Part 4: Case Management at Branches
- Introduction
- Resources
- The Individual Rehabilitation Plan
- Vocational independence
- Measurement and monitoring of branch performance
- File review and audit
- Catalyst Injury Management Limited
Introduction
4.1
Case management at ACC branches involves many internal elements, and is
subject to many external influences on its quality – such as the performance of
health service providers, and case manager interaction with claimants and their
employers.
4.2
In this part, we discuss six aspects of case management at ACC branches:
- resources;
- the Individual Rehabilitation Plan;
- vocational independence;
- measurement and monitoring of branch performance;
- file review and audit; and
- Catalyst Injury Management Limited.
Resources
4.3
ACC provides case managers with a range of resources, including:
- information systems;
- key support staff; and
- safety measures.
Information Systems
4.4
A comprehensive range of accessible and reliable tools is available to assist case
managers in their work, and to help them to be consistent in their application of
case management practices on a national basis. The tools include:
- an on-line policy and procedures manual, Informe;
- ACC’s registration system, Pathway;
- a statistical data collection system, Data Warehouse;
- the Medical Disability Advisor computer program;
- an on-line interview tool, Scripting; and
- a national helpdesk.
4.5
The most comprehensive resource available to case managers is ACC’s on-line
policy and procedures manual, Informe. Informe was created in 1992 as a
manual that could be easily accessed by ACC staff, and now contains about
50,000 pages of information on:
- ACC guidelines and interpretation of legislation;
- ACC policies, procedures, and processes;
- definitions and examples;
- payment calculation methods;
- legislation and regulations from 1992 to 2001;
- lists of contracted health service providers;
- links to standard ACC forms, letters, and fact sheets; and
- guidance for making decisions regarding cover and entitlements, making payments and payment-related decisions, and managing claims.
4.6
ACC identifies proficiency in the use of Informe as a crucial first step in staff
induction. New case managers use Informe to learn about ACC’s policies and
procedures, and case management method. The sheer size of the system might be
daunting for new staff (and some staff criticised Informe as unwieldy and difficult
to navigate), but we found Informe to be a useful resource.
4.7
Policies are regularly updated on Informe by Head Office, and any changes are
co-ordinated there to ensure consistency. Some staff expressed concern at the
length of time between a policy change at Head Office and the formalisation of the
change on Informe. In our view, ACC’s process for policy changes is necessarily
thorough.
4.8
ACC told us that it is part-way through implementing a Standard Operating
Policies and Procedures Framework to replace Informe as the single reference site
for ACC staff. ACC says that the new on-line manual will be more user-friendly
for staff.
4.9
Another tool for case managers is the registration system, Pathway, which holds
claim information on every ACC claimant. Pathway records all payment details
and most communications between case managers and claimants, as well as other
useful information such as assessment results and medical data. The information
on Pathway is more comprehensive than ACC’s paper record.
4.10
Pathway is also valuable for ACC’s case management method, as it generates
prompts for case managers to act on particular tasks at a certain time.
These prompts help ACC to comply with deadlines for particular actions as
defined by the Act.
4.11
Case managers can use ACC’s Data Warehouse, which is a collection point for
statistical data30 from Pathway, to produce a weekly case listing report. Some case
managers told us that the report is a useful workload management tool as it
prompts them about outstanding tasks. For example, the report shows case
managers when an Individual Rehabilitation Plan is due to be placed on a
particular file in the week ahead.
4.12
We believe that the weekly case listing report is a useful tool to ensure that tasks
are completed within the periods defined by the Act and by ACC’s internal
policies. However, not all case managers are making use of the report.
| Recommendation 1 |
|---|
| We recommend that ACC promote the wider use of the case listing report by case managers. |
4.13
The Medical Disability Advisor (MDA) computer program helps to define an injury,
and predicts the length of time a person should be off work as a result,
based on statistics from the recovery times of people who have suffered the
same injury. This tool is used during the initial interview with the claimant at
the branch to establish how long the claimant should be off work (according to
the nature and extent of the injury, and the claimant’s employment31), which
provides guidelines as to when a return to work is realistic.
4.14
ACC has now introduced an on-line tool – Scripting – to the branches, to assist
case managers to obtain all necessary information (such as employer and earning
details) from a claimant during their initial interview. The initial interview is
usually the first face-to-face contact between the claimant and their case manager.
