 7. The forecasts were based on epidemiological modelling. The baseline year of the model is 1996.
6: Ministry of Health (2004), A Portrait of Health: Key Results of the 2002/03 New Zealand Health Survey, Wellington, pages 66 to 67.
7: Lipid is a term for some forms of fat.
8: Public Health Group (1997), Ministry of Health, Wellington, page 11.
9: Diabetes New Zealand is a non-governmental, non-profit organisation that supports its 39 member diabetes societies and health professionals involved with diabetes.
10: Zoltán, Endre, et al. (2006), “Preventable kidney failure: The cost of diabetes neglect?”, The New Zealand Medical Journal, Vol. 119, No. 1246, Wellington.
11: Ministry of Health (2000), The New Zealand Health Strategy, Wellington.
12: Page 13.
13: Ministry of Health and District Health Boards New Zealand (2003), Wellington.
14: The requirements of the Health Information Privacy Code apply to this service. People with diabetes receiving this service should understand the purpose and use of their health information. Specific consent must be obtained from the patient to forward identifiable contact or clinical information from the PHO to other diabetes service providers.
15: Retinopathy is a disease of the small blood vessels in the retina of the eye, which, left untreated, leads to blindness.
16: High-density lipoproteins (HDL) form a class of lipoproteins that carry cholesterol from the body’s tissues to the liver. They are sometimes called “good cholesterol”.
17: Diabetic nephropathy is the kidney disease that occurs as a result of diabetes. It is caused by damage to the small blood vessels or to the units in the kidneys that clean the blood. It begins with protein appearing in the urine and over 5 to 10 years can develop to a stage where the kidneys are unable to remove toxins from the blood and to end-stage kidney disease. The disease is more likely to occur if blood sugar is poorly controlled.
18: Page 13.
19: A diabetologist is a physician in internal medicine trained in diabetes; a podiatrist is a trained health professional who treats and takes care of people’s feet; a urologist is a surgeon who specialises in surgery of the urinary tract; and an ophthalmologist is a doctor who sees and treats people with eye problems or diseases.
20: A chronic condition is any ongoing, long-term or recurring condition that can have a significant effect on people’s lives. Disabilities are not included in this definition, although many people with a disability have one or more chronic conditions and they are sometimes causally linked.
21: National Health Committee (2007), Meeting the needs of people with chronic conditions – Hāpai te whānau mo ake ake tonu, Wellington, page 1.
page top