4.15
We agree with ACC’s focus on providing for structured informationgathering
at the initial interview, because this:
- facilitates an earlier start to rehabilitation through a reduction of the time taken to assess and establish entitlements (for example, weekly compensation and social rehabilitation such as home help);
- increases claimant satisfaction through quicker establishment of entitlements, and a reduction in the number of cases where entitlements are delayed because a claimant must be contacted again for further information;
- provides Head Office with assurance that case managers are obtaining essential information at the initial interview; and
- ensures consistency of practice among branches.
4.16
A national helpdesk is available to answer queries from branches that cannot be
answered at the branch. If the query has application for all of ACC, the Policy
and Assurance division at Head Office can give directions for all staff through
an update section of Informe, or through an e-mail or memo distributed
throughout the organisation.
Key Support Staff
4.17
While Informe is often the first source for case managers seeking information,
human resources are also readily available to support the case management
process – such as the:
- team manager;
- branch medical advisor;
- technical claims manager;
- case co-ordination panel;
- Pae Arahi (see paragraph 4.24 on page 60);
- Lifetime Rehabilitation Planner; and
- Head Office support divisions.
4.18
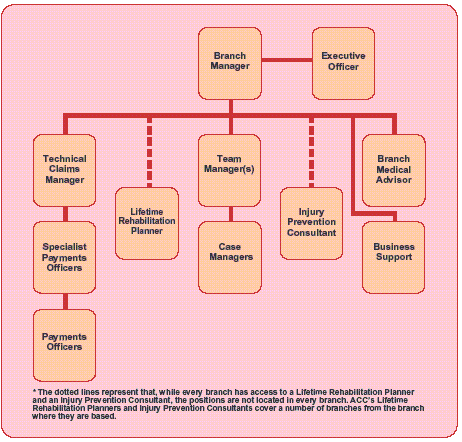
A typical ACC branch structure is shown in Figure 6 on the opposite page.
Figure 6
Staff Positions in a Typical ACC Branch Structure*
4.19
The team manager is the key support person for case managers. The team manager:
- distributes caseloads to case managers;
- helps to solve complex case management problems;
- coaches case managers;
- assists with achievement of KPIs;
- attends weekly case co-ordination panel meetings;
- reviews case managers’ files;
- assesses case managers’ performance;
- manages the induction process for new case managers; and
- reports team performance to the branch manager.
4.20
The work of case managers is also supported by branch medical advisors and
technical claims managers32. Branch medical advisors are available part-time to
offer expert advice on medical issues, approve decisions to fund various treatments
for claimants, and participate in reviews.
4.21
Technical claims managers work mainly with payments staff but generally have
a good understanding of applicable law and are able to assist case managers with
legal issues. The technical claims manager acts as an intermediary between
Head Office and branch staff to clarify the application of policy.
4.22
Technical claims managers review and approve submissions drafted by case
managers for the formal review process. Case managers can seek advice from
technical claims managers when making decisions on what treatments to make
available to a claimant. However, some branches do not have timely access to
technical claims managers.
4.23
The branch medical advisor, technical claims manager, team manager, and case
manager can also discuss difficult cases at a weekly case co-ordination panel meeting. Through this panel, a common approach to particular cases can be
agreed, which helps to ensure consistency. Once a course of action is agreed, the
case manager draws up a plan for moving the case forward. This plan is sent to
the branch medical advisor for follow-up – if required – with the case manager.
The branch manager must report to Head Office the number of cases discussed at
the case co-ordination panel every month.
4.24
Case managers also have access to one of nine Pae Arahi – Māori people who
liaise between ACC branches and the Māori community in their area. The status
of Pae Arahi in the community is such that Māori claimants feel comfortable
approaching them on ACC matters. ACC sees the Pae Arahi as a means of
facilitating contact with Māori, assisting the recruitment of Māori case managers,
and providing opportunities for ACC staff to increase their knowledge and
understanding of tikanga. The Pae Arahi advise case managers on matters of
protocol, and conduct ceremonies on ACC’s behalf.
4.25
Planning rehabilitation for serious injury claimants is not a task that case
managers necessarily have the experience, or time, to do.33 Therefore, in early
2003, ACC introduced the position of Lifetime Rehabilitation Planner. The planner
assists new serious injury claimants (such as those with head or spinal
injuries) by drawing up lifetime rehabilitation plans, and continuing to monitor
the claimant’s progress after the case is referred back to the case manager for active
management.
4.26
The planner’s role is being extended to include drawing up plans for existing
serious injury claimants. ACC says that it might take several years to create lifetime
rehabilitation plans for all serious injury claimants.
4.27
The Head Office support divisions of Policy and Assurance, Scheme Performance,
Strategy and Research, and Development are responsible for ensuring that ACC
practices are consistent with and comply with the Act and ACC policy. Staff in
these divisions can be contacted when a branch needs to address a unique or
difficult issue that could set a precedent.
Safety Measures for Case Managers
4.28
ACC operates a highly safety-conscious workplace, and takes many measures to
protect staff from dangerous situations. ACC considers that the safety of its staff is
paramount. We observed the comprehensive security measures in place for staff,
and the security-minded culture that has evolved within ACC. The health and
safety requirements of ACC branches are made clear to visitors, and ACC audits
compliance with these requirements.
4.29
The work of case managers can be difficult, and they face conflict from time to time
because of the decisions they make. Case managers that we spoke to were
generally philosophical about this aspect of their role, and said that they cope with
it well.
4.30
ACC provides case managers with access to a number of resources when dealing
with conflict. Case managers are trained in negotiation and how to deal with
high-risk claimants, and are given the opportunity for a debriefing session with
their team manager when handling a difficult case. Additionally, staff are
expected to use monthly professional supervision sessions as an opportunity to
discuss any work issues with a person who is independent of ACC. Staff can also
use the Employee Assistance Programme in regard to personal issues.
4.31
The Remote Claims Unit (the Unit) was created in 1999, and deals with claimants
whom ACC has assessed as a threat to staff safety because of staff assertions of
threatening behaviour. Sited at a secret location, the Unit deals with around 40
claims at a time. The claimants managed by the Unit cannot contact their case
managers directly but can leave a recorded message on an 0800 number.
4.32
ACC receives complaints from claimants who have been barred from their local
ACC branch and prevented from having face-to-face contact with their case
manager.
4.33
The Ombudsmen have questioned the concept of the Unit in light of complaints
from ACC claimants that they are “severely disadvantaged and are not receiving
appropriate service and care” because of a lack of face-to-face contact with their
case manager once assigned to the Unit. The Ombudsmen consider that …
the processes employed in placing some claimants in the Unit and the arrangements for
the management of their ACC business is not working satisfactorily.34
4.34
ACC responded that, while a claimant assigned to the Unit is prevented from
having face-to-face contact with their case manager, the ratio of case managers
to claimants in the Unit means that the level of service actually increases in
comparison to the branches. Nevertheless, the Ombudsmen have encouraged
ACC to review the Unit’s policies and processes. ACC’s Chief Executive has told
us that the ACC Board considered this suggestion and responded that the safety
of staff is paramount, and that the Unit should remain.
The Individual Rehabilitation Plan
4.35
The MDA computer program predicts the length of time that a person is likely
to be off work, based on statistics relating to the nature and extent of their injury.
For all claimants assessed as needing more than 13 weeks to return to work or
independence, ACC is required to prepare an Individual Rehabilitation Plan (IRP),
in consultation with the claimant.
4.36
The IRP sets rehabilitation goals to be achieved progressively by the claimant,
with the aim of restoring their health, independence, and participation to the
maximum practical extent. Each IRP includes the claimant’s medical and
occupational assessments, sequential steps for treatment and social and vocational
rehabilitation, and preparation towards the final vocational independence
assessment.
4.37
The claimant’s rights and responsibilities in regard to their own rehabilitation
are also discussed and included in the IRP. Claimants are encouraged to bring
along a support person during all discussions, especially during the preparation
and signing of the Individual Rehabilitation Plan.
4.38
Ideally, the case manager and the claimant will agree the content of the IRP,
including the proposed schedule for the claimant to return to work. However, if
the claimant refuses to agree to the IRP after a reasonable time, the Act says that
ACC may deem the IRP to be finalised. These decisions can be reviewed.
4.39
For those claims exceeding 13 weeks, the preparation and implementation of an
IRP provides impetus and structure for the rehabilitation process. However, we
found that the approach taken to prepare and confirm the IRP varies between
ACC branches. Some case managers are diligent in facilitating IRP meetings,
fully encourage the participation of the claimant, and welcome the presence of an
advocate. Other case managers prepare an IRP, and then send a letter that outlines
the contents of the plan and asks the claimant to sign a final decision letter.
4.40
The quality of the IRPs prepared by case managers also varies between branches.
We saw examples of plans that complied with timeliness requirements under the
Act and ACC policy, but compromised quality because they were produced in
haste to make the deadline. We also found instances where the content in IRPs
appeared to have been copied, with little to differentiate them in detail from other
plans. They may have been produced this way to ensure that they met timeliness
requirements. In our view, for reasons of consistency and claimant satisfaction,
ACC needs to ensure that all IRPs have regard for the claimant’s individual
rehabilitation needs.
| Recommendation 2 |
|---|
| We recommend that ACC ensure that all case managers tailor the content of each Individual Rehabilitation Plan to the claimant’s rehabilitation needs. |
4.41
A case manager’s caseload could affect the quality of the IRP (along with other
case management tasks) and the quality of the explanation of the plan’s purpose
and content to claimants. However, we did not try to establish whether a link
exists between a high caseload and poor-quality IRPs.
4.42
We understand that ACC is comfortable with the present average caseload for its
case managers, which in November 2003 stood at 78 “active” claims (those that
have received payment within the last 35 days). However, we share ACC’s
concern that caseloads vary between branches (the range in November 2003 was
65 to 109 cases per case manager). ACC should continue efforts to resolve
caseload variations and, longer term, report caseload changes in regard to
the potential performance goal results noted in paragraph 3.17 on page 47.
4.43
Some claimants described the timing of the preparation of their IRP and the setting
of goals as being too early for them as their injury was quite new (see Part Six
for further discussion of claimant views of ACC). They considered that they were
rushed into agreeing to an IRP so that a date could be set for them to return to
work.
4.44
Other claimants found the preparation of the IRP difficult to understand, and
thought that their case manager found it hard to explain all of the details to them.
They said that case managers were often in a hurry and gave out information
in brochures rather than taking the time to explain in detail the content and
stages shown in the IRP.
4.45
Although an IRP is to be planned and agreed between the case manager and the
claimant, some claimants we spoke to considered that it was often prepared
without consultation and with no consideration for them personally. It was
also sometimes offered on a “take it or leave it” basis, along with a reference to
the statutory consequences of non-compliance with ACC directions.
4.46
The content and goals to be achieved within the IRP need to be reviewed and
updated from time to time as rehabilitation progresses, and the case manager
has responsibility for contacting the claimant when necessary. We found that
branches had different approaches to the means of contact, such as by telephone
or through face-to-face meetings.
4.47
Despite the requirement that IRPs must be prepared within 13 weeks, we
consider that more time and care should be given to the understanding of
individual claimants – especially when they are first injured. In our view, case
managers may concentrate more on processing IRPs to satisfy branch targets
than allowing time for claimants to fully discuss and know how the rehabilitation
process will assist their recovery.
4.48
In our view, the planning and content of the IRPs sometimes requires more
discussion with the claimant so that the claimant has a clearer understanding of
their goals, rights, and responsibilities before they sign the plan. This discussion
will help to ensure that the IRP has direct relevance to the claimant’s treatment
and rehabilitation needs.
| Recommendation 3 |
|---|
| We recommend that ACC case managers make sure that a claimant fully understands their goals, rights, and responsibilities before the claimant is asked to sign the Individual Rehabilitation Plan. |
4.49
The Act requires ACC to prepare an IRP for all claimants whose case will take
more than 13 weeks to resolve. Despite this statutory requirement, ACC has set
a target for branches of 90% compliance.
4.50
Recent reports on branch performance show that more than three-quarters of
branches meet the 90% target, while the lowest level of compliance recorded was
67%.
4.51
ACC asserts that 100% compliance with the statutory requirement is not possible
because, for example, a claimant who returned to work may have their claim
reactivated at a later date for surgery.
4.52
ACC’s 90% target is not consistent with the statutory requirement, which (in our
view) contemplates no exceptions to full compliance.
Vocational Independence
4.53
Vocational independence means that a claimant has the capacity to engage in
work for which they are suited (by reason of experience, education, or training)
for at least 35 hours a week.
4.54
The Act prescribes a detailed process for ACC to assess whether a claimant is able
to return to full-time work or independence. If, at the end of the process, they
are considered to be rehabilitated, they are required to leave the accident
compensation scheme. Three months after a claimant is determined to have
vocational independence, their entitlement to weekly compensation ceases.
4.55
Before ACC undertakes the final vocational independence assessments, the
claimant will already have undertaken initial occupational and medical
assessments (which determine their suitability to undertake vocational
rehabilitation), and will then have completed a course of vocational rehabilitation.
4.56
Accordingly, if communicated properly to the claimant, ACC’s decision to
undertake the vocational independence assessments should not be a surprise.
These assessments occur at the end of a long and rigorous process, which is
detailed in the Individual Rehabilitation Plan. Despite this, some claimants
commented that they had received notice of appointments for assessments
before ACC told them that they were candidates for the vocational independence
process.
4.57
Case managers do not make the key decisions about vocational independence.
Rather, they co-ordinate the process and ensure compliance with all procedural
requirements. The determination of vocational independence is based on two
independent assessments. They are:
- an occupational assessment – to consider the progress and outcomes of vocational rehabilitation, and to consider whether the types of work previously identified in the Individual Rehabilitation Plan remain suitable for the claimant; and
- a medical assessment – to assess whether, having regard to the claimant’s injury, the claimant has the capacity to undertake the work identified in the occupational assessment.
4.58
These assessments are conducted by appropriately qualified and experienced
professionals. The assessors meet – separately – with the claimant, and are different
to the assessors who conducted the initial occupational and medical assessments.
4.59
Some claimants are suspicious of the people whom ACC uses to conduct these
assessments, particularly the medical assessment. They think ACC selects people
who are likely to make judgements biased against the claimant. However, we saw
no evidence of this, and claimants have the opportunity to participate in the choice
of assessor.
4.60
There are good reasons why ACC has access to a relatively small pool of
professionals who are qualified to carry out these assessments, because:
- An assessment needs to be carried out by a person with the necessary qualifications and experience. The Act imposes specific requirements about whom ACC may use. We were satisfied that ACC’s processes for selecting and training occupational and medical assessors were sound.
- The assessment needs to be carried out by someone who is independent of the claimant. For example, an assessment could not be carried out by a person who also provides medical advice and treatment to that claimant.
4.61
The Act specifies in detail the requirements for managing the vocational
independence process. Our file reviews showed that case managers follow the
required procedures carefully and methodically, with their decisions on vocational
independence requiring sign-off by their branch medical advisor and team
manager.
4.62
Frequently, the determination depends on a difficult medical judgement, which can
be (and often is) later closely scrutinised at a review hearing. These decisions can
be overturned on review. Overall, however, we found no evidence that ACC was
selecting claimants that were unsuitable for the vocational independence process,
or that it was making decisions that were not in accordance with the law.
4.63
The vocational independence process can be discomforting for claimants,
especially if they have been on the accident compensation scheme for years.
Often, they may not have been actively case-managed in the past, and do not
see rehabilitation as a realistic goal. Furthermore, they may have no job to return
to. In addition, the prescriptive nature of the process makes some claimants feel
that ACC lacks empathy for their individual circumstances. For these reasons,
claimants are often reluctant to participate in the process, and are unhappy if they
are ultimately determined to have vocational independence.
4.64
However, under the Act, ACC has a responsibility to direct claimants through the
vocational independence process if it considers that the claimant’s injury has
recovered sufficiently for them to return to work.
Measurement and Monitoring of Branch Performance
Branch Key Performance Indicators
4.65
Branch performance is regularly measured, monitored and ranked according to a
range of key performance indicators (KPIs) that are set annually by Head Office,
such as payment timeliness and a claimant’s duration on the accident
compensation scheme against the MDA’s assessment of the claimant’s
maximum amount of time off work (see paragraph 4.13 on page 57).
4.66
ACC’s KPIs are a mixture of quantitative and qualititative measures. For example,
the number of IRPs on files at 13 weeks is a quantitative measure, while claimant
satisfaction is a qualitative measure. Branches are measured against an extensive
list of KPIs, not all of which are included in the Annual Report. ACC generally
does a good job of reporting statistics in relation to rehabilitation, though it should
include more KPIs relating to the quality of claimant outcomes, such as the rate of reactivated claims. While not a perfect measure of the quality of the
rehabilitation (because some claims will reactivate on the basis of payment for a
single treatment) the measure would help ACC to identify common reasons
behind the reactivations of more long-term claims of claimants who had previously
left the scheme because they had been rehabilitated.
| Recommendation 4 |
|---|
| We recommend that ACC include more KPIs relating to the quality of claimant outcomes, such as the rate of reactivated claims, in its Annual Report. |
4.67
ACC does not rate each KPI at the same level of importance – rather, each KPI
is given a different level of emphasis depending on ACC’s priorities in its
Business Plan for the year ahead. For example, in 2003-04 an ACC priority is
increasing claimant satisfaction rates, so the weighting given to the related KPI
is higher than it was in 2002-03. The 2002-03 KPIs included reducing long-term
claims and producing Individual Rehabilitation Plans for claimants already in the
system. We agree that periodically changing the relative importance of KPIs is
a good way to get branches to concentrate on priority areas as KPIs are an
important business impetus to improve service delivery.
4.68
Head Office sends a weekly report on branch performance against the KPIs to
each branch manager.
4.69
Information in the branch performance reports allows Head Office to rank
branches, which are then told how they compare with other branches. These results
are important to branch managers because their performance is assessed mainly
on how their branch performs against the KPIs.
4.70
The General Manager for the branches seeks explanations from the Area Managers
for any variations noted in the reports before he meets with the Chief Executive at
the end of every week. Branch managers of poorly performing branches are then
asked what strategies they have in place to improve performance.
4.71
If this approach is unsuccessful, Head Office can then send a troubleshooting team
in an attempt to rectify the situation. ACC has two mobile teams – one specialising
in case management (with one case manager based in Auckland, and another
in Hawke’s Bay), and the other dealing with branch compliance with the financial
control objectives set by Head Office. ACC also sends highly performing team
managers to struggling branches in an attempt to raise that branch’s performance.
4.72
Despite these measures, there remains a considerable variation in branch
performance against the targets. Some staff explain the variation in performance
as being the result of the different knowledge bases and levels of experience of
staff within different branches. We support that view, as we found that those
branches with a stable workforce and experienced staff tended to be the better
performers.
4.73
Some staff suggested that a way of resolving the variation in branch performance
would be to make an allowance for the combined experience of a branch’s staff
when setting KPIs. In our view, it would be difficult to create a fair and
transparent system for making such an allowance.
File Review and Audit
4.74
ACC operates a multi-tiered quality assurance system, which covers both formal
file reviews by team managers and formal audits conducted by Risk and
Assurance (a section of the Policy and Assurance division) at Head Office.
Branch File Reviews
4.75
Through their file reviews, team managers look at entitlement decisions, and the
quality of material such as Individual Rehabilitation Plans, to determine whether
the decisions and material comply with legislation (for example, that IRPs were
negotiated between the case manager and the claimant, and were on the file
within 13 weeks of ACC accepting cover for the claim).
4.76
When a file for a claimant who has received weekly entitlement payments is closed,
an audit form is filled out to ensure that specified documents are on the file, such
as some form of identification for the claimant (which Head Office has found to be
missing from files in the past). Branches use the audit form as a means of
identifying and addressing any deficiencies in practice before the file is reviewed
by Risk and Assurance.
4.77
ACC, through performance agreements, expects its team managers to review their
case managers’ files on a monthly basis, but we were told that sometimes the files
are not reviewed because of other work priorities. These reviews are important
because they:
- assist the team manager to identify areas where coaching may assist a case manager’s performance; and
- allow the team manager to intervene where case managers have acted contrary to the Act or ACC policy, such as in their communication with claimants.
| Recommendation 5 |
|---|
| We recommend that ACC ensure that team manager file reviews are completed in accordance with the team manager’s performance agreement. |
4.78
The Scheme Performance division at Head Office occasionally asks for completed
file audits to check the quality of the file and the decisions made by the case
manager.
4.79
When requested (about twice a year for each team manager), team managers send
to Scheme Performance an example of a review they have completed of a case
manager’s file. Scheme Performance checks both the paper file and the electronic
Pathway files relating to the case, and considers issues such as effective
information and relationship management.
4.80
Scheme Performance then provides feedback on the team manager’s review and
gives the team manager an opportunity to respond. These checks aim to ensure
a consistent standard of review between team managers in the branches.
Head Office Audit of Branches
4.81
Internal audit is conducted by Risk and Assurance to independently review
internal controls for compliance with ACC policy, and to map progress towards
achieving ACC’s business and service goals.
4.82
Risk and Assurance prepares a business plan and an audit plan, and submits a
quarterly report to the Chief Executive based on a summary of the audits
conducted and any significant findings.
4.83
The internal audit plan for branches targets rehabilitation services based on risk,
and schedules an annual visit to most branches. Risk and Assurance audits
compliance with an audit handbook that it produced as a guide for branch
managers and their staff.
4.84
One example of a Risk and Assurance audit is the Financial Control Health Audit,
which assesses branch compliance against 61 specific control objectives. The control
(or business) objectives are given a different weighting depending on the risk to
ACC of getting the particular process wrong – for example, the objective for
legislative requirements/entitlements is weighted at 12%.
4.85
Branches are audited on case management, with a 90% target for compliance
against Financial Control Health Audit objectives. The target for the Risk and
Assurance audits has been deliberately set high in line with ACC’s focus on
compliance and continuous improvement. Both the Risk and Assurance Manager
and the General Manager for the branches acknowledge that 90% is difficult to
achieve. Only a small number of branches have consistently achieved 90%
compliance with the Financial Control Health Audits.
4.86
The achievements of each branch against the objectives are reported back to an
Audit Committee (a sub-committee of the Board), which meets quarterly.
The committee’s membership includes independent directors and the Chief
Executive.
4.87
Risk and Assurance can also undertake special audit projects aimed at providing
assurance to management on the effectiveness of specific operations. These
effectiveness audits are listed in the annual internal audit plan, and may include
audits of:
- the content of assessment reports received by case managers;
- a new service, such as lifetime rehabilitation planning; or
- coaching, which ACC uses to improve case manager performance.
4.88
Risk and Assurance’s scheduled internal audits of files and branch practices are
regular and detailed, and set demanding standards. We encourage ACC’s
emphasis on continuous improvement of branch compliance with Head Office
standards.
4.89
As well as scheduled audits, the Chief Executive has the discretion to fund
additional audits on risk areas as they arise. Effectiveness audits are an
extremely useful tool to identify areas where ACC’s case management practices
can be improved.
Catalyst Injury Management Limited
Background
4.90
Catalyst Injury Management Limited (Catalyst)35 is a wholly owned subsidiary of
ACC, established in 1998. On 1 September 2003, ACC announced that Catalyst’s
long-term case management function would be given to new Long Term Claims
Units within ACC. Catalyst continues to provide other services (such as case
management of short-term claims for private organisations) that we excluded
from the scope of this audit.
4.91
Until September 2003, Catalyst managed long-term claimants specifically
selected from branches, and progressed each claimant through the Individual
Rehabilitation Plan until the claimant was assessed as being vocationally
independent. Claims were selected on the basis that Catalyst expected the
claimants to leave the accident compensation scheme within 12-15 months.
4.92
At the time of our field work, Catalyst had three offices situated in Auckland,
Wellington, and Christchurch to process claimants through vocational
rehabilitation. Of about 14,000 long-term claimants receiving assistance from
ACC, around 3000 were assigned to Catalyst and were under active management.
4.93
Catalyst’s case managers concentrated on the benefits of rehabilitation for
claimants, and were expected to demonstrate the principles contained in the Code
of ACC Claimants’ Rights in their contact with claimants. Catalyst’s case
management practices also had to comply with the Act.
4.94
One of Catalyst’s business goals was to return 2000 long-term claimants to
independence during the 2002-03 financial year. In its 2002-03 Business Plan,
Catalyst adopted several strategies in key areas to assist with meeting the
performance targets for the rehabilitation of long-term claimants. They included:
- introducing individual performance targets for case managers;
- maintaining a minimum of 55 case managers;
- providing correct and timely payments to claimants; and
- 70% of Catalyst decisions being upheld at review.
4.95
Catalyst had access to and used the same systems and resources that are available
to ACC case managers – including Pathway, Informe, and the ACC intranet.
They used similar case management practices to branches, but each Catalyst case
manager had a target of a specified number of claimants leaving the scheme each
month.
4.96
Catalyst case managers needed to have additional skills to those of their branch
counterparts (see paragraph 5.35 on page 85), as their claimants often had other
issues to those managed at branches because of the length of time they had
received assistance from ACC.
Catalyst’s Selection and Transfer of Files
4.97
Catalyst initially selected files based on the information contained in the paper
files, without reference to the more complete information on Pathway.
4.98
Many files that Catalyst initially selected were found to be inappropriate for
its attention, and were returned to branches. This caused disruption for
branches and claimants because relationships needed to be rebuilt. Subsequently,
ACC and Catalyst agreed that all files that were returned to a branch required the
mutual consent of Catalyst and the branch.
4.99
In addition, Catalyst implemented new criteria to select claimant files from
branches. To be selected by Catalyst, claimants had to:
- be in receipt of weekly compensation;
- require ACC assistance for more than 52 weeks;
- have a capacity to leave the accident compensation scheme in 12-15 months;
- be under 60 years of age; and
- have a recent medical report indicating a probable capacity to work and, ideally, initial occupational and medical assessments.
4.100
Catalyst did not accept claims that were registered as sensitive or risky, or those
that involved claimants who were alcohol and/or drug dependent, or were
under a fraud investigation.
4.101
The transfer of claims to Catalyst caused unease for some claimants. Some
claimants suggested that they were not properly advised of the transfer of their
file from the branch to Catalyst. Now that Catalyst long-term claims are to be
returned to ACC, ACC should communicate closely with claimants during the
handover process.
Catalyst Case Management
4.102
Catalyst case managers were aware that their decisions were constantly under
scrutiny, as a result of intense media interest in Catalyst. They described their case
management approach as requiring a combination of quality and speed to
achieve the targeted number of claimants leaving the scheme each month.
4.103
Claimant satisfaction with Catalyst’s service had only recently been surveyed
separately from wider satisfaction with ACC. The February-June 2003 Catalyst
Claimants Survey showed that 42% of all Catalyst claimants were dissatisfied or
very dissatisfied with their experience of the service provided by Catalyst, as
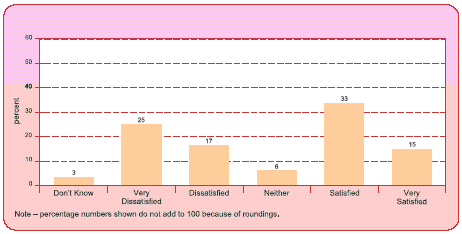
shown in Figure 7 below. This percentage is far higher than the level of
dissatisfaction with branch performance in general.
Figure 7
Claimant Satisfaction With Catalyst’s Service in General
4.104
In relation to case management, 50% of Catalyst claimants were satisfied or
very satisfied that they had received the level of service that they considered
necessary to assist their treatment and rehabilitation. This satisfaction is much
lower than that for branches.
4.105
The survey also showed that Catalyst claimants were concerned with the progress
of their rehabilitation, as only 45% felt that the details in the Individual
Rehabilitation Plans were followed. Branch claimants have expressed a similar type
of concern.
4.106
The same survey compared Catalyst claimant service performance with that of the
branches, and found that 42% of claimants felt that Catalyst’s claimant service was
worse than the service they received from ACC before their claim was transferred.
4.107
Specific issues identified by claimants in the survey included the frequent change
of Catalyst case managers, and not enough face-to-face contact and communication
with them. The rate of staff turnover in one Catalyst office was particularly high.
Catalyst attempted to address this by implementing a new person-specification
and a more comprehensive induction programme.
4.108
Catalyst claimants often require more intensive management than other
claimants, so ACC needs to take particular care to communicate with them regularly
and fully.
| Recommendation 6 |
|---|
| We recommend that ACC communicate regularly and fully with former Catalyst claimants about progress in their rehabilitation. |
4.109
ACC should make full use of the information contained in the Catalyst survey to
identify and address long-term claimants’ concerns that contributed to their
dissatisfaction with Catalyst.
4.110
Claimants often considered that Catalyst’s monitoring of their progress was
impersonal and process-bound. Monitoring is necessary to make sure that the
claimant is consistently attending all appointments, so that the original plan
containing all rehabilitation phases remains relevant. A strong ongoing relationship
between the case manager and the claimant is necessary to achieve the ultimate
goal of rehabilitation.
4.111
Attempts at establishing a strong relationship between long-term claimants and
Catalyst may have been hampered by ACC and Catalyst’s expectation that
the claimants would be vocationally independent within 12-15 months. The
pressure on case managers to have a set number of claimants leave the scheme
each month also may have affected the level of service they could provide to
each claimant.
Reviews
4.112
In contrast to the branches, each Catalyst office had a legal staff member on site
(a practice continued in the Long Term Claims Units) who:
- provided prompt input into the case management process;
- prepared submissions for reviews of Catalyst files; and
- represented ACC at the review hearings.
4.113
Catalyst also intended having in each office at least one case manager who was
skilled in managing reviews to co-ordinate the increasing volume of reviews,
conduct administrative reviews, prepare submissions, and report at hearings.
4.114
As noted in paragraph 4.94 on page 72, Catalyst had a target that 70% of its
decisions would be upheld at review. A report to the Catalyst Board for the
months of February-April 2003 showed that 76% (or 65 out of 86) of Catalyst
decisions were upheld at review. This was a high percentage for such a
contentious area, and showed that most of Catalyst’s decisions were justifiable.
30: Data is collected for:
reporting on KPIs;
injury prevention purposes, and research and policy development;
monitoring of provider performance; and
monitoring accident compensation scheme and delivery costs.
31: In the case of a broken leg, if a claimant does sedentary work then they are likely to return to work earlier than someone who does physical work.
32: The size of the branch and its functions determine the amount of time that the branch medical advisor spends at the branch, and whether the branch has a technical claims manager.
33: ACC has moved away from assigning work to teams based on the nature of the claim, such as serious injury claims.
34: Office of the Ombudsmen Annual Report 2001-02, page 18.
35: As noted in the Summary, we have retained our discussions of Catalyst in this report because we consider that the lessons learned from ACC’s Catalyst experience have relevance to ACC’s future dealings with long-term claimants.
page top